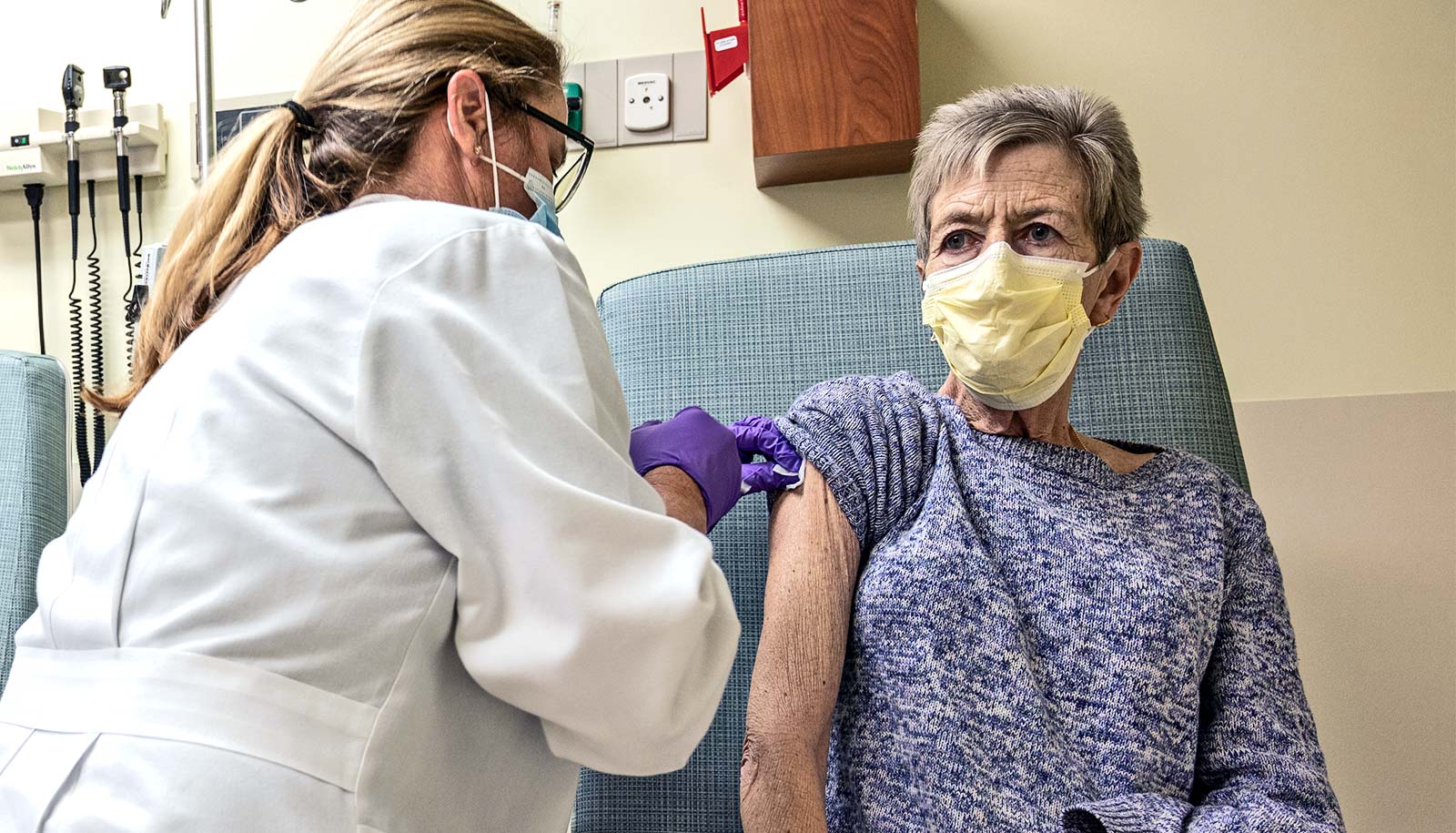
Vaccinated (but not boosted) people with cancer who have breakthrough COVID-19 infections remain at high risk for hospitalization and death, according to a new study.
The findings show that vaccinated patients who experienced breakthrough COVID-19 infections had a hospitalization rate of 65%, an ICU or mechanical ventilation rate of 19%, and a 13% death rate.
Researchers collected data for the study before booster vaccines were recommendation for patients with cancer by the US Centers for Disease Control and Prevention.
“These findings come at a time of concerns that immune escape mutants such as the Omicron strain may emerge from chronically infected patients with weakened immune systems,” says Dimitrios Farmakiotis, an associate professor of medicine at Brown University’s Warren Alpert Medical School and a senior author of the study in Annals of Oncology.
“Thus, the immunosuppressed and their close contacts should be target groups for therapeutic and preventive interventions, including community-level outreach and educational efforts.”
The COVID-19 and Cancer Consortium, a group of 129 research centers that is tracking the impact of COVID-19 on patients with cancer, conducted the study. The Lifespan Cancer Institute and partner Brown University are among the participating institutions.
Similar high COVID-19 mortality rates among fully vaccinated individuals have been reported in other immunocompromised patient populations, such as organ transplant recipients, prior to the utilization of additional vaccine doses, Farmakiotis says.
At the time the study was conducted, patients were considered fully vaccinated after having received two doses of either the Pfizer-BioNTech vaccine or the Moderna vaccine, or one dose of the Johnson & Johnson vaccine, with the last dose long enough before breakthrough COVID-19 to consider them fully vaccinated.
Researchers collected the data from November 2020 through May 2021, before booster vaccines were recommended by the CDC.
The consortium identified 1,787 patients with cancer and COVID-19 for the study, the vast majority of which were unvaccinated. The number of fully vaccinated was 54, and 46% of those fully vaccinated had reduced levels of lymphocytes—the T cells and B cells responsible for immunological responses to viruses. Lymphopenia commonly occurs in patients with cancer receiving anti-CD20 monoclonal antibodies or CAR-T-cell treatments for hematologic malignancies, including lymphoma and leukemia.
The study appears to support previous observations that patients with hematologic malignancies are at greater risk for severe outcomes from COVID-19. However, the number of patients in the study is too small to make definitive conclusions about specific types of anticancer therapies that might be associated with breakthrough infections, the researchers note. Patients on a treatment regimen of corticosteroids also appeared to be more susceptible to hospitalization.
“Because measures of immunity are not routinely collected in clinical care, we don’t know whether these were patients who mounted effective immune responses after vaccination; a lot of emerging data have suggested that patients with cancer, especially blood cancers, don’t mount adequate protective antibody responses,” says Jeremy Warner, director of the CCC19 Research Coordinating Center, associate professor at Vanderbilt-Ingram Cancer Center, and a senior author of the study.
“It’s important to note that many of the same factors that we identified prior to the availability of vaccination—age, comorbidities, performance status, and progressing cancer—still seem to drive many of the bad outcomes.”
Farmakiotis is also director of transplant and oncology infectious diseases at Rhode Island Hospital, the Lifespan Cancer Institute, and the Lifespan Cardiovascular Institute.
Additional coauthors are from Dana-Farber Cancer Institute, Vanderbilt-University Medical Center, and Brown.
Source: Brown University