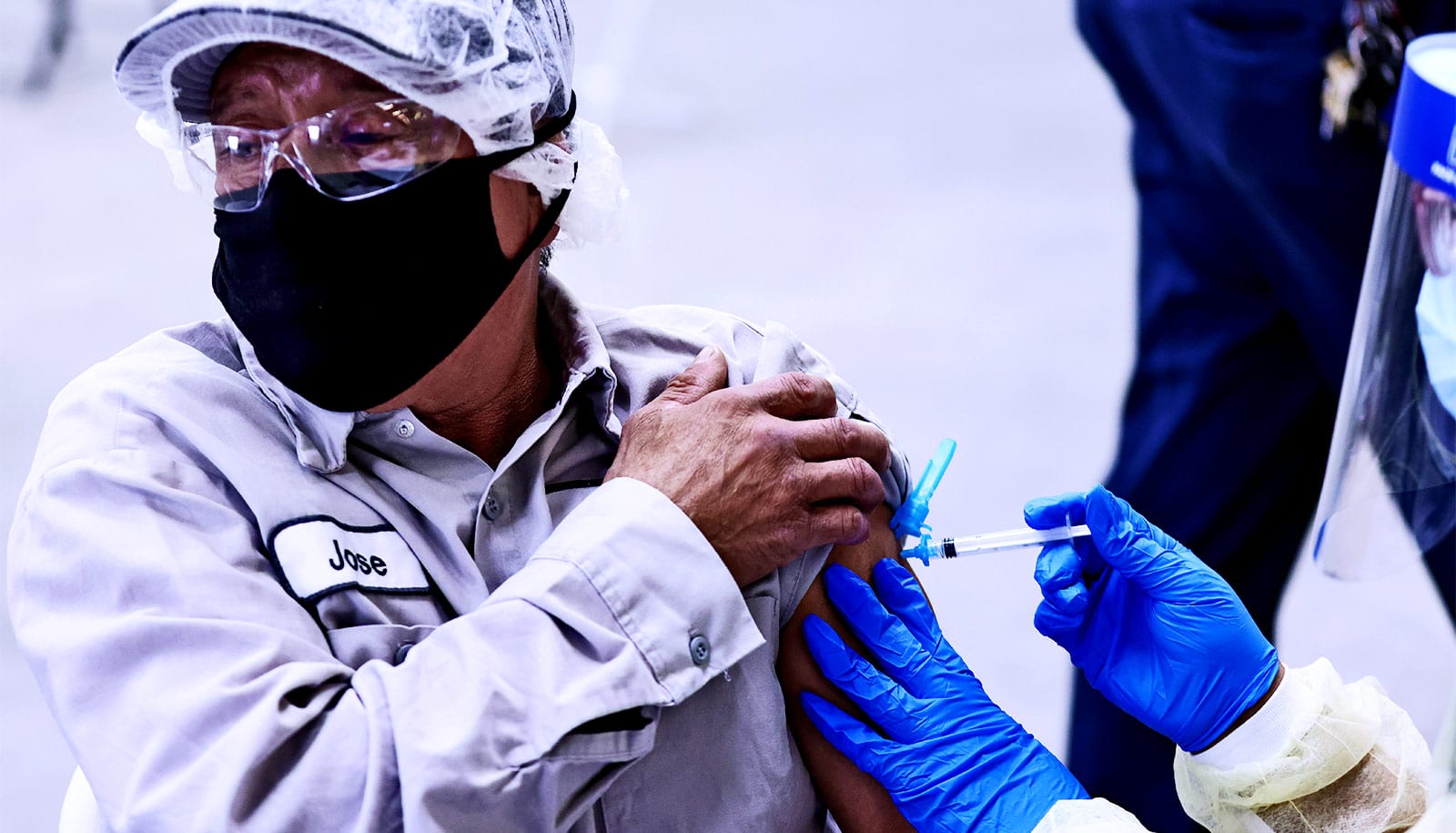
The pause in the rollout of the Johnson & Johnson vaccine is the right course, but the vaccine’s benefits “without doubt outweigh the risks,” a vaccine researcher argues.
