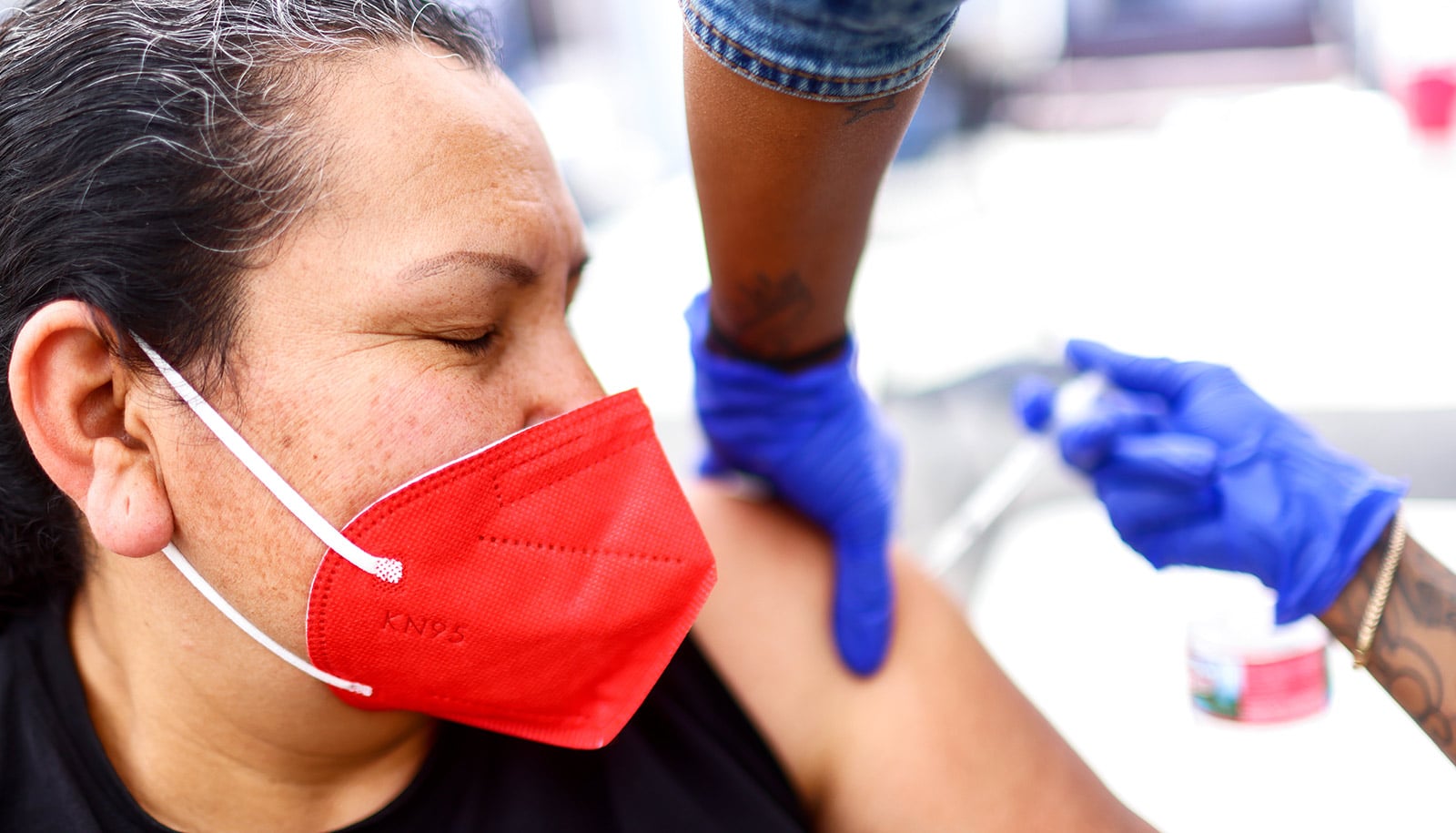
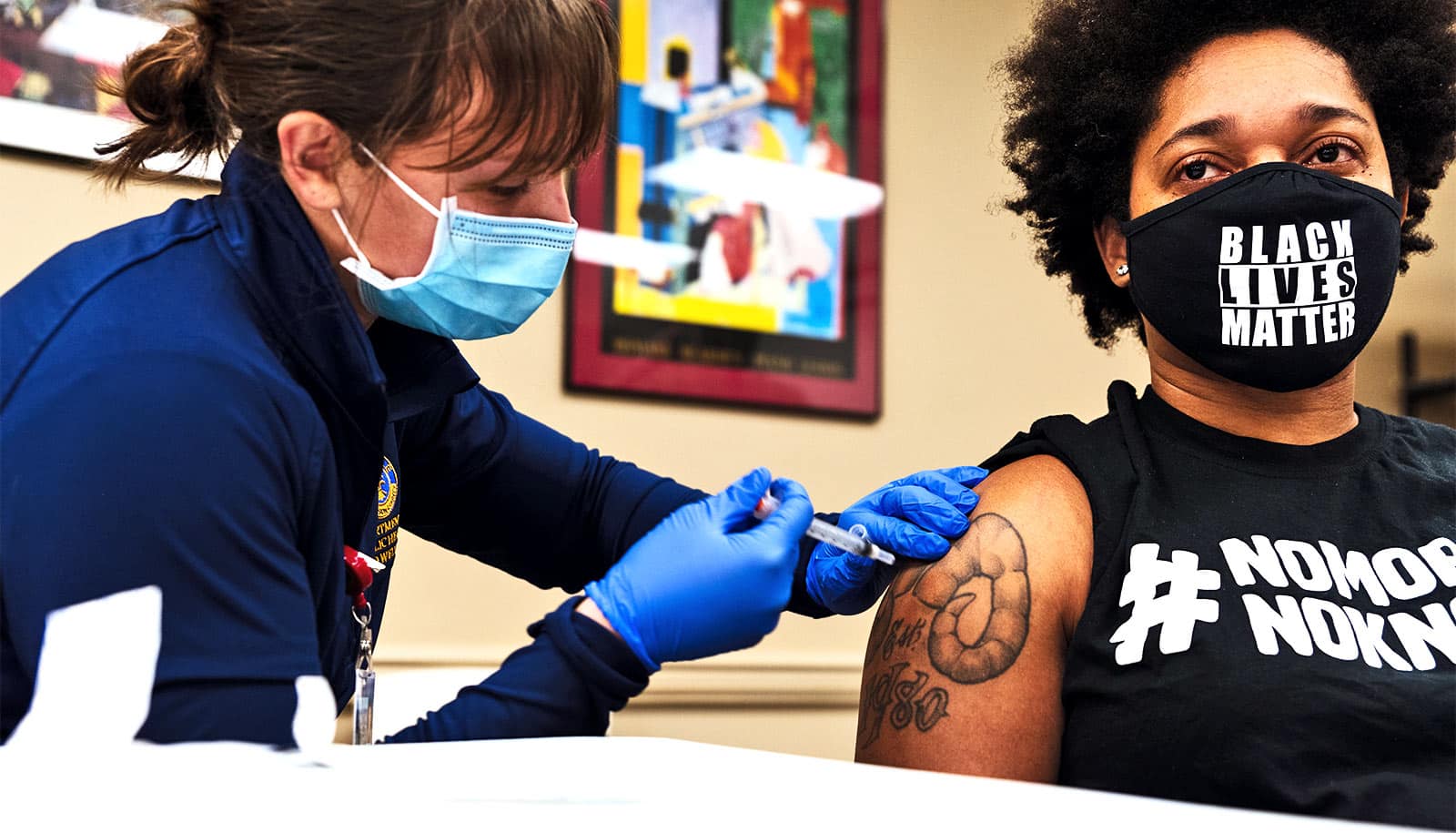
People who have recovered from COVID-19 had a robust antibody response after the first mRNA vaccine dose, but little immune benefit after the second, research finds.
The findings, published in Science Immunology, suggest only a single vaccine dose may be needed to produce a sufficient antibody response.
