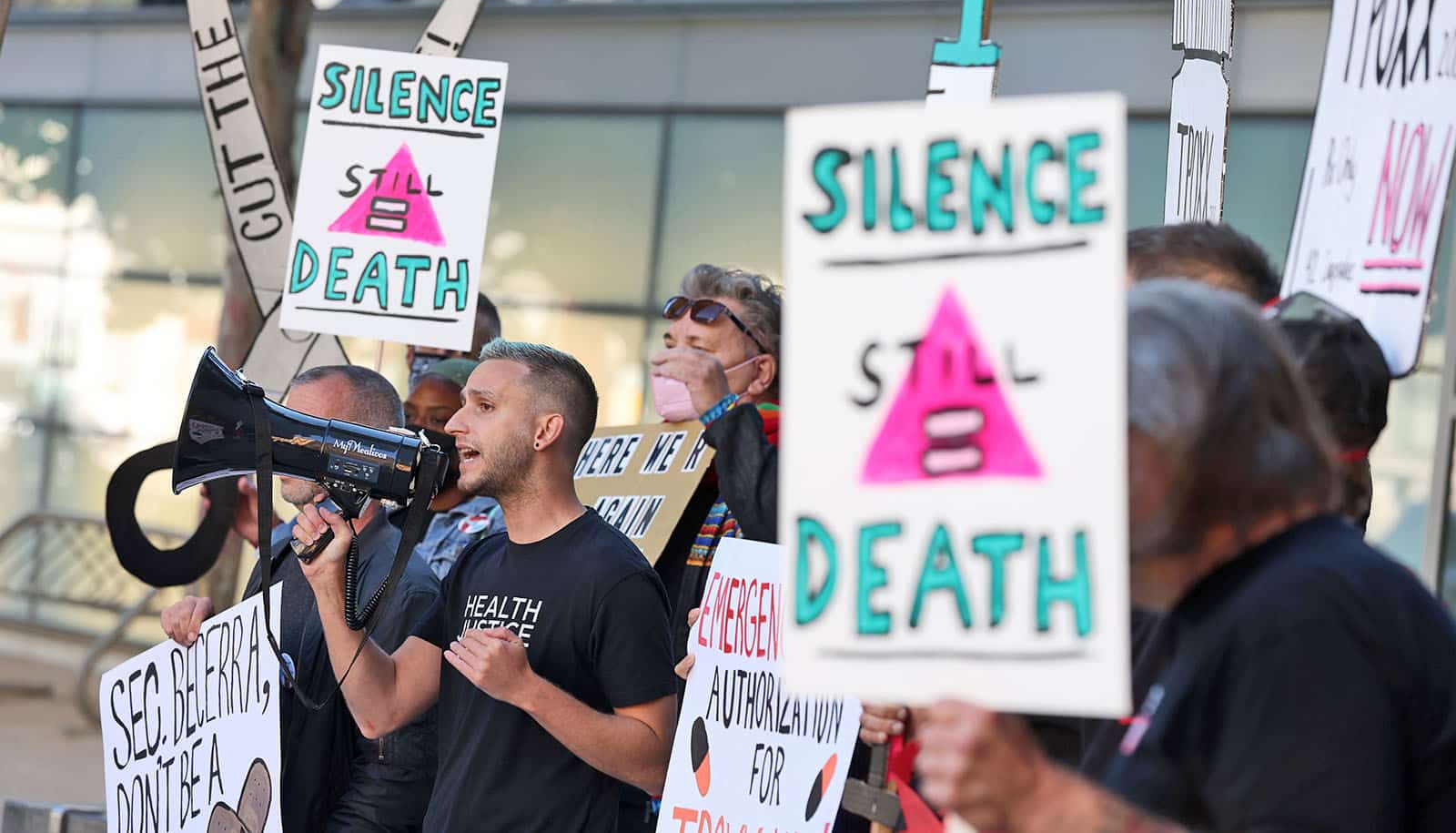COVID-19 and HIV offer lessons for the monkeypox pandemic, says microbiologist Joseph Osmundson.
Osmundson has been drawn to microbes—particularly viruses—since he was a kid, in part from growing up in the 1980s in the shadow of HIV. (“A virus with nine genes that could kill you? How could that type of mystery not astound and shock?” he explains.)
In college, he began studying the evolution of viruses like HIV, and since then has dedicated his scientific career to unraveling the mysteries of microbes. But Osmundson, now a clinical assistant professor of biology at New York University, also found that viruses are too complex to understand with science alone.