On Tuesday, the US Centers for Disease Control and Prevention (CDC) recommended that states pause their rollout of the Johnson & Johnson one-shot COVID-19 vaccine, citing six people who suffered rare cases of blood clotting in a vein carrying blood away from the brain. The six cases occurred in American women between the ages of 18 and 48, and one of the women died.
The news comes as Johnson & Johnson was also dealing with a processing plant that botched 15 million doses before distribution. Tuesday’s Johnson & Johnson pause, which could last days or a week, is also an obstacle to President Biden’s administration as it tries to assure vaccine-hesitant Americans that the coronavirus vaccines are safe.
On Tuesday, Anthony Fauci, the nation’s leading infectious disease expert, said at a White House press briefing: “This is a really rare event. If you look at what we know so far, there have been six out of the 6.85 million doses, which is less than one in a million.”
Florian Douam is a virologist and vaccine expert at Boston University’s National Emerging Infectious Diseases Laboratories (NEIDL) who’s developing humanized mouse models that can help lead to better vaccines against COVID-19 in humans.
Here, Douam, who is also a Boston University School of Medicine assistant professor of microbiology, explains his take on how the J&J news will affect national and global COVID vaccination efforts as well as vaccine hesitancy among the public:
Were you surprised by the news today?
Partially. You’ve probably heard about what is going on with the AstraZeneca vaccine in Europe—the European Medicines Agency has established a link between the AstraZeneca vaccine and some thrombosis cases. Both the AstraZeneca and Johnson & Johnson vaccines are derived from an adenovirus. So when I heard the news, my first thought was, this might be bad news in general for adenovirus-based vaccines.
Can you explain what you mean by that?
It’s the first time we’ve vaccinated so many people with an adenovirus-based vaccine. [These vaccines use a protein shell, derived from a virus and encased around the genetic material from the coronavirus, delivering the coronavirus genetic code into the body which triggers an immune response to build antibodies against the coronavirus.] What we’re uncovering is a very small risk that the vaccine may cause clotting in some individuals. With the J&J vaccine we’re talking about six cases among seven million people vaccinated. These events are providing us with a better overview of the risks and benefits associated with the J&J vaccine; it’s very informative from a vaccine development perspective.
That being said—the benefits still far outweigh the risks. I understand the cause for concern, for the need to step back and see what’s going on, but I don’t think these six cases should be a cause for people to fear the J&J vaccine.
For comparison, if you consider the yellow fever vaccine—more than 500 million people have been vaccinated. Even though it’s one of the most efficient vaccines ever created, there’s a slight risk. About .4 to .8% of every 100,000 vaccines will cause severe illness (that’s about .0004% of people vaccinated). But yellow fever has a 25 to 50% mortality rate. So the vaccine benefit outweighs the risk. In the case of a massive-scale pandemic like coronavirus, the benefits without doubt also outweigh the risks. What we’re witnessing here is .00008% of people might develop a severe reaction—much, much less than the chances of getting COVID-19.
So this pause announced today should not be a cause for widespread fear. As we try to shut down a global pandemic, the benefit of the J&J vaccine, which only requires one dose, is huge.
So, with such a small number of people being affected by clotting, why the big pause in rolling out the J&J vaccine?
Given that only six people out of seven million have had reactions, pausing vaccination is a bit of a surprising move. But I think it’s the best decision to try and not lose public trust, to show the population that [public health] authorities are taking this handful of reactions very seriously. I think that’s the right move. If, instead, they did not pause vaccination but just moved forward, pretending that nothing had happened, it would undermine public trust.
This is almost like a political move [on the part of public health authorities] to keep people’s trust, because the most important factor in successfully rolling out COVID-19 vaccines is to keep that trust. That being said, the news media have a critical role to play—making the public understand that reviewing the safety profile of a vaccine is very different from saying that a vaccine is dangerous. That distinction is key.
