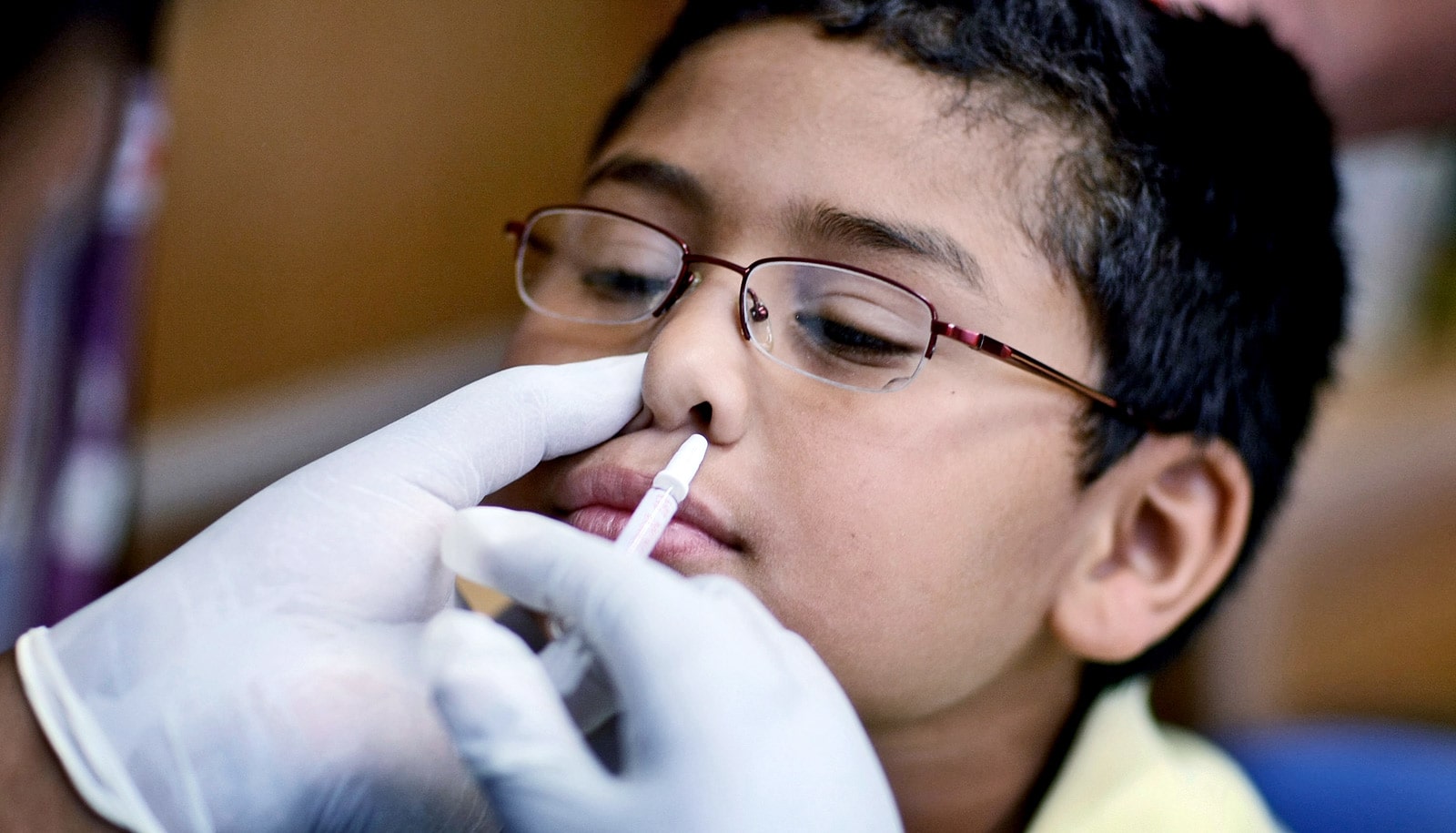
Exploiting a previously unnoticed genetic mutation may restore the effectiveness of the popular nasal spray version of the flu vaccine.
