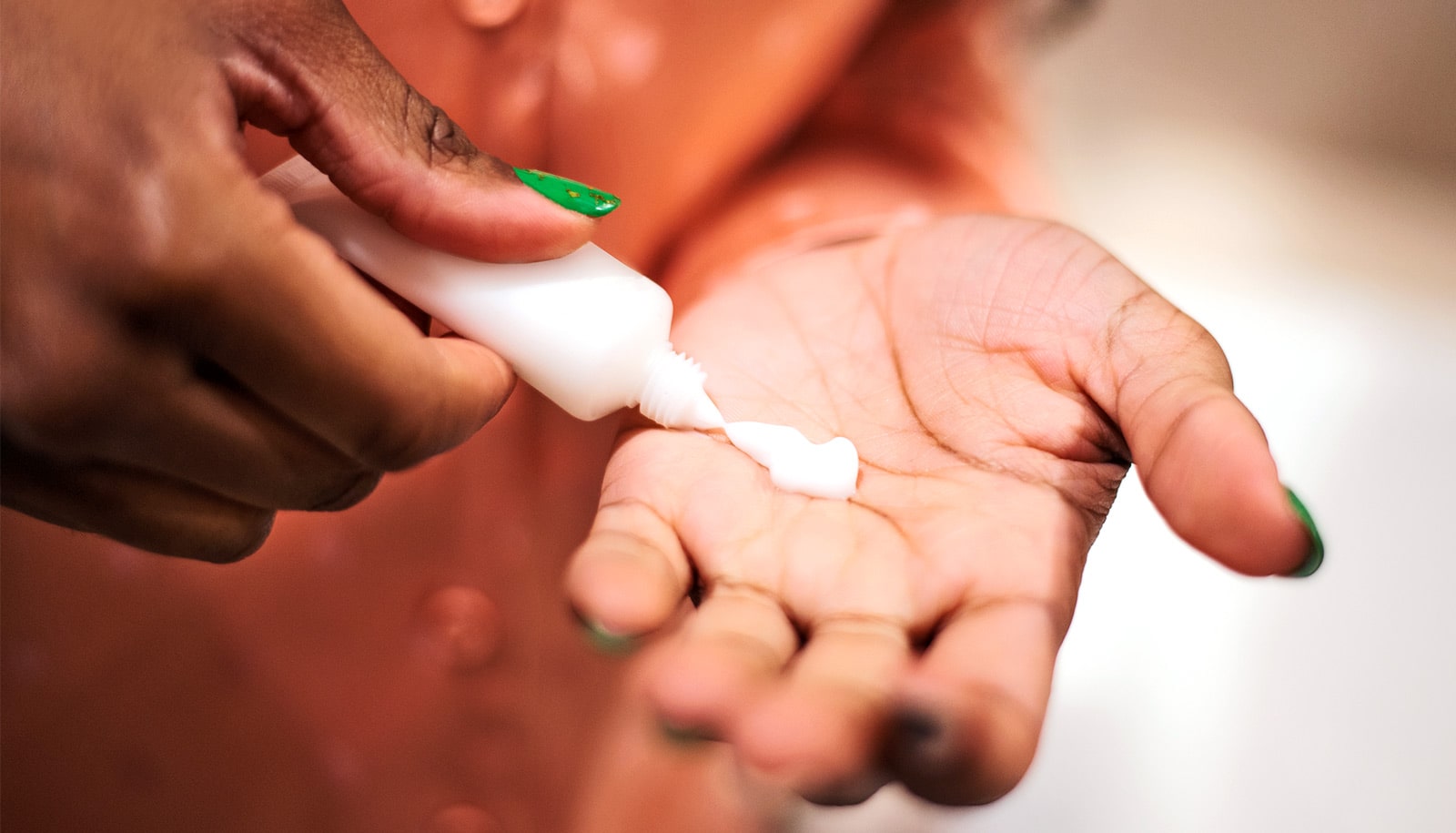
Rice University seniors are developing an efficient and inexpensive uterine contraction monitor to help save the lives of mothers in labor and their newborns in resource-poor settings.
A team of bioengineering students at Rice University designed, built, and programmed a sensor to monitor women in labor, as well as a unique test rig. They plan to validate the monitor’s accuracy with the help of faculty at the University of Texas Health Science Center at Houston (UTHealth) and their patients.
“…the patient-to-nurse ratio is 15-to-1, so it’s not physically possible to adequately monitor all the patients.”
Eventually, the monitor will likely undergo tests in maternity wards at hospitals in Malawi, where the Rice 360˚ Institute for Global Health is working to solve the challenges they and other low-resource hospitals face.
“Maternal mortality is a large problem in Malawi,” says Leah Sherman, one of two team members who has spent time there with Rice 360˚. “We’ve seen the wards, which isn’t something you can easily forget, and we all have a passion for bringing the maternal mortality rate down. Of all of the bioengineering projects we were offered, this one seemed the most powerful and impactful for a community that is in dire need.”
Sherman and Mildred Antwi-Nsiah, who has also worked in Malawi, worked with teammates at Rice’s Oshman Engineering Design Kitchen (OEDK), where some designed and programmed the sensor and monitoring algorithm and others pieced together a method to test their invention.
“In Malawi, nurses are supposed to perform a partograph, in which they manually measure contractions every 30 minutes for 10 minutes, but the patient-to-nurse ratio is 15-to-1, so it’s not physically possible to adequately monitor all the patients,” Sherman says. “Most mothers there go unmonitored for the majority of their labor.”
The heart of the new device is a puck-like sensor that presses against the patient’s abdomen and stays in place thanks to a robust, washable rubber and nylon belt designed to lessen the need for disposable supplies and cut the risk of infection.
Contracting muscles move a membrane on the sensor, which in turn moves an LED on the inside closer to a photoresistor that measures the intensity of the light and determines the voltage output to a microcontroller. That sends information about the contractions to the user interface in real time.
When contractions become more frequent or indicate a risk to the patient, a box attached to the computer will light up and sound an alarm, Antwi-Nsiah says. “When they’re outside of a safe physiological range for more than 10 minutes, the audible and visual cues will become more intense,” she says.
Because contractions can last between 30 seconds and three minutes, the team’s test device had to deliver a gradual increase and decrease in pressure to the sensor. A beach ball hooked to a set of microcontroller-controlled solenoids was the answer. “We started with a hand pump, but it was hard to get the nice, smooth curves you would get in real life,” says team member Catherine Schult.
The team designed the contraction monitor to cost less than $100.
Prep for fetal surgery involves kickball, chicken breasts
The students plan to test the monitor under the supervision of Suneet Chauhan, a professor in UTHealth’s department of obstetrics, gynecology, and reproductive sciences.
Validation will take place in parallel with devices that UTHealth faculty use in their practices, though the Rice team won’t hook up its graphical interface so attending physicians will only have access to their own monitors, Schult says. “Also, for some women who have higher-risk pregnancies, they often monitor them with an intrauterine pressure catheter (IUPC), which is the gold standard and very accurate.
“If our device detects 70 percent of contractions relative to those detected by that (IUPC) technology, it will be equivalent to the tocodynamometer used in the United States, which is our base goal.”
Co-advisors of the team are OEDK director Maria Oden, a teaching professor in bioengineering; Eric Richardson, a lecturer in bioengineering; and Jennifer Carns, a postdoctoral researcher in the lab of Rice 360˚ director Rebecca Richards-Kortum.
The team will demonstrate its device at the annual George R. Brown School of Engineering Design Showcase April 12.
Source: Rice University