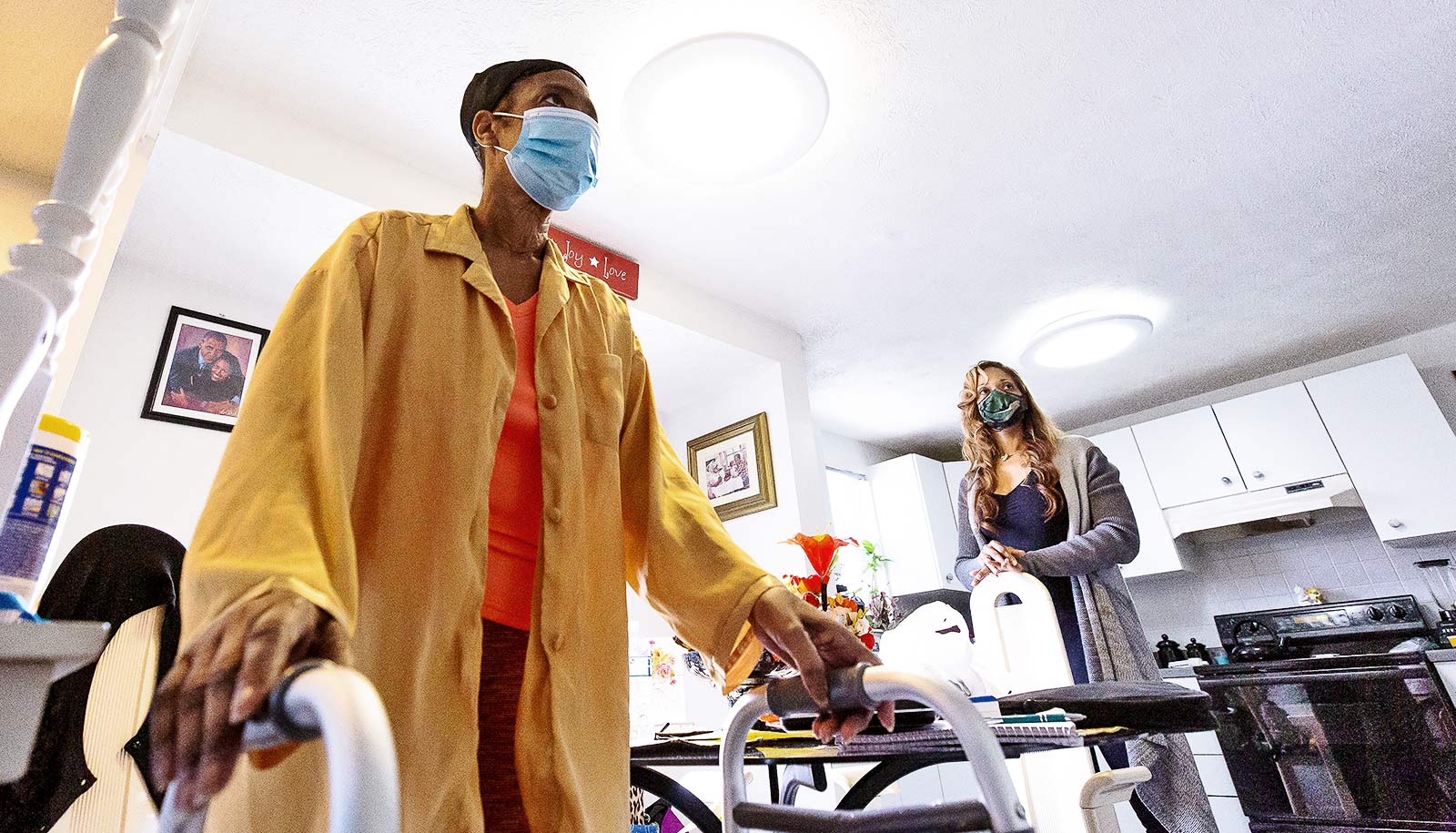
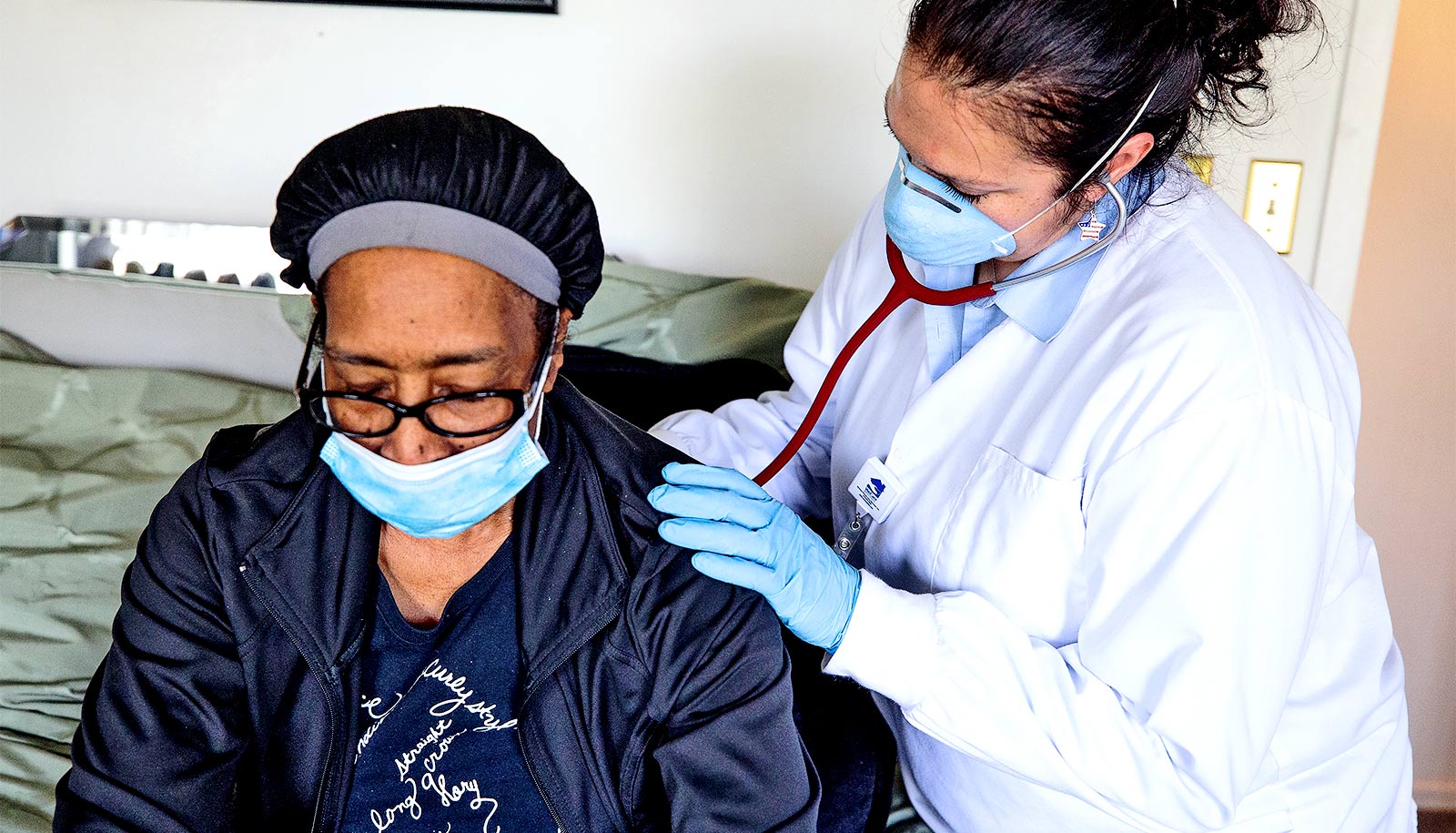
A new study shows that many patients hospitalized for COVID-19 experienced significant functional decline after being discharged.
