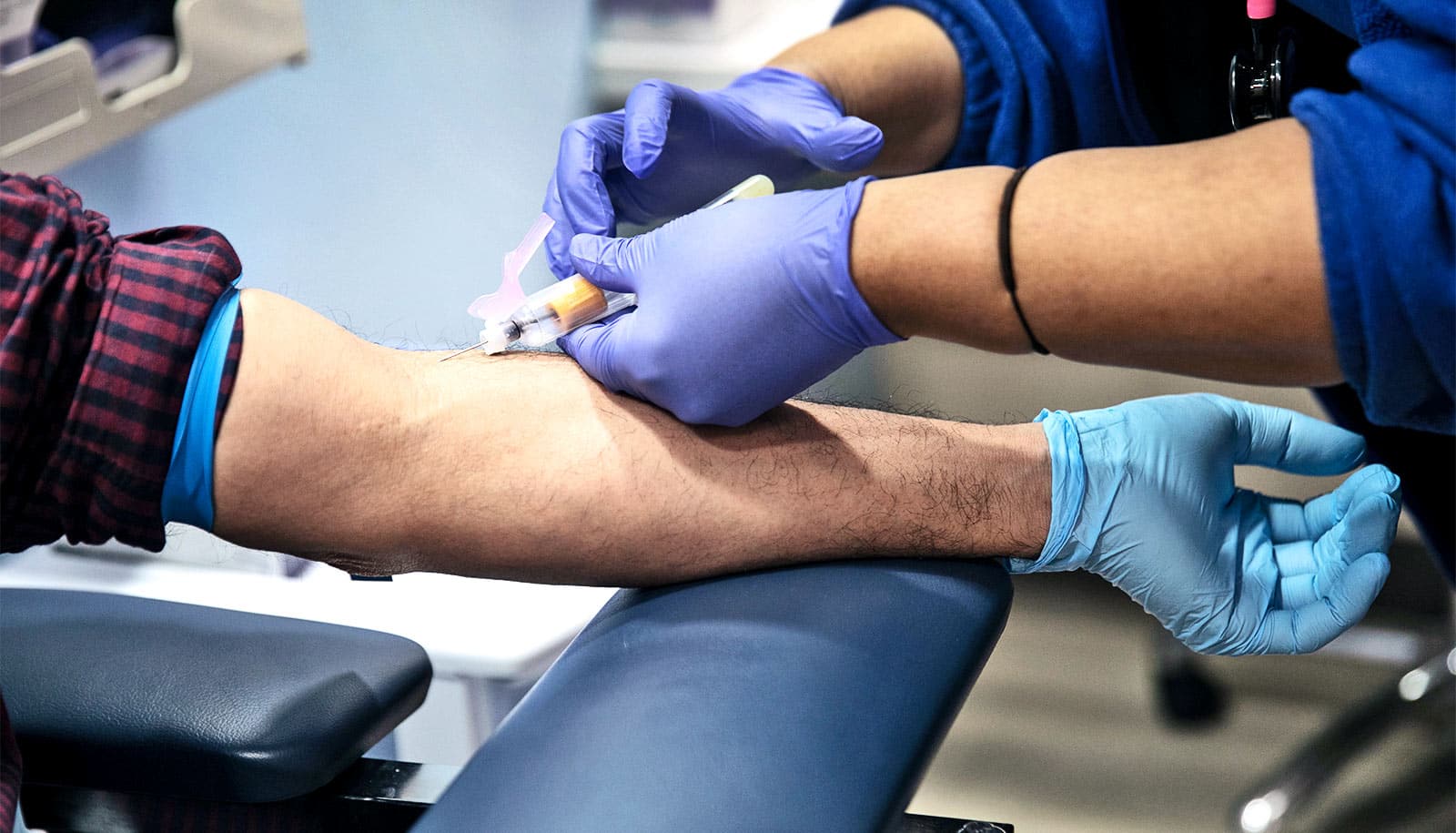
A new paper outlines a set of guidelines to guide researchers on an ethical approach to deliberately infecting volunteers who have been given a vaccine candidate with COVID-19.
This may significantly speed up the process of vaccine development and potentially save many lives, according to the paper.
“…it is incorrect to rule out human challenge experiments as unethical in relation to COVID-19 vaccine development.”
“Currently there are several vaccine candidates that are undergoing human safety testing, but to find out whether they work we need to discover what happens when a vaccinated person is exposed to COVID-19,” says Adair Richards, an honorary associate professor in the chemistry department at the University of Warwick who carries out research ethics training for postgraduate researchers in science and medicine.
“With new infections dropping in the countries where research is taking place, it may be a long time before many of the volunteers in these experiments naturally come into contact with the disease,” he says.
“Deliberately infecting volunteers with a disease as dangerous as COVID-19 has previously been considered to be unethical by the research community. However I believe that the current global situation is so different to those previously faced, that it is ethical in this case,” Adair says.
“In other areas of life it is not unusual for society to allow individuals to do things that put them at personal risk, such as to be a fire fighter or a health professional treating COVID-19 patients. Speeding up vaccine development even by a few weeks or months could result in saving many lives.”
The research analyses each of the common arguments against these types of experiments: the risk of harm to volunteers, the risk of no useable vaccine, the validity of a volunteer’s informed consent, the reputational risk to research, and that this could be a slippery slope to increasingly unethical research.
Richards demonstrates that these arguments can be overcome and in fact we do not need to lower our ethical standards to permit these types of experiment, and that it is possible to put sufficient ethical safeguards in place.
The article provides guidance for regulators and researchers and poses three key questions for those planning vaccine development studies:
- Has reasonable care been taken to maximize the potential benefits of the proposed study and minimize the risks of harm to participants?
- Is the informed consent process sufficiently robust?
- What do we need to do now to amend our processes to speed up the consideration and approval processes for proposed COVID-19 vaccine candidate phase II and phase III trials?
“My research shows that it is incorrect to rule out human challenge experiments as unethical in relation to COVID-19 vaccine development. I argue that you can apply the same standards of ethics, but that they lead us now to a different conclusion because the facts are different,” Richards says.
“Very large numbers of people globally are affected both directly and indirectly from COVID-19, and the saving of a few weeks or months of time in vaccine development can be expected to result in saving a large number of lives. There are also good ways to minimize the risk of harm to volunteers, and it is ethical, and I argue, admirable to allow a volunteer to choose to take a personal health risk to help serve a greater benefit to humanity.”
The work appears in the Journal of Medical Ethics.
Source: University the Warwick