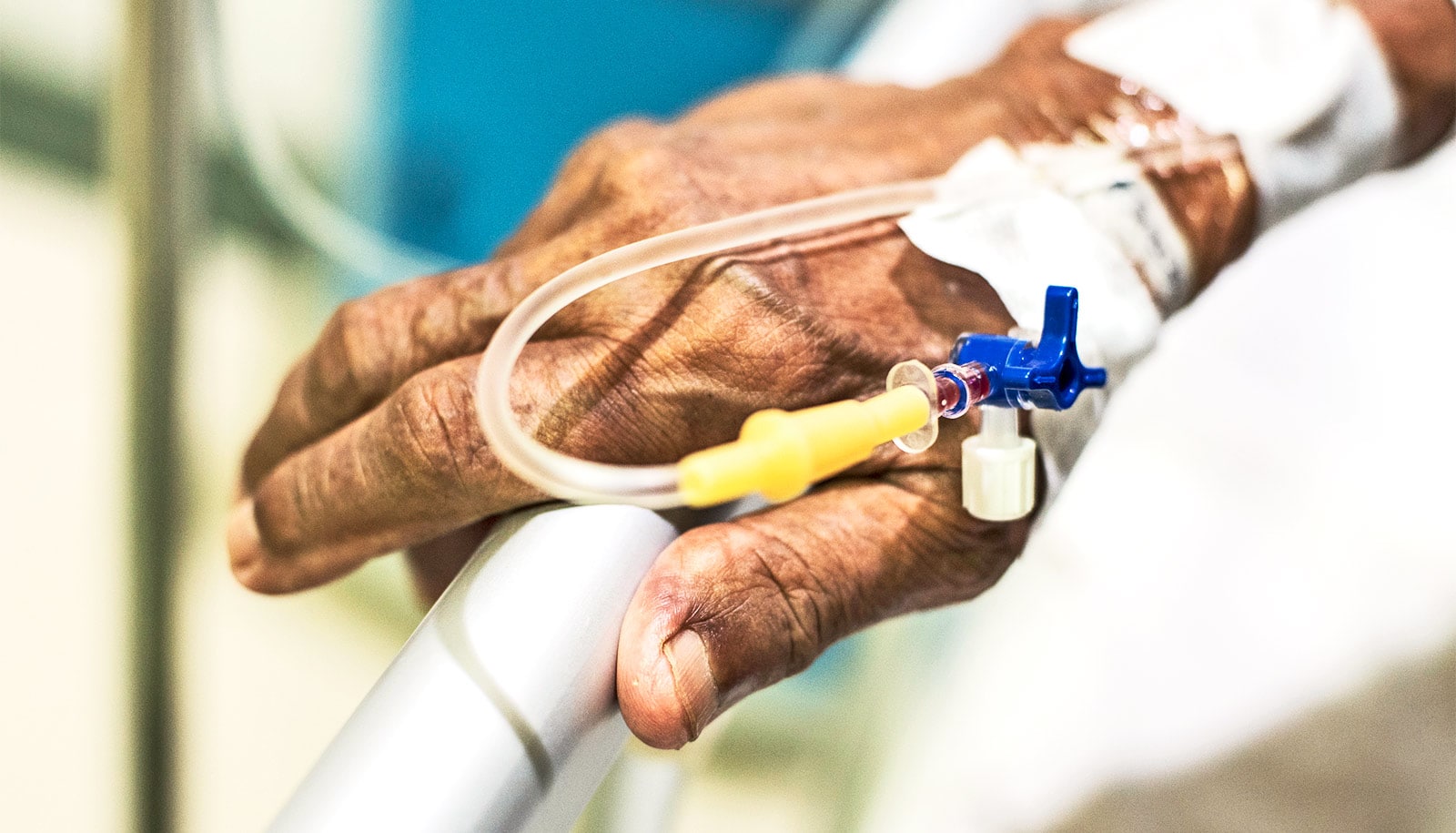
Decisions about which antibiotics to give a patient when a life-threatening infection is suspected may have unintended consequences for patient outcomes, a new study reveals.
Beginning in 2015, a 15-month national shortage of a commonly prescribed antibiotic, piperacillin/tazobactam, known by the brand name Zosyn, provided a unique opportunity to compare rates of death in hospitalized patients with sepsis who were administered two different types of antibiotics—one that spares the gut microbiome and one that profoundly alters it.
Piperacillin/tazobactam is a broad-spectrum antibiotic that is commonly administered for sepsis, a life-threatening complication from infection. In its absence, clinicians commonly instead use another antibiotic, cefepime, which has similar activity against common sepsis pathogens but, unlike piperacillin/tazobactam, has minimal effects on anaerobic gut bacteria.
“These are powerful antibiotics that are administered to patients every day in every hospital nationwide.”
“We saw this Zosyn shortage as a one-of-a-kind opportunity to ask whether this antibiotic, which we know depletes the gut of anaerobic bacteria, makes a difference in terms of patient outcomes,” says Robert Dickson of the University of Michigan medicine department’s division of pulmonary and critical care medicine. Dickson is also deputy director of the Weil Institute for Critical Care Research & Innovation.
In health, the gut microbiome is largely populated by anaerobic bacteria that rarely cause disease. Prior work by the study team has revealed that even a single dose of piperacillin/tazobactam kills most of these anaerobic gut bacteria, which play important roles in the body’s metabolism, immunity, and prevention of infections.
Dickson, Rishi Chanderraj of the division of infectious disease, Michael Sjoding of the division of pulmonary and critical care medicine, and their team at the University of Michigan and the VA Ann Arbor used patient record data to look at outcomes in 7,569 patients. The team compared 4,523 patients who were treated were piperacillin/tazobactam with 3,046 patients who received cefepime.
They found marked differences: treatment with piperacillin-tazobactam was associated with a 5% increase in 90-day mortality, more days on a ventilator, and more time with organ failure.
“These are powerful antibiotics that are administered to patients every day in every hospital nationwide,” says Chanderraj. “Clinicians use them because they are trying to treat every possible pathogen that might be causing their patients’ illness. But our results suggest that their effects on the microbiome might also have important effects on patient outcomes.”
“A 5% mortality difference has enormous implications because sepsis is so common.”
The study builds on previous work by the study team that suggested critically ill patients may do worse when given antibiotics that deplete the gut of anaerobes. They have also seen similar effects when studying animal models.
“Our prior work suggested that there might be harm with piperacillin/tazobactam, but it was an observational study that had some limitations,” says Sjoding, the study’s senior author.
“That’s why the drug shortage was such an amazing opportunity. It created an almost perfect natural experiment that let us test the difference between these two drugs on patient outcomes in a very rigorous manner.”
A recent clinical trial pitted these two antibiotics against each other and compared side effects and mortality after two weeks. That trial did not find any differences in the short term—a finding that the team also observed in their analysis.
“When we looked at two-week outcomes in our study, we didn’t find differences either,” says Chanderraj. “But the differences at three months were dramatic.”
Overall, the new findings suggest that treatment with piperacillin/tazobactam instead of cefepime may contribute to one additional death per every 20 septic patients treated.
“A 5% mortality difference has enormous implications because sepsis is so common,” says Dickson. “Every day, thousands of clinicians are deciding which of these drugs to use in septic patients.”
Physicians should give more thought about whether anti-anerobic antibiotics are warranted before prescribing them, adds Chanderraj.
“We need to think about antibiotics like chemotherapy. In the right context, treatment can be lifesaving, but in the wrong context, it can be quite harmful.”
The research appears in JAMA Internal Medicine.
Source: University of Michigan