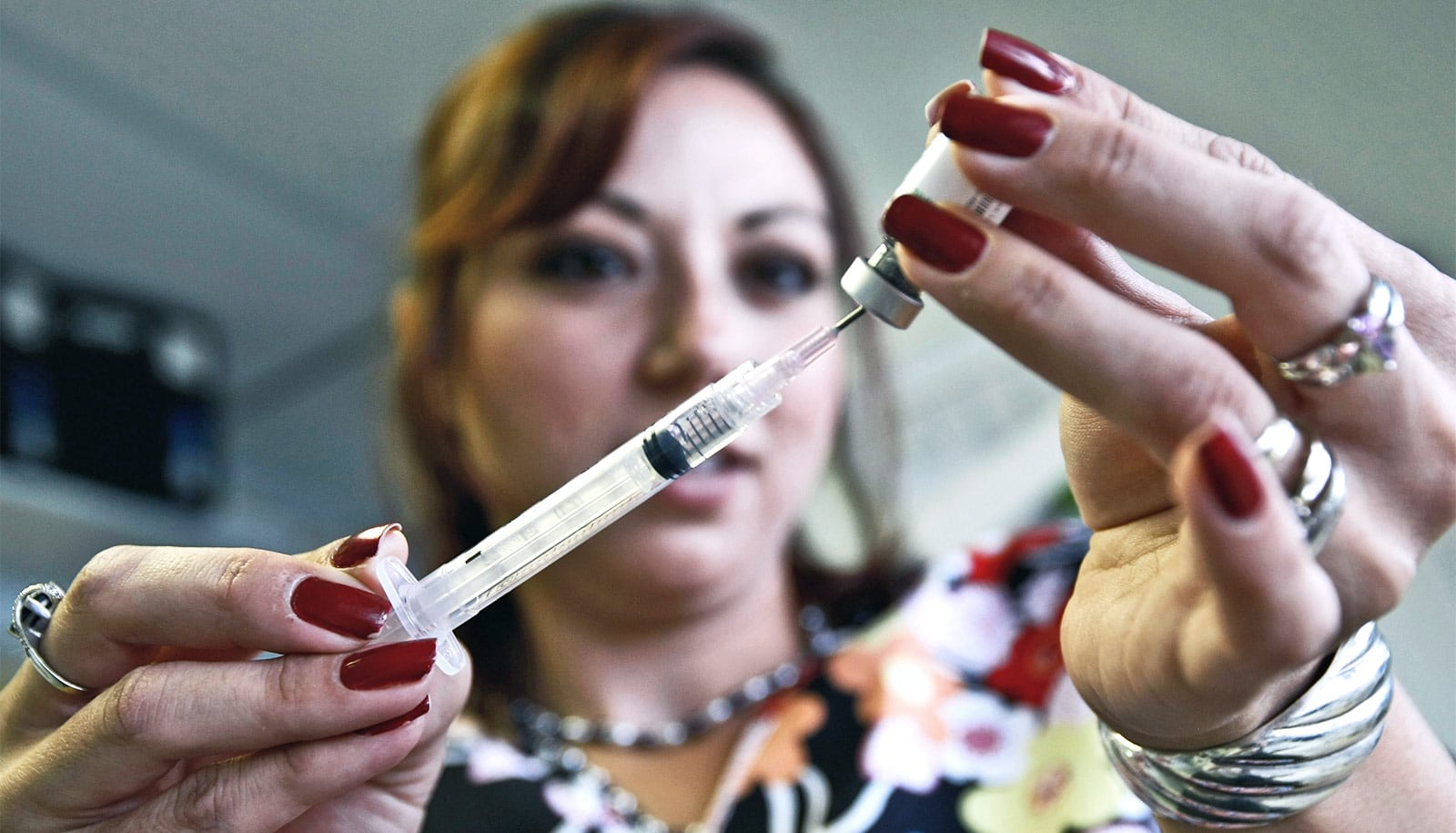
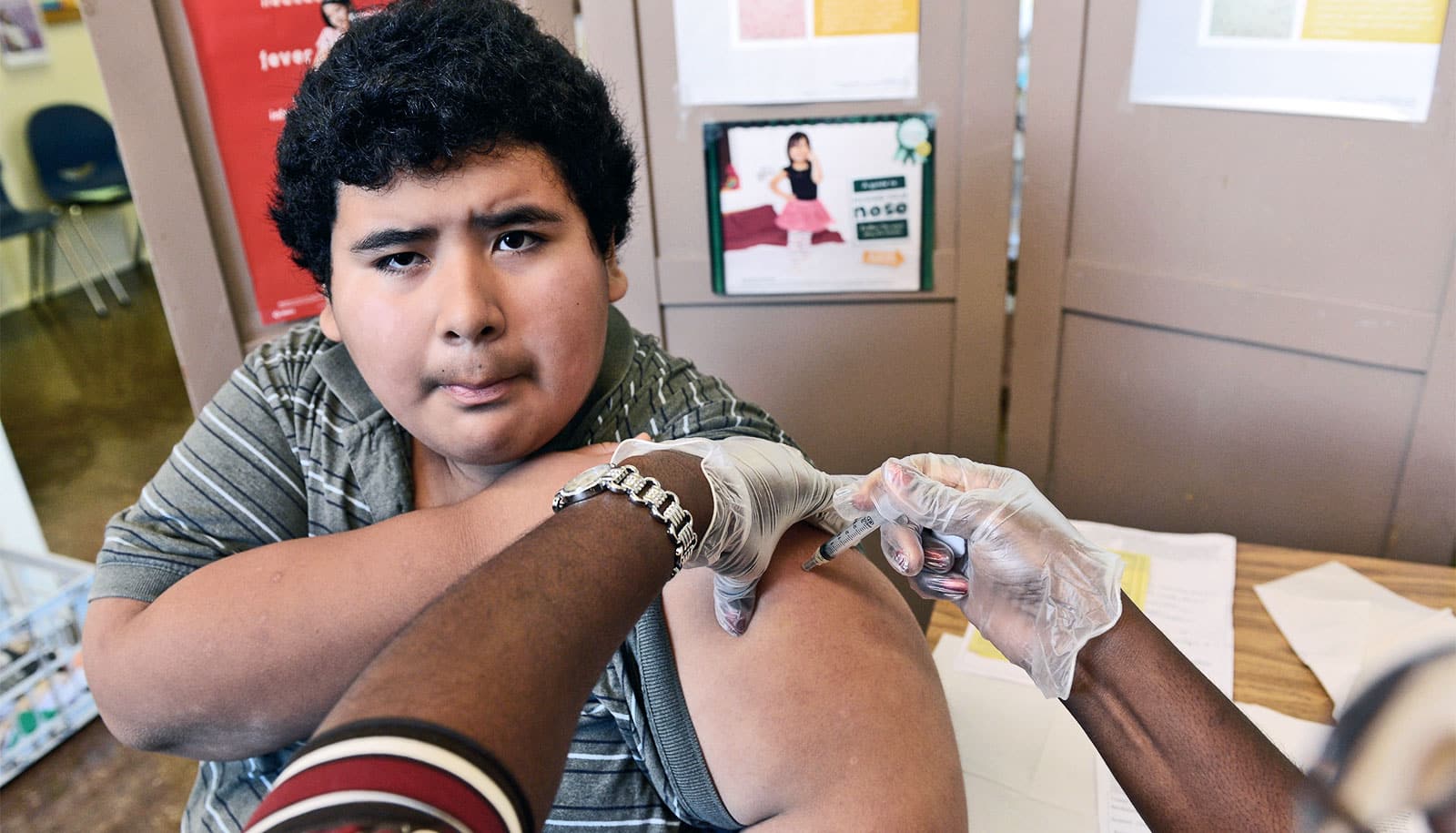
