Parasitic infections were likely widespread in New England, even in remote areas and in wealthy households, report archaeologists who analyzed excavated fecal samples.
Parasitic infections, including tapeworm and whipworm, were a common problem in the United States until the 20th century. The common belief is that these infections mainly affected lower-income, urban areas where conditions—including shared public spaces, lack of sewage systems, and poor sanitation—were prime for disease spread.
However, the new research, published in the Journal of Archaeological Science: Reports, suggests otherwise.
“Unlike today, when high-income households are less likely to exhibit signs of infection, wealth and status did not apparently provide insulation from infection exposure in this rural setting, despite likely having greater access to medicines and improved sanitation,” says Theresa Gildner, assistant professor of biological archaeology at Washington University in St. Louis.

Gildner and Jesse Casana of Dartmouth College found conclusive evidence for parasitic infection from samples recovered from a privy (outhouse) that was attached to a wealthy household on the Dartmouth campus in New Hampshire. The samples are believed to be from the 1830s and ’40s.
Archaeologists analyze excavated fecal samples to learn about historic parasite infection patterns, as well as the diet and health of past human populations. The earliest indication of parasite infection in human ancestors dates back 500 million years ago.
Using latrine samples from urban archaeological sites, researchers have previously suggested that parasitic infection disproportionately affected lower-income households.
“Our results suggest that parasitic infection in this region may have been more widespread than previously recognized. These findings help inform our understanding of the lives of rural 19th-century New England communities,” Gildner says.
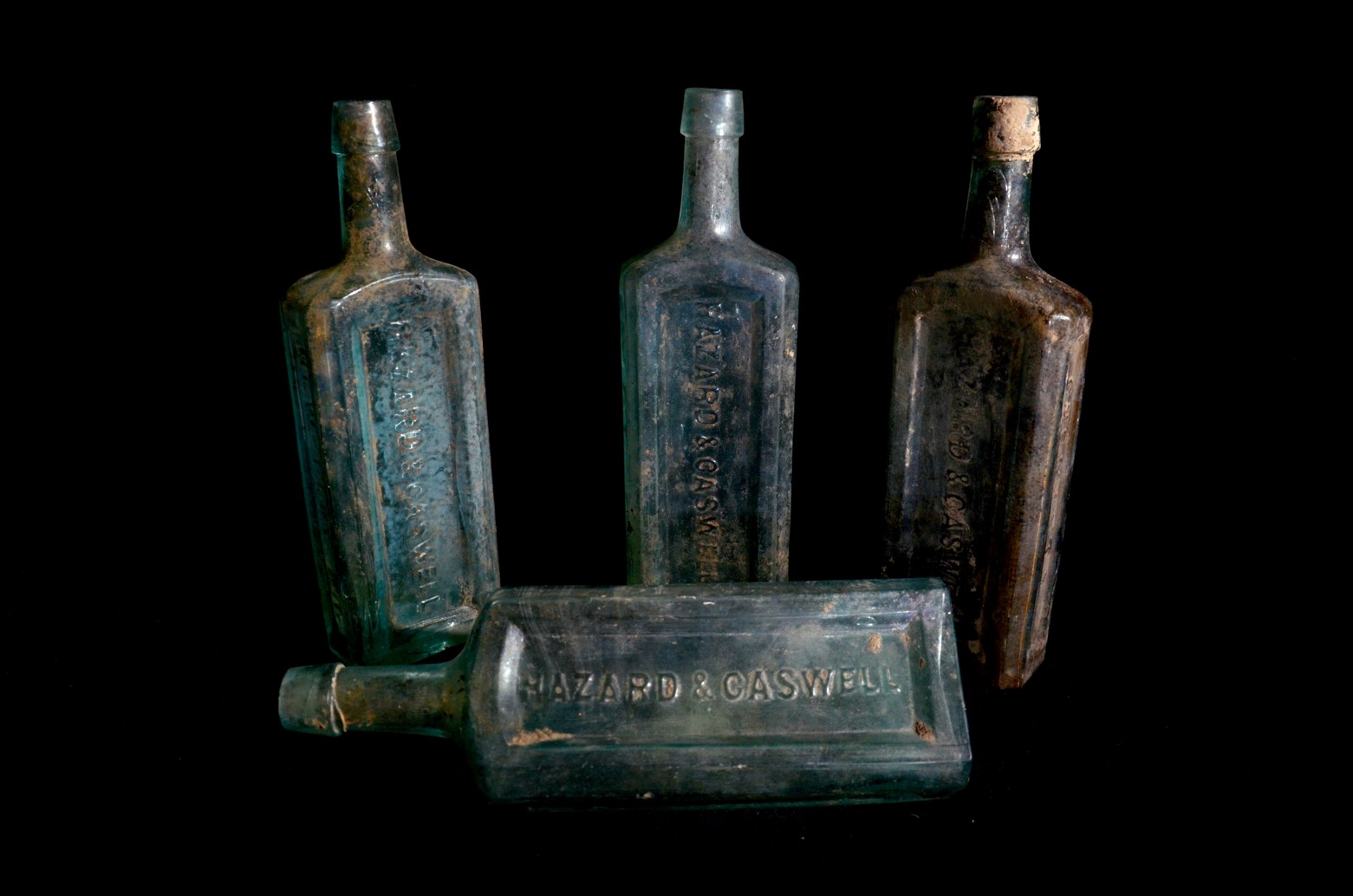
‘Not just a fluke’
In the late 18th and early 19th centuries, large, stately homes went up around the Dartmouth campus for wealthy families connected to the college. One of these grand houses was the home of Mills Olcott, a Dartmouth graduate who went on to become a wealthy businessman and politician. He lived in the home with his wife, Sarah Olcott, and their nine children from 1801-1850. They were one of the wealthiest families in the community.
In 1910, Dartmouth purchased the house and moved it several blocks north on Main Street to make way for the construction of Baker Library, leaving the underground privy intact. Today, the house is known as the Choate House, named for Dartmouth alumnus Rufus Choate.
In anticipation of a major infrastructure project that could threaten much of the archaeological remains on central campus, an excavation of the privy and surrounding areas began in June 2019.
In one level of the privy, likely dating to the 1830s and ’40s, organic preservation was exceptionally good with intact shoes, cloth, wood, and botanical remains, the researchers say. From this level, they recovered several intact fecal samples, which—based on their context—likely derive from the period when the house was occupied by the Olcott family.