That’s where writing came in.
Osmundson had been writing about HIV for publications like The Village Voice and Guernica for years before COVID-19 hit, but the pandemic prompted a closer look at how viruses have shaped our lives.
“I needed to share what it felt like to live through this moment, this time of overlapping pandemics, as a queer scientist,” says Osmundson. “Scientists have feelings too—we are human, we live through the very things we study, and I wanted that complexity and emotionality to exist in a book full of science writing.”
The result is Virology: Essays for the Living, the Dead, and the Small Things in Between (W. W. Norton, 2022) a collection of Osmundson’s reflections on the personal, political, and scientific impact of viruses, such as SARS-CoV-2 and HIV, which became even more relevant in recent months.
Just as Virology was published in spring 2022, the US found itself facing yet another viral outbreak. Cases of monkeypox—a type of orthopoxvirus closely related to smallpox—have grown, predominantly affecting queer men and their sexual networks with painful rashes and flu-like symptoms.
In recent weeks, New York City and State, the White House, and the World Health Organization (WHO) have all declared monkeypox a public health emergency.
Here, Osmundson talks about the lessons we’ve learned from HIV and COVID-19, and how to apply them to this new public health challenge:
There’s been some debate about the name for monkeypox, and the WHO has started a process to rename it. Why is language important here?
We have to rename this virus. It is verifiably incorrect that this virus comes from monkeys in the Congo; the monkeys were in a lab in Europe. The virus was then found in rodents and humans in Central Africa. The name evokes a lot of Heart of Darkness images of Central and West Africa that do serious harm.
We need more neutral language. I’ve seen MPV and MPX and they’re both a significant improvement (I’ll call it MPV). When HIV/AIDS was called GRID—Gay-Related Immune Deficiency—the name of the virus and disease was associated with queer identity, doing harm both to gay folks who were sick by equating their identity or behavior with a disease and to folks with HIV who weren’t queer who were associated with that identity through the virus. Viruses don’t have identity! They’re just little packets of genetic information!
In the US, monkeypox is mostly spreading among gay and bisexual men and their sexual networks—a community shaped by the AIDS epidemic. Are there lessons that can be applied to monkeypox?
Of course. It’s essential, as this epidemic continues, to maintain that MPV can infect anyone. Any place where there’s a large amount of touch—sports like wrestling comes to mind—or shared tight spaces—like dorm rooms—may spread the virus. And we can’t blame this outbreak on gay men, even though we are one of the groups where the virus is spreading.
There are essential lessons from HIV that need to be applied in this crisis. With MPV, we are very lucky: we have tests, treatments, and vaccines that are FDA-approved and stockpiled. People need these tools! This was a huge lesson from HIV: After medications that worked were developed, it took a decade to ensure those drugs were available in South Africa. Still today, less than 25% of the people who qualify for HIV PrEP [a medication taken to prevent HIV] have access to the drug. The number for Black people is 8%, whereas 63% of eligible white people have access to PrEP. Biomedicine is necessary but not sufficient. People have to have access to the biomedicine, and trust that it’s designed with them in mind.
Early during the COVID-19 pandemic, the CDC infamously bungled testing by distributing flawed tests, which made it difficult to identify early cases and stem the spread of the virus. It sounds like monkeypox testing also got off to a slow start.
I co-wrote a New York Times op-ed in late May both demanding an increase in MPV testing and laying out a framework to build that capacity immediately. But, just like in the COVID-19 response, the urgency to make those changes was absent. Between June and mid-July, testing capacity in New York City—a city with a million queer people hosting Pride where hundreds of thousands more visit—was limited to under 20 MPV tests a day.
This was a choice. The lack of testing meant we were undercounting cases. The fact that we were undercounting cases led the federal government to delay the shipment of vaccines until after Pride.
Speaking of vaccines, how does vaccination work for monkeypox?
MPV should have been an easy virus to contain in the United States. We have millions of doses of two effective vaccines stockpiled. And yet, by late summer, it seems like this virus is most likely to remain in our communities for some time, if not forever.
In 1980, the WHO announced that smallpox had been eradicated from the planet. In this context, it became unethical to vaccinate widely against smallpox; this decision also impacted MPV immunity, though, since smallpox is closely related to MPV. From 1980 through 2010, MPV immunity in the region of Africa where MPV is endemic went from nearly universal to nearly non-existent. MPV outbreaks swelled. In Nigeria, from 2017 through today, there has been community spread of MPV in urban centers. We could have been vaccinating in the endemic region to prevent this spread, and if we had, we likely wouldn’t have seen the virus spread globally.
