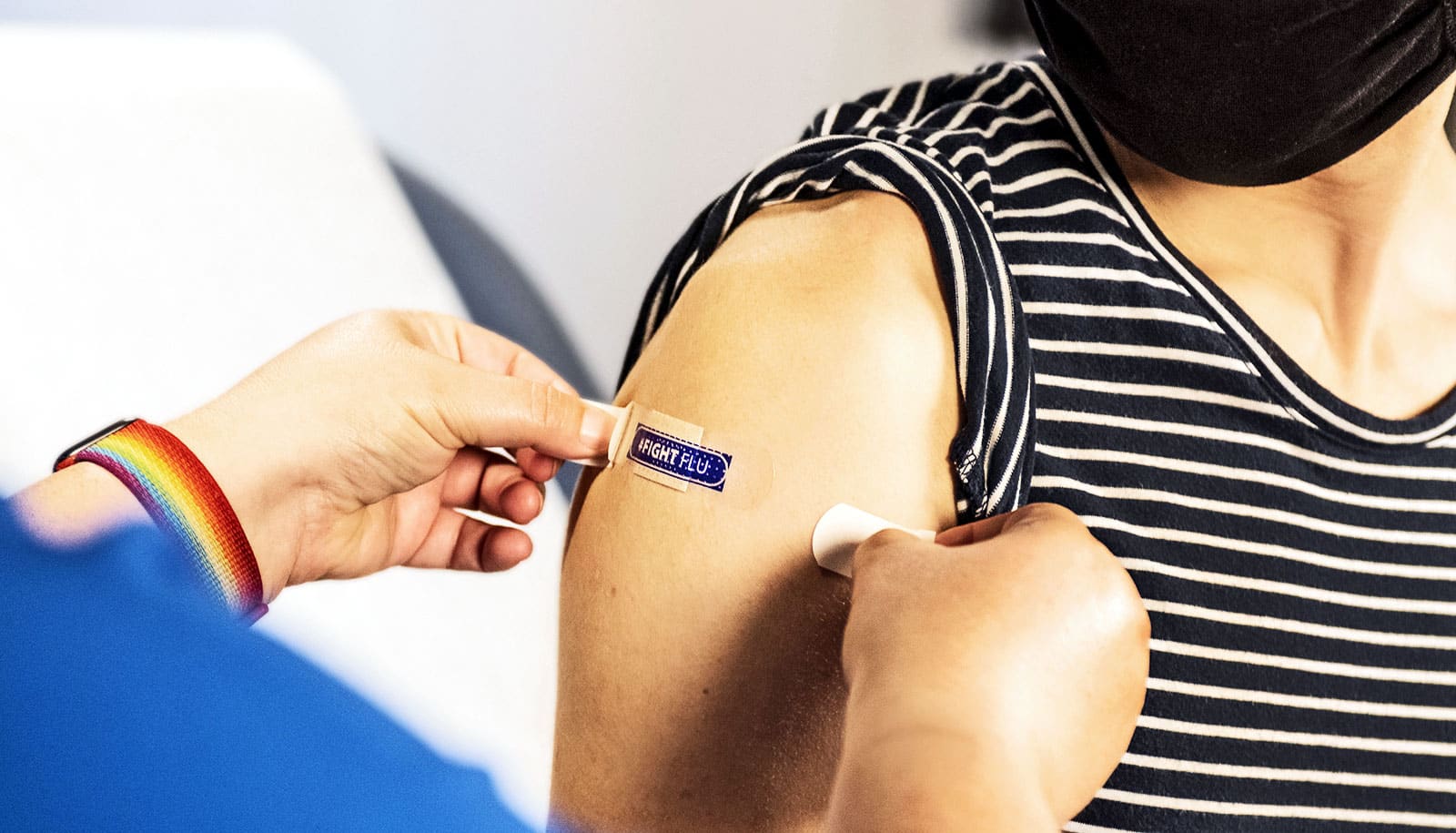
A deactivated virus can safely transplant new genes into retina cells, which may help save the eyesight of some patients with wet age-related macular degeneration.
The gene therapy, if proven effective in future larger experiments, could replace the current therapy for some patients, which requires uncomfortable eye injections six to nine times a year.
“This preliminary study is a small but promising step towards a new approach that will not only reduce doctor visits and the anxiety and discomfort associated with repeated injections in the eye, but may [also] improve long-term outcomes,” says Peter Campochiaro, professor of ophthalmology at Johns Hopkins University School of Medicine.
Wet age-related macular degeneration is an advanced form of AMD, affecting an estimated 1.6 million Americans. It accounts for only 10 to 15 percent of total age-related macular degeneration cases but about 90 percent of AMD-related severe vision loss, according to the Macular Degeneration Partnership.
It involves the growth of abnormal blood vessels that leak fluid into the central portion of the retina called the macula, which we use for reading, driving, and recognizing faces.
Can vitamin D prevent macular degeneration?
The study, published in the journal the Lancet, reports a new treatment approach in which a virus, similar to the common cold but altered in the lab so it can’t cause disease, is used as a carrier for a gene and is injected into the eye. The virus penetrates retinal cells and deposits the gene, which turns the cells into factories for a protein that shuts down formation of the abnormal blood vessels.
The standard treatment today requires injections of the protein directly into the eye—which reduces fluid in the macula and improves vision, but proteins gradually exit the eye and another injection is usually needed every six to eight weeks. Because of the time burden and discomfort, many patients don’t get injections as often as needed, causing vision loss.
Researchers conducted a phase 1 clinical trial of their gene therapy approach, testing it in 19 men and women, all 50 years old or older with advanced wet AMD.
The test subjects were divided into groups that received increasingly larger doses of the virus. A test group was monitored for signs of adverse reactions for at least four weeks before researchers administered a higher dose to the next group.
After no problems arose with the three groups, the researchers administered the maximum dose to 10 participants and again observed no serious side effects.
Training restores some vision after stroke
“Even at the highest dose, the treatment was quite safe. We found there were almost no adverse reactions in our patients,” Campochiaro says.
For safety and ethical reasons, the study recruited patients for whom the standard approved treatments were highly unlikely to restore vision, so only 11 of the 19 had the potential for fluid reduction. Of those eleven, four showed dramatic improvement. The amount of fluid in their eyes dropped from severe to almost nothing, just as is observed with optimal standard treatment, Campochiaro says. Two other participants showed a partial reduction in the fluid in their eyes.
Five participants showed no reduction in fluid levels. From that result, the researchers conclude that even if further studies confirm the safety and value of their gene therapy, it may have limitations for broad use. The researchers believe that many Americans have an immunity to the virus used in the study and that, in patients with that immunity, the virus was destroyed before it could insert the therapeutic gene. More work is needed to confirm that guess, Campochiaro says.
Other researchers involved in this study were from Johns Hopkins, Ophthalmic Consultants of Boston, Retinal Consultants of Arizona, the University of Massachusetts Medical Center, and Sanofi Genzyme. Sanofi Genzyme, a company in Framingham, Massachusetts, funded the work.
Source: Johns Hopkins University