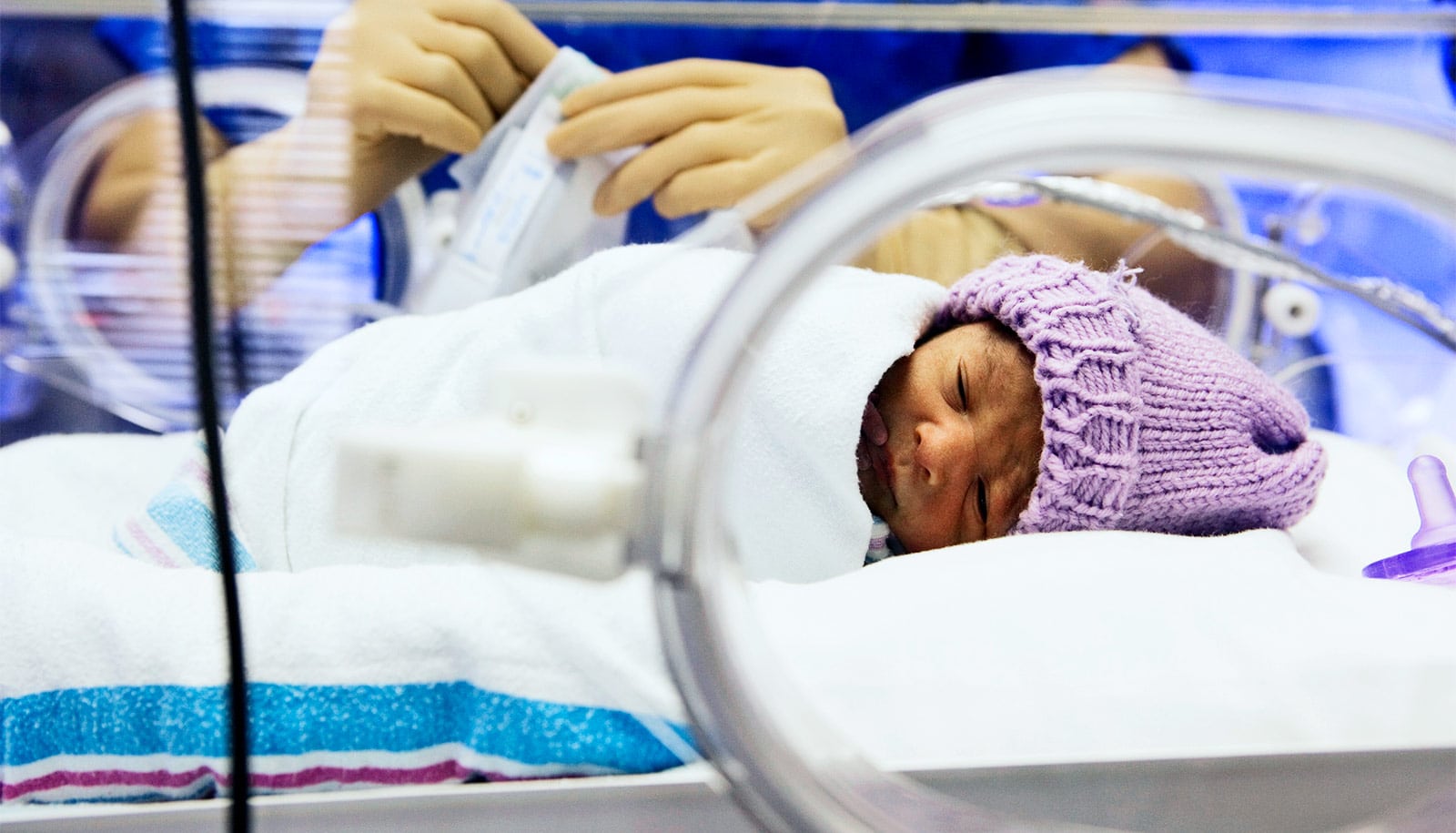
Researchers have developed a new diagnostic tool to better predict the likelihood of premature birth and neonatal morbidity in the early stages of pregnancy.
The tool may improve care and outcomes for both baby and mother.
Premature birth affects one out of 10 women in the United States and can lead to multiple complications in newborns. Until now, there were limited tools available to predict preterm birth and no tools to predict neonatal morbidity.
“Preterm delivery is an area of study that has tremendous implications for the health of the newborn. This is an exciting opportunity to empower women to understand risks to their pregnancy and be proactive about their care choices,” says Avinash Patil, clinical assistant professor in the obstetrics and gynecology department and a maternal-fetal specialist at the University of Arizona College of Medicine-Phoenix.
“When I see pregnant women, their concern is, ‘Will my child be able to come home with me or will my child need to stay in the NICU?'”
“This science will be the basis of a tool to help shape the care that women receive to improve pregnancy outcomes.”
The study, published in PLOS ONE, examined levels of progesterone metabolites in conjunction with patient demographic and obstetric history. The combination of these factors allowed researchers to predict, with a high degree of certainty, women who more likely to have a very preterm birth. Very preterm births—babies born before 32 weeks of pregnancy—often result in neonatal morbidity and mortality.
The investigation also identified which pregnancies would result in newborns with multiple complications, as premature birth is associated with substantial complications for the newborn. The study revealed a high correlation between at-risk pregnancies and newborns spending up to seven weeks longer in the neonatal intensive care unit than the low-risk group.
“This is really an attempt to better understand what might happen to the newborn. When I see pregnant women, their concern is, ‘Will my child be able to come home with me or will my child need to stay in the NICU?'” says Patil.
The study used plasma samples collected as part of the Building Blocks of Pregnancy Biobank at the Indiana University School of Medicine. For more than 11 years, the biobank has collected samples from pregnant patients in all trimesters, as well as during labor and delivery.
“These discoveries about different progesterone metabolites and their roles in prediction and potentially prevention of spontaneous preterm birth are very exciting,” says coauthor David Haas, vice chair of research for the Indiana University School of Medicine department of obstetrics and gynecology.
“While more research is needed, these findings are a significant step in helping physicians provide multidisciplinary, personalized care to improve perinatal outcomes for their patients.”
Patil, is the founder and CEO of Nixxi, a company focused on improving women’s health and pregnancy outcomes. Additional coauthors are from Valley Perinatal Services, Wake Forest University, Gaikwad Steroidomics Laboratory, and Indiana University.
Source: University of Arizona