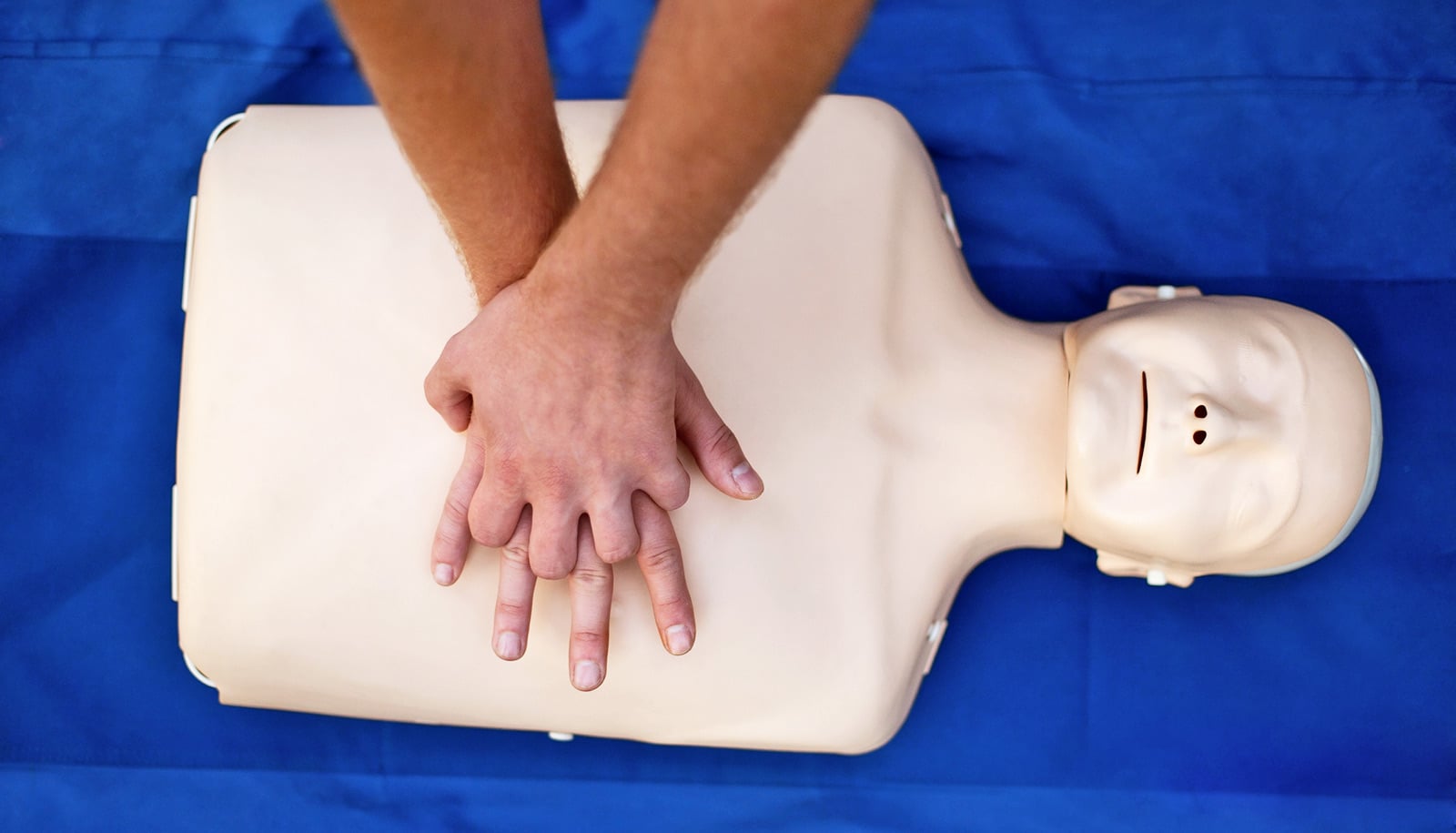
People in predominantly Hispanic neighborhoods are less likely to receive CPR from a bystander, a new study shows.
The findings confirm that the ethnic makeup of the neighborhood where a person experiences sudden cardiac arrest has a lot to do with whether they will survive the event, researchers say.
“Identifying these disparities highlights an important public health problem and leads us to think about ways to reach these communities, perhaps by tailoring CPR training to them,” says Audrey Blewer, an assistant professor in the Duke University School of Medicine, who began the study as the assistant director for educational programs at the Center for Resuscitation Science at Penn Medicine.
“It’s important to think about whether we’re doing what we need to do to help promote bystander recognition of sudden cardiac arrest and CPR in these communities.”
A previous 2017 study, found that the rate of people receiving bystander CPR was also lower in African-American neighborhoods.
The current study analyzed sudden cardiac arrest survival data from the Resuscitation Outcomes Consortium which recorded 27,482 arrest events from 2011-2015.
Blewer and colleagues compared outcomes in four different types of neighborhoods: less than 25% Hispanic; 25 to 50% Hispanic; 50 to 75% Hispanic; and more than 75% Hispanic.
While Hispanics are the fastest growing minority population in the US, few studies have assessed whether the proportion of Hispanics in a neighborhood associates with bystander CPR delivery and survival from out-of-hospital cardiac arrest.
The team found that among neighborhoods with less than 25% Hispanic residents, CPR was administered in 39% of sudden cardiac arrest events, but it was only administered in 27% of events in neighborhoods with more than 75% Hispanic residents.
The findings appear in Circulation. Additional coauthors are from Duke and from the Resuscitation Outcomes Consortium. The American Heart Association and the National Institutes of Health funded the work.
Source: Duke University