Here’s what to do if you strongly suspect you have COVID-19 but get negative results on rapid tests.
A few weeks back, my partner and I attended a wedding where, it turns out, love wasn’t the only thing in the air. Within 36 hours, a dozen attendees reported positive COVID-19 tests—which means they may have been infected before the wedding. At least a dozen more positives followed.
Soon, I started to feel a tickle in my throat and my partner started coughing. We were able to lock down for the week with work-from-home, grocery deliveries, and isolation from each other. I didn’t get sicker, but he did, with a phlegmy cough, congestion, and a slight fever. We both took several rapid tests and I also used Nucleic Acid Amplification Tests, which are more sensitive.
Neither of us ever tested positive. But we wonder whether we still “had COVID” in some sense, and it was a hard question to investigate on our own.
Fortunately, in my job, I get to talk to scientific experts—and who better to tap for infectious disease knowledge than Benjamin Pinsky, a Stanford School of Medicine professor of pathology and of medicine who works in clinical practice, and researches and designs infectious disease diagnostics and testing?
Pinsky, medical director for the Clinical Virology Laboratory for Stanford Health Care and Stanford Medicine Children’s Health, answered all the questions that raced through my mind during quarantine.
The main takeaway? Take a deep breath, do your research, be honest and thoughtful about your situation, and do the best you can for yourself and others.
“It’s important for folks to take stock of their own risk and their personal responsibility to others with the information they have at the time,” says Pinsky. “But it’s hard to make these sorts of decisions with imperfect information—that’s the challenge.”
The following Q&A has been lightly edited for clarity and consistency:
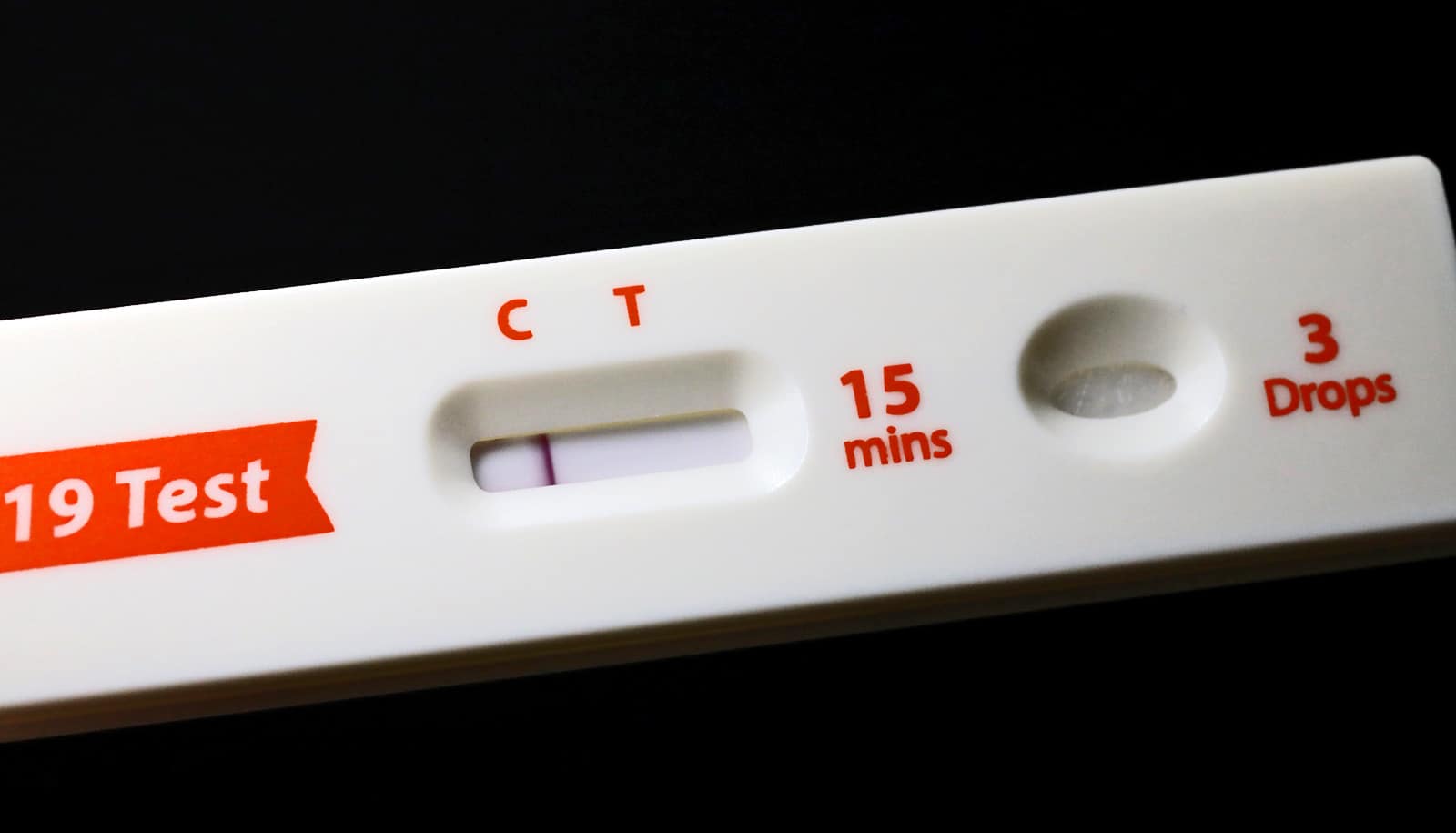
How dependable are rapid COVID-19 tests? And can people use the darkness of the positive line to gauge how infectious they are?