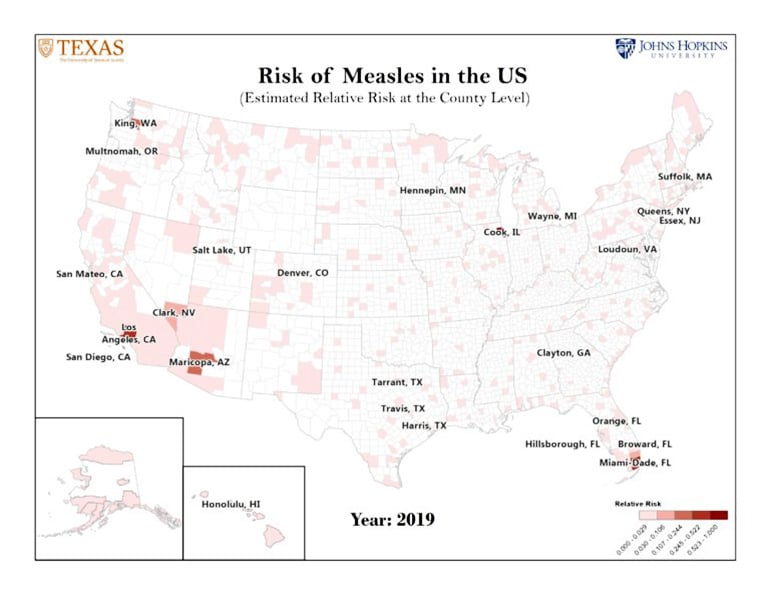
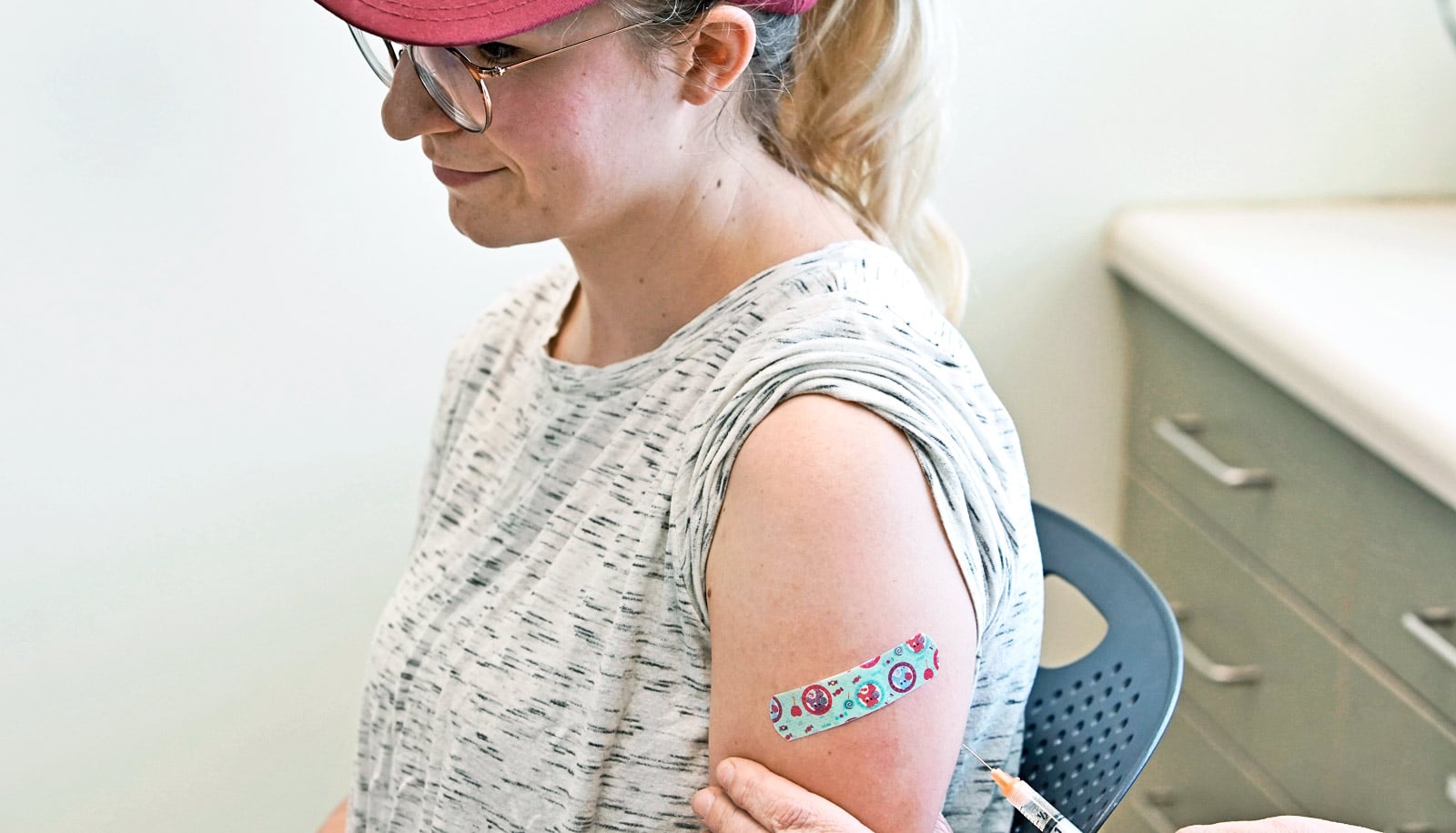A new analysis identifies the 25 United States counties most likely to experience measles outbreaks in 2019.