Researchers found that those who did not have COVID-19—called COVID naïve—did not have a full immune response until after receiving their second vaccine dose, reinforcing the importance of completing the two recommended doses for achieving strong levels of immunity.
The study provides more insight on the underlying immunobiology of mRNA vaccines, which could help shape future vaccine strategies.
“These results are encouraging for both short- and long-term vaccine efficacy, and this adds to our understanding of the mRNA vaccine immune response through the analysis of memory B cells,” says senior author E. John Wherry, chair of the department of systems pharmacology and translational therapeutics at the University of Pennsylvania and director of the Penn Institute of Immunology in the Perelman School of Medicine.
Memory B cells and COVID-19 immunity
The human immune response to vaccines and infections result in two major outcomes—the production of antibodies that provide rapid immunity and the creation of memory B cells, which assist in long-term immunity. This study represents one of the first to uncover how memory B cell responses differ after vaccination in people who previously experienced infection, compared to those who have not had COVID-19.
“Previous COVID-19 mRNA vaccine studies on vaccinated people focused on antibodies more than memory B cells. Memory B cells are a strong predictor of future antibody responses, which is why it’s vital to measure B cell responses to these vaccines,” Wherry says. “This effort to examine memory B cells is important for understanding long-term protection and the ability to respond to variants.”
The researchers recruited 44 healthy people who received either the BioNTech/Pfizer or Moderna mRNA COVID-19 vaccine at the University of Pennsylvania Health System. Of this cohort, 11 had a prior COVID-19 infection. The researchers collected blood samples for deep immune analyses four times prior to and after vaccine doses.
The data show key differences in vaccine immune responses in COVID naïve versus COVID-19 recovered people. The findings suggest that only a single vaccine dose in people recovered from COVID-19 may be enough to induce a maximal immune response, based on both strong antibody and memory B cell responses. This is likely due to a primary immune response because of their natural infection.
In contrast, it took two vaccine doses to demonstrate considerable antibody and memory B cell responses for those who did not have COVID-19, underlying the importance of the two-dose mRNA vaccine schedule to achieve optimal levels of immunity.
Protection against re-exposure to COVID-19
An analysis of antibodies against the D614G mutation and the B.1.351 South African variant of COVID-19 also reflected the findings. For those who did not have COVID-19, it took a second dose to get a robust enough immunity level against the mutation and variant, but those recovered from COVID-19 had a strong enough antibody response after one dose.
“This is important for us to keep in mind as we consider vaccination strategies in the future and potential viral variants,” Wherry says. “We need to make sure people have the strongest memory B cell responses available. If circulating antibodies wane over time, our data suggests that durable memory B cells could provide a rapid source of protection against re-exposure to COVID-19, including variants.”
Side effects “are not necessarily a bad thing—they may actually be an indicator of an even better immune response.”
The researchers also examined vaccine-induced side effects in relation to immune responses. While seen in a smaller cohort of 32 COVID naïve people, they found that those who experienced systemic side effects after receiving a vaccine dose—such as fever, chills, headache, and fatigue—had stronger post-vaccination serum antibodies, but not memory B cells.
Although more data are needed and all subjects developed robust immunity, it is possible that inflammation and side effects early after vaccination could signal stronger immune reactions.
“Everyone has good responses to the vaccines. They work to protect people against COVID-19. But for those who may be worried about side effects, they are not necessarily a bad thing—they may actually be an indicator of an even better immune response,” Wherry says.
The researchers are continuing larger-scale studies, which are necessary to fully examine the question of a one- or two-dose regimen in COVID-19-recovered people and to see how long the vaccine antibodies last. Wherry and his team are continuing to study the vaccine’s effect on virus-specific T cell responses, another element of the body’s immune response.
The National Institutes of Health, the Allen Institute for Immunology, Cancer Research Institute-Mark Foundation Fellowship, Chen Family Research Fund, the Parker Institute for Cancer Immunotherapy, the Penn Center for Research on Coronavirus and Other Emerging Pathogens, the University of Pennsylvania Perelman School of Medicine, and a philanthropic gift from Jeffrey Lurie, Joel Embiid, Josh Harris, and David Blitzer funded the work.
Source: Penn