I assume [the public health authorities] are now going to look at the medical history of these individuals; I have low expectations that they will find out exactly what happened with these individuals. But if they can identify a specific clinical condition in these patients that contributed to these adverse reactions, especially in the person that died, I think that will help the J&J vaccine rollout and [the US in keeping up with its goal pace of vaccinations].
I have many family members and friends in France, where Europeans are grappling with the same concerns about AstraZeneca. I’ve received a lot of calls from family and friends, telling me that they’ve been offered AstraZeneca but are afraid to take it because of the thrombosis cases—even though I’ve told them they ought to take the first vaccine that becomes available to them. They say they would rather wait to get the Moderna or Pfizer-BioNTech vaccines. This suggests to me that even though the benefits of adenovirus-based vaccines [like the ones manufactured by J&J and AstraZeneca] clearly outweigh their risks, the public is starting to associate mRNA vaccines with being a potentially safer option. This is good news for mRNA vaccine manufacturers [like Moderna and Pfizer-BioNTech] and for the future of mRNA vaccine technology in general.
Can you remind us what’s different about the mRNA vaccines versus adenovirus vaccines, and how that might impact reactions to vaccination?
The advantage of mRNA vaccines is that they are [easily and quickly] produced in large scale. After synthesizing mRNA (in the case of COVID-19 vaccines, “messenger” RNA is genetic material that instructs the body to build antibodies against SARS-CoV-2), you just need to encapsulate that mRNA inside a lipid shell (a lipid is a naturally occurring fatty acid) to create a vaccine. In contrast, making a viral vector—like adenovirus—is a bit more complicated [and time-consuming]. So the biggest advantage is that mRNA vaccines can be developed faster in response to emerging infectious diseases.
The lipid shell surrounding the mRNA is also [not very] immunogenic—meaning it doesn’t trigger an immune reaction from the human body. The adenovirus shell does trigger an immune response, so the body is recognizing and mounting an immune response both to the adenovirus shell and to the SARS-CoV-2 genetic material inside it. This heightened immune response could trigger some adverse effects, so there is a slightly higher risk of a more adverse reaction when using an adenovirus shell.
What do you hope the outcome will be when it comes to the J&J vaccine?
We’ll see what information the investigation yields. But I have absolutely no concerns about the safety profile of the J&J vaccine. I am concerned, however, about the public losing trust in this critical [public health] tool that could bend the trend of this pandemic [in the right direction]. It needs to be explained that getting this vaccine still remains a huge benefit, because [vaccination is] the only path toward [us all having] a more normal life again. Even if a clear connection isn’t found to explain why these six individuals developed blood clotting, there should be a clear explanation to the public that the benefits [of the J&J vaccine] still outweigh the risks. The extremely low frequency of adverse reactions suggests that they are really, really rare and should not be cause for concern.
To my knowledge, a situation like this has never happened before, where a vaccine rollout of this scale has been paused for so few adverse reactions [.0008% of people vaccinated]. But it’s also the first time we’re doing such a massive global vaccination effort in such short timing. Everything is historic at the moment. I am hopeful that in a few days’ time, the J&J rollout will be back on track. I think this pause is being done to preserve public trust and conduct a thorough review of what has happened with these six cases. However, how the conclusions of this review will be [described and communicated] is going to be very important to preserve public trust in [COVID-19] vaccines.
If we lose public trust toward the J&J vaccine—like what is happening in Europe with the AstraZeneca vaccine—the rollout of the mRNA vaccines will have to be intensified, which will be a complicated process. This will create a slowdown of the vaccine rollout overall, which would mean more COVID-19 cases and deaths. It’s obviously still too early to say if what happened Tuesday will have a [long-term] impact on the rollout, but I really hope it does not. The news media has a big role to play here; [they need to continuously explain] that these adverse reactions represent a very small percentage of [all vaccinations], and that the benefits of the J&J vaccine outweigh the risks. If we do start seeing more and more people refuse to get the J&J vaccine over the next few weeks, it may be that the mRNA vaccines will become even more useful than we ever thought they would be.
Source: Boston University