That would be a boon to the millions of people who want protection from influenza’s fever, chills, and sore throats without a shot.
This is the second straight flu season that a federal government panel recommended against using the spray vaccine, known as FluMist, in the United States. The Centers for Disease Control and Prevention advisory panel reports that the vaccine had grown less effective in recent years.
Researchers discovered an overlooked mutation in two of the viral strains used in the vaccine. When they reversed the mutation in one virus, it became more active, making copies of itself more quickly in cultured human nasal cells. That stimulated production of more of the proteins that protect against flu infection.
“It’s not clear exactly why [FluMist] has failed,” says Andrew S. Pekosz, professor of molecular microbiology and immunology at the Johns Hopkins Bloomberg School of Public Health. It is clear, however, that only one component of the vaccine—the one targeting the Type A H1N1 virus—has been a problem.
“But this mutation we identified could be used to make that component of the vaccine a little stronger, thereby improving vaccine efficacy,” Pekosz says. “We now see the possibility of altering this mutation and perhaps others in the vaccine to optimize the vaccine’s protective effect, perhaps for different age groups.”
The findings appear in Vaccine.
Weakened strains
When it first recommended against using FluMist last year, the CDC said that the manufacturer had projected making as many as 14 million doses for the 2016-2017 flu season, about 8 percent of the total flu vaccine doses projected for the year.
FluMist was licensed in 2003 and originally was considered comparable to or better than injectable flu vaccine in protecting against the flu virus. It is the only non-injection flu vaccine on the market.
Three types of influenza viruses affect people, Type A, Type B, and Type C. Flu vaccines include a mix of virus strains tailored to anticipate the upcoming flu season. The CDC estimates that over the past seven years, flu viruses have caused 9.2 million to 60.8 million illnesses, 140,000 to 710,000 hospitalizations, and 12,000 to 56,000 deaths annually in the United States. Across the globe, there are an estimated 3 million to 5 million severe flu cases each year and about 250,000 to 500,000 deaths.
The FluMist vaccine, also known as LAIV (live, attenuated influenza vaccine) is made from four weakened flu virus strains, two each representing Type A and Type B. Two segments of the strains used in the vaccine change periodically to match influenza circulating in the population.
The non-varying parts of the vaccine are made from a special cold-adapted H2N2 strain that is known to contain mutations that slow its replication at the temperatures found in the human nose and throat. That slowing of activity is largely what keeps these vaccine strains from causing illness in people, although they remain active enough to induce at least partial immune protection against influenza A.
Previous studies have linked the slower replication of this cold-adapted strain to changes in three virus genes. However, there have been hints in recent years, from Pekosz’s work and that of others, that another gene encoding a viral protein called M2 may also contribute to this effect.
“We had studied M2 for years, but one day recently a student in my lab noticed that the M2 in the LAIV influenza A viruses contains a mutation in the same part of the protein that we had previously identified as affecting viral replication,” Pekosz says.
Immune response
When the researchers introduced the mutation into a strain of influenza A virus that normally doesn’t have it, the replication rate of the virus dropped. Alternate mutations at the same site on the M2 gene also resulted in a slowing of viral replication.
The team then did the opposite experiment, starting with a FluMist influenza A strain and reversing the M2 mutation. They found that this enhanced the replication rate of the strain in human nasal cells.
Rare flu mutation might lead to new vaccine
The enhanced activity of the virus also led to a jump in production, in infected cells, of the immune protein interferon lambda, indicating an increased immune response. The result showed in principle that this mutation site, and perhaps others on the virus, may be used as “dimmer switches” to adjust the vaccine’s strength up or down—so that it induces an immune response without also causing illness.
“What we’re trying to do now is make a panel of these LAIV viruses with different mutations to see if we can boost the replication rates to get vaccine formulations that protect children and other age groups better than LAIV has done in the past few years,” Pekosz says.
Source: Johns Hopkins University