The analysis combined international air travel volume, non-medical exemptions from childhood vaccinations, population data, and reported measles outbreak information.
“There has been a resurgence of measles cases, among other vaccine preventable diseases, in the US and other countries in recent years. Measles, in particular, poses a serious public health threat due to the highly contagious nature of the disease. It is therefore critical that we proactively identify areas most likely to experience outbreaks to strategically target for surveillance and control,” says co-corresponding author Lauren Gardner, an associate professor of civil engineering at the Johns Hopkins University.
As of late April, the US has seen more than 700 cases of measles this year, the highest number in decades. Although measles was officially eliminated from the US in 2000, the ongoing outbreak shows that the nation remains at risk.
The recent spike in cases, the researchers say, is due to reintroduction by international travelers from countries experiencing measles outbreaks, compounded by low-vaccination rates in certain localities, which an increasingly visible anti-vaccination movement fuels.
“Anti-vaxxers are denying the best and very successful medical science we have and choosing instead to rely on fraudulent claims, such as a purported link to autism, that have been uniformly debunked by evidence and analysis over the last two decades,” says the study’s other corresponding author, Sahotra Sarkar, professor of philosophy and integrative biology at the University of Texas at Austin.
To identify the top 25 US counties most likely to experience outbreaks in 2019, the research team performed a risk analysis that took the following data into account: non-medical exemption rates in each county, anonymous full-route passenger travel data from all international airports into each of the US counties, county population, and size and location of measles outbreaks globally.
The analysis correctly predicts the regions in Washington, Oregon, and New York that have already seen major measles outbreaks this year. Furthermore, the vast majority of counties that have reported measles cases as of April 2019 are included in team’s top 25 at-risk counties or lie adjacent to one of the top 25 counties.
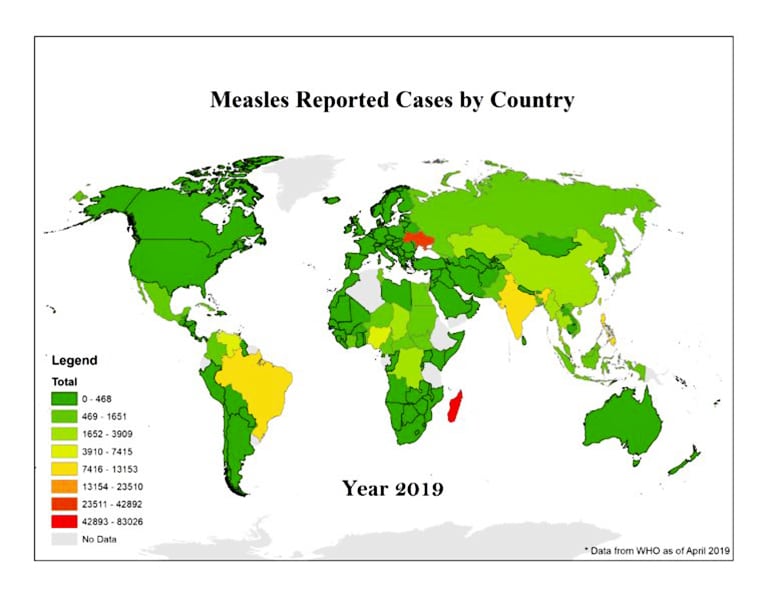
Additionally, the analysis specified the following countries that contribute most to measles risk in the US: India, China, Mexico, Japan, Ukraine, Philippines, and Thailand.
“Our prediction is aligned with multiple counties that have experienced measles outbreaks this year. Critically, we recommend that public health officials and policymakers prioritize monitoring the counties we identify to be at high risk that have not yet reported cases, especially those that lie adjacent to counties with ongoing outbreaks and those that house large international airports,” says Gardner.
Sarkar adds that policymakers must focus on centers of vaccination resistance, as well as regions with a lot of passenger inflow from affected countries worldwide if there are even small local pockets of unvaccinated people.
“The New York borough of Brooklyn is a perfect example with a large number of unvaccinated members of an orthodox Jewish community even though the overall county vaccination rate is not low,” Sakar says.
The analysis appears in The Lancet Infectious Diseases. To see the complete list of at-risk counties, visit this interactive map.
Additional authors are from the University of New South Wales Sydney and St. Michaels Hospital in Toronto.
Source: Johns Hopkins University