All three samples showed signs of parasitic infection, specifically, both tapeworm and whipworm eggs. Researchers also recovered an abundance of medicine bottles, including medicines marketed to cure digestive ailments, from the same privy levels in which the fecal samples were collected.
“While these results do not definitively demonstrate that parasitic disease was widespread across New England at this time, they do provide novel evidence that infection was possible in these areas, including within wealthy rural communities, which we might expect to be protected from the spread of these infections due to low population density and access to resources like healthy food,” Gildner says.
“Additionally, the two types of parasite observed—whipworm and tapeworm—were consistently evident in all three samples, suggesting it’s not just a fluke.”
Given that most parasite infection today is found in warm, tropical regions, it is somewhat surprising that parasitic eggs are evident in all three samples analyzed, the researchers say. The cold New England winters are not hospitable to parasite eggs passed into the environment. However, mature worms could survive in their human hosts during the winter months and transmit infective eggs during warmer months leading to reinfection of household members—which is what likely happened to the Olcott family.
Parasites are still a concern
Today, parasitic infections remain a global health concern—especially in low-income communities in tropical regions. Millions of people are currently infected worldwide, Gildner says.
“These infections are not restricted to populations living in the 1800s. They continue to be a very real global health crisis today.”
“I view these findings as a reminder to be grateful for all the amenities we have today that help prevent parasite infection and which we often take for granted.”
While relatively few people die from these illnesses, chronic infections with many worms often cause a range of symptoms, such as abdominal pain, weight loss, rectal prolapse, nausea, and impaired physical and cognitive function.
“These results highlight how different our health concerns in the US are today than in the past,” Gildner says. “With excellent sanitation and sewage systems, filtered water, uncontaminated food items from the grocery store, and houses built to shield us from sources of infection, most Americans have probably never worried about contracting a parasite infection.
“So, I view these findings as a reminder to be grateful for all the amenities we have today that help prevent parasite infection and which we often take for granted.”
The results are also a call to action, Gildner says.
“We have the tools to successfully control the spread of parasitic infection, as many communities in the US have successfully done. But millions of people around the world still experience parasitic infection, and emerging evidence suggests that parasites may continue to infect Americans living in areas with limited medical and sanitation infrastructure,” she says.
“There is still a lot of work to be done. These infections are not restricted to populations living in the 1800s. They continue to be a very real global health crisis today.”