Mounting evidence in the literature points to only modest sensitivity in rapid tests, even in symptomatic individuals. Overall, the latest Cochrane Review, a large meta-analysis of rapid test sensitivity, showed the sensitivity was around 70%. That’s a lot of folks who will test negative with the rapid antigen test but are actually infected.
The nucleic acid amplification tests [which is what the author of this article used] are much more sensitive. But for this type, you swab on the inside of the nostrils, which are less sensitive than those that go farther into the nasal cavity.
Another thing to think about is frequency of testing. The viral load increases, peaks, and then starts to wane. You can improve the overall test performance by serial sampling.
The darkness of the line, and the time in which it turns positive may be correlated with the amount of virus in that specimen. But there’s so much variability in how people do the test, the rapid tests should be used only as a yes or no answer.
What is the strict definition of “having” COVID-19? If someone finds themselves in the situation I was in—with a likely COVID-19 infection but no positive test—what should they do?
Strictly defining what it means to “have” COVID-19 is really hard. Technically, the definition of infection is being able to detect the virus in a clinical specimen.
In reality, you can be infected and have it fly under the radar of the medical system. There are probably folks who are infected and do not test positive with any of our tests. Maybe some people never have a viral load that’s high enough. That being said, we’d probably detect most of those infections if people were tested at the right time.
You can also try to figure it out after the fact if you are—and I love this term—”immuno-curious.” You or your partner could potentially be tested for antibodies. But even this depends on getting the timing right.
If you’re sick, you don’t need to have the diagnosis to isolate. But if you can’t isolate yourself and have even mild symptoms, you should get a molecular test. Preferably, get the most sensitive one, with the far-back swab, done by a professional—I suspect that your partner would probably have been positive with that kind of test.
If you’re subsequently negative with the most sensitive testing, it’s likely that you do not have SARS-CoV-2. However, if you still have symptoms and you’re able to isolate, you should.
The main goal is to be less likely to transmit. That gets really tricky and asks for a lot of personal responsibility. Consider whether you’re likely to interact with folks that are elderly, immunocompromised, or not vaccinated—all those sorts of things.
Increasingly, it seems like people are working while they have symptoms of illness, but they’re convinced it’s not COVID-19 because they’ve been testing.
That’s a bit concerning because most people test with rapid antigen tests and its performance is not ideal. On the other hand, if you’re antigen negative, it means you probably don’t have a lot of virus, so you’re not as likely to transmit; that is, if your sample was taken at the right time. Unless you’re testing continually, you don’t know whether you’re on the way up or on the way down in terms of viral load. So, I don’t really trust that argument for making public health or individual decisions.
Another common refrain is, “Well, there are still other illnesses,” referring to colds and the flu. But is it likely someone has one of those, rather than COVID-19?
That statement is accurate, in the strictest sense, except that over the past two years, there’s been very little circulation of other respiratory viruses. It’s likely, also, that COVID-19 is more transmissible, at least in the current world.
The first year of the pandemic, with masking and social distancing rules, we had very few cases of influenza in the specimens we tested at the Clinical Virology Laboratory. Separately, for a study, we tested 15,000 specimens that were negative for COVID-19 and we found one case of respiratory syncytial virus, or RSV, a common cold-like virus. That’s it.
We’ve seen other respiratory viruses come back as we’re “opening back up.” But at Stanford Health Care, in adults, the circulation of respiratory viruses is still low. In pediatrics, we’re getting a lot of cases of non-COVID-19 respiratory viruses, mostly rhinovirus and RSV. Now, that we’re moving into the respiratory virus season, we’ll be keeping a close eye out for an uptick in non-COVID-19 viruses, particularly influenza.
Part of your work aims to help us tackle some of those unknowns about infection status. What exciting examples can you share?
We’re still working on various SARS-CoV-2 diagnostic tests. We’re trying to use host response to the virus to diagnose SARS-CoV-2 and other respiratory virus infections—specifically looking at metabolites, which a body generates in response to infection. The idea would be to identify all the small metabolites on a swab using a technique called mass spectrometry, which would give a chemical signature that indicates whether a person is infected.
We’re hoping to move the process to more portable mass spectrometers that are less expensive and easier-to-use—similar to those used in airport security lines to analyze swabs for chemical traces of explosives. It would be really cool if it works out because the time to result would be one to two minutes.
We’ve also developed a test that used mostly to check whether hospitalized patients still have replicating virus when they meet criteria for removal from isolation. The SARS Coronavirus is a “plus-stranded” RNA virus, which means the infected host cell makes a “minus strand” of RNA during replication. If a test detects only that minus strand, we can identify patients that are most likely to be replicating.
A lot of this research and what we’ve learned throughout the pandemic will inform how we behave for future respiratory infections.
Source: Stanford University