One of the frustrating things about viruses is that they’re all immensely different from one another. All living organisms, from bacteria to bears, write their genetic information in DNA. Not so with viruses. And each virus will infect a different type of cell with different types of outcomes. All of these differences make some viruses relatively prone to strong immunity from vaccines— like measles, where a vaccine is over 95% effective—and some viruses resist vaccine-based immunity altogether, like HIV.
Access to vaccines also feels reminiscent of the first COVID-19 vaccines, when booking an appointment felt like winning the lottery. You told Wired, “When there’s such scarcity, equity is impossible.” What needs to be done to improve vaccination efforts?
Global infectious diseases need global solutions. There are answers in the short, middle, and long term. For now, vaccines need to get into arms. The new CDC/FDA strategy of using one-fifth of the dose intradermally may help here, but it throws yet another variable into the question of how effective this vaccine will be in this epidemic.
Middle and long term, the world will need more MPV vaccines. Some colleagues and I argued in January 2021 that the globe deserved COVID-19 vaccines. We had momentum to get that done in the Biden administration, using the model of PEPFAR that funded HIV medications for all globally. Ultimately this didn’t happen, and SARS-CoV-2 continued to evolve and mutate, which global vaccination with the highest efficacy vaccines may have helped prevent.
HIV, COVID, and MPV show us that infectious diseases are global by their nature. MPV vaccination everywhere the virus is, and especially in the endemic region, will help prevent more painful infections and loss of life. We need to make more vaccine, and we need to move with urgency.
Harm reduction is used in public health efforts to reduce negative consequences without calling for abstinence—for instance, the use of supervised injection sites to prevent drug overdoses and encouraging “pandemic pods” during early COVID waves to allow socialization in small groups. Is there a role for harm reduction with monkeypox?
Harm reduction is the name of the game! Calls for changing sexual behavior actually came from the queer community first. Public health officials are terrified of this, but I was working with and talking to some people who host large parties, and so many people in their friend groups had MPV. They shut down voluntarily, and I’m proud of them.
So from the people most affected by MPV, we’re starting to hear that we should all maybe modify our sexual behaviors until more vaccine is available: talk to your hookups, wear more clothes at the party, avoid skin contact with large groups. Only after the community started this work did the CDC and New York City Department of Health issue the same guidance.
Look, you cannot and will not stop people from gathering or having sex, especially long term. It just won’t work. HIV research showed us this. You have to offer people information on the risk of various infections, prevention via biomedicine when we have it, and knowledge about what the infection looks like, how to get tested, and how to get treated.
Are there other lessons from COVID that can be applied to monkeypox?
We should be talking more about just how miserable it is to isolate when infected with MPV. Even for milder courses of infection, people are being asked to fully isolate at home for weeks.
COVID taught us just how painful only five to 10 days of isolation can be. Here, folks are having to isolate for twice that or more. And we haven’t built in any support—financial, practical, or emotional. We need to be supporting people during and after the infection, and working on reducing stigma for the recovered people.
You’re a co-investigator on RESPND-MI, an LGBTQ+ community-built survey of monkeypox prevalence and networks. What are you hoping to learn?
RESPND-MI is designed and led by my dear friend Keletso Makofane, a Harvard-trained epidemiologist who studies how social networks lead to different healthcare outcomes. It’s a web-based survey that we’ll try to get every queer person in New York City to take. It asks questions about MPV symptoms, if you’ve been vaccinated, who you’re friends with, and who you have sex with. This will ultimately provide some information about how widespread the virus has been in our city, and who’s most likely to have had it. We also will build a map of sexual and social networks—anonymously, of course. This map can be used to target vaccinations to those at highest risk and/or where vaccine uptake is lagging behind. [People administering vaccines] can show up, for example, at a gay bar, gym, or even a coffee shop, if that place overlaps with the people you need to find.
In New York, we know that Black people are disproportionally sick with MPV compared to their access to vaccines: while Black people make up 31% of the queer community, only 12% of eligible Black queer people have received a single dose of vaccine. RESPND-MI, led by a Black epidemiologist alongside co-investigators who are mostly queer and trans people of color, is one of many essential ways to end this horrifying disparity.
Source: NYU