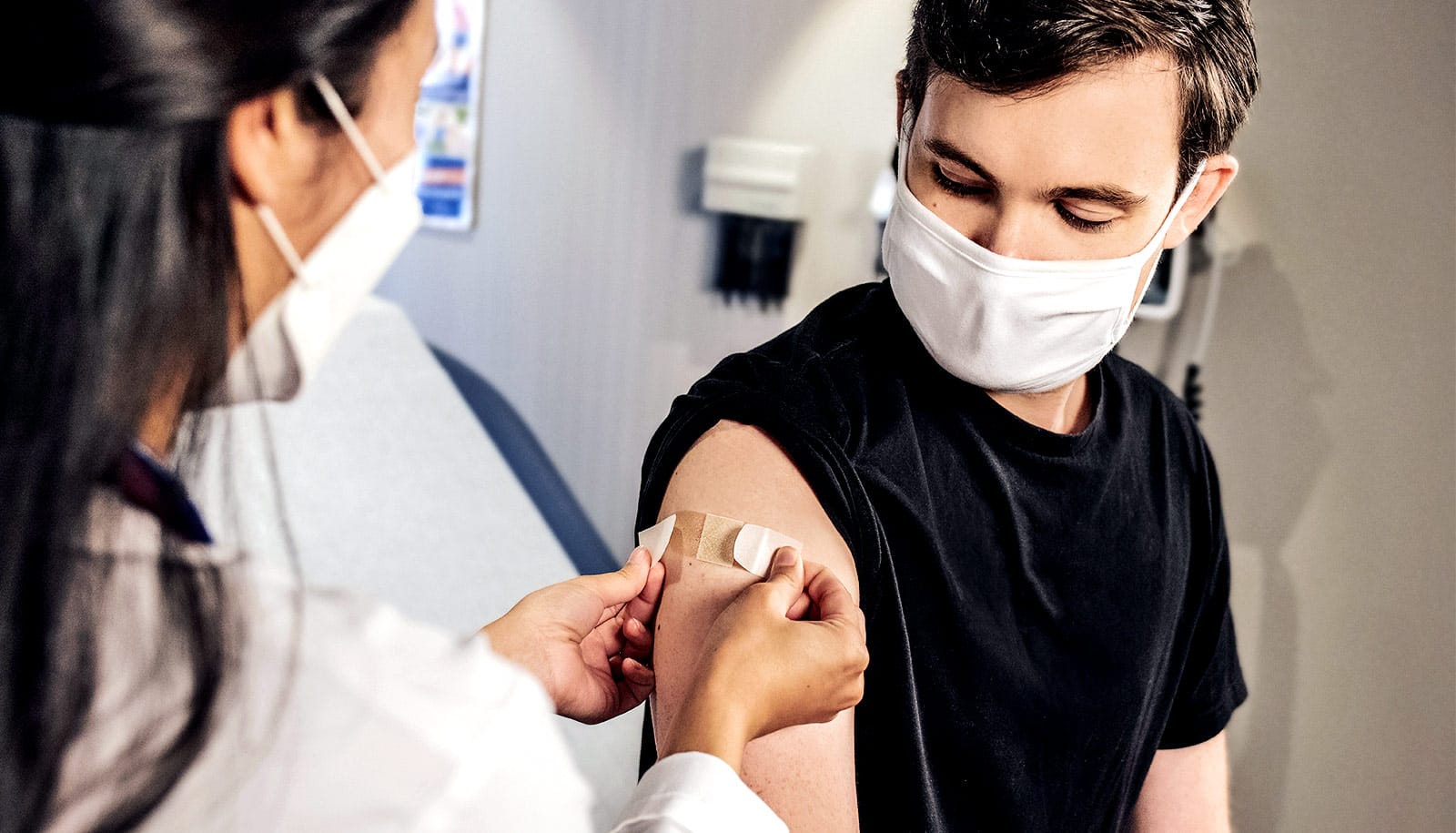
Vaccinations against human papillomavirus (HPV), a major cause of throat and back of mouth cancers, are expected to yield significant reductions in the rates of these cancers in the US, but not until after 2045.
HPV is the most common sexually transmitted infectious virus worldwide. HPV infections are often silent, and while most infections clear, some are chronic and can trigger cancers including mouth and throat (oropharyngeal), and cervical cancer because they disrupt DNA and inhibit tumor-suppressor proteins in the cells they infect.
Although there is no cure for existing HPV infections, new infections are preventable with vaccines, the first of which entered use in the US in 2006.
For the study in JAMA Oncology, researchers analyzed national databases on oropharyngeal cancer cases and HPV vaccinations, and projected the impact of HPV vaccination on the rates of these cancers in different age groups.
They estimated that the oropharyngeal cancer rate would nearly halve between 2018 and 2045 among people ages 36–45. However, they also projected that the rate in the overall population would stay about the same from 2018-2045, due to still-rising rates of these cancers in older people, where most of these cancers occur.
“We estimate that most of the oropharyngeal cancers from 2018 to 2045 will occur among people who are 55 years and older and have not been vaccinated,” says study lead author Yuehan Zhang, a PhD candidate in the research group of Gypsyamber D’Souza, professor in the epidemiology department at the Bloomberg School at Johns Hopkins University.
“HPV vaccination is going to work to prevent oropharyngeal cancers, but it will take time to see that impact, because these cancers mostly occur in middle age.”
Oropharyngeal cancer is the most common HPV-related cancer, and according to the Oral Cancer Foundation there are more than 50,000 new cases of it in the US each year. Alcohol and tobacco use also are risk factors, but are seen as increasingly less important than HPV.
Vaccination is a powerful medical weapon against this family of viruses, but has one major shortcoming: It can prevent, but not treat. In other words, it does not work against established HPV infections or against cells that have been transformed by HPV and are on their way to forming tumors.
Thus it is recommended chiefly for the young who are not yet exposed to sexually transmitted HPV. (Most people who were already adults when HPV vaccination became available have never been vaccinated, and thus remain at risk for these cancers.)
For the study, the researchers estimated current and future HPV vaccination rates using data from surveys conducted by the US Centers for Disease Control and Prevention, and projected oropharyngeal cancer rates based on past and current incidence data from the National Cancer Institute.
They estimated that the rates of vaccination by 2045, for different age groups—given the emphasis on vaccinating the young—will amount to about 72% of people ages 36–45, 37% of those ages 46–55, 9% of those ages 56–69, and 0% of people ages 70–83 being vaccinated.
These projections show continuing high oropharyngeal cancer rates in older, mostly unvaccinated groups, and almost no change in the overall US rate of these cancers—14.3 per 100,000 assuming no vaccination; and 13.8 per 100,000, with vaccination, in 2045.
However, they foresaw the rates of new oropharyngeal cancers would fall substantially in the relatively well vaccinated 36–45 and 46–55 age groups during the 2018-2045 period: from 1.4 to 0.8 per 100,000; and from 8.7 to 7.2 per 100,000, respectively.
The results suggest, though, that by 2045 HPV vaccination will have begun to make a significant impact.
The National Institute of Dental and Craniofacial Research funded the work.
Source: Johns Hopkins University