The researchers found that 45% of patients hospitalized for COVID-19 they studied experienced significant functional decline after being discharged.
Over a year after the novel coronavirus cemented its grip on the world, much of the conversation surrounding the disease remains simple: how many people died and how many survived?
“They survived, but these people left the hospital in worse physical condition than they started.”
But researchers say a devastating side effect between those two extremes has gone underreported—the loss of ability the virus causes.
“Rehabilitation needs were really, really common for these patients,” says Alecia K. Daunter, a pediatric physiatrist at Michigan Medicine at the University of Michigan and lead author of the paper in the journal PM&R.
“They survived, but these people left the hospital in worse physical condition than they started. If they needed outpatient therapy or are now walking with a cane, something happened that impacted their discharge plan.”
Loss of physical ability after COVID-19
The researchers reviewed charts of nearly 300 adult patients hospitalized for COVID-19 at Michigan Medicine during the pandemic’s first wave between March and April 2020. They analyzed patients’ discharge locations, therapy needs at the time of release, and if they needed durable medical equipment or other services.
Of survivors who experienced functional decline, 80% were referred for additional therapy after being discharged. Nearly 20% of all patients lost so much ability, they were not able to live independently after their release.
“Some of these people were working and many were living independently. To lose that level of function is meaningful.”
“These patients may have needed to move to a subacute facility, or they might have needed to move in with a family member, but they were not able to go home,” Daunter says. “This has a massive impact on patients and their families—emotionally and physically.”
The study period occurred in the pandemic’s infancy, as health care providers sought best practices to minimize exposures and manage patient overflow. As a result, 40% of patients never had a rehabilitation evaluation while hospitalized. That likely means, Daunter explains, that the number of patients losing ability is underreported.
“Physicians and others in the health care system were working appropriately to discharge patients,” she says. “They needed to keep patients safe while maximizing available beds and minimizing exposure to staff. I think that contributed to many people not being assessed by a therapist or PM&R physician. So, the things we do to in the hospital to maximize functioning, like mobility interventions and assessing activities of daily living, were not happening as often.”
Loss of daily function
COVID-19 can systematically damage various organ systems, causing neurological and musculoskeletal impairments.
However, the virus’ effect on daily functioning is not frequently described, which, given the magnitude of the current public health crisis, can’t be ignored any longer, says coauthor Edward Claflin, a Michigan Medicine physiatrist.
“These results help to highlight the true impact of the COVID-19 disease on our patients,” Claflin says. “They fill in that gap in knowledge about how patients with COVID recover and what kind of rehabilitation needs they have.”
The “first wave” study is a snapshot look at acute therapy needs during a time when knowledge of the unique virus was even more limited. The team hopes for additional research examining the long-term effects COVID has on functionality. However, health systems can use the current data to optimize rehabilitation evaluations and prepare resources for this underserved population, Daunter says.
“These problems are frequent, and the stakes are pretty high if we miss them, or allow them to progress during hospitalization,” she says. “Some of these people were working and many were living independently. To lose that level of function is meaningful. We want to make sure we’re addressing those needs, not just looking at the black and white, survival or death.”
The findings are just the tip of the iceberg when it comes to the effects of COVID on functioning, says senior author Anna Kratz, a clinical psychologist at Michigan Medicine.
“The major shifts in functioning that we highlight are important, but less dramatic declines in physical and cognitive functioning are likely to be found in nearly all previously hospitalized COVID patients,” Kratz says.
“And we know from decades of rehabilitation work that even subtle changes in functioning can derail a person’s life trajectory. Future work needs to focus on improving our ability to identify and treat people across the full range of the functional decline spectrum.”
Source: University of Michigan