It may be possible in the future to screen patients for Alzheimer’s disease using a simple eye exam, according to new research.
Using technology similar to what is found in eye doctors’ offices, researchers have detected evidence indicating Alzheimer’s disease in older patients who had no symptoms.
“This technique has great potential to become a screening tool that helps decide who should undergo more expensive and invasive testing for Alzheimer’s disease prior to the appearance of clinical symptoms,” says first author Bliss E. O’Bryhim, a resident physician in the ophthalmology & visual sciences department at Washington University in St. Louis.
“Our hope is to use this technique to understand who is accumulating abnormal proteins in the brain that may lead them to develop Alzheimer’s.”
Hear co-principal investigator Gregory Van Stavern discuss the findings:
Thinning retina
Significant brain damage from Alzheimer’s disease can occur years before any symptoms such as memory loss and cognitive decline appear. Scientists estimate that Alzheimer’s-related plaques can build up in the brain two decades before the onset of symptoms, so researchers have been looking for ways to detect the disease sooner.
Physicians now use PET scans and lumbar punctures to help diagnose Alzheimer’s disease, but they are expensive and invasive.
In previous studies, researchers reported that the eyes of patients who had died from Alzheimer’s disease showed signs of thinning in the center of the retina and degradation of the optic nerve.
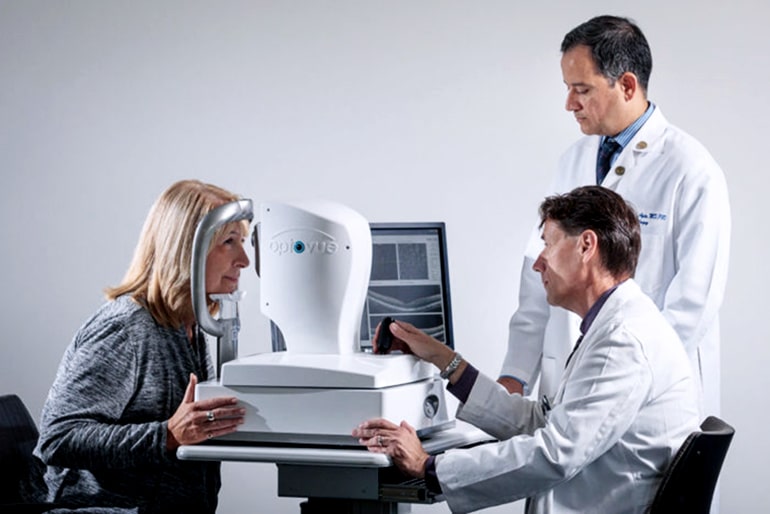
In the new study, which appears in JAMA Ophthalmology, researchers used a noninvasive technique—called optical coherence tomography angiography—to examine the retinas in eyes of 30 study participants with an average age in the mid-70s, none of whom exhibited clinical symptoms of Alzheimer’s disease.
Participants were patients in the Memory and Aging Project at Washington University’s Knight Alzheimer’s Disease Research Center. About half of those in the study had elevated levels of the Alzheimer’s proteins amyloid or tau as revealed by PET scans or cerebrospinal fluid, suggesting that although they didn’t have symptoms, they likely would develop the disease. In the other subjects, PET scans and cerebrospinal fluid analyses were normal.
Blood flow
“In the patients with elevated levels of amyloid or tau, we detected significant thinning in the center of the retina,” says co-principal investigator Rajendra S. Apte, distinguished professor of ophthalmology and visual sciences.
“All of us have a small area devoid of blood vessels in the center of our retinas that is responsible for our most precise vision. We found that this zone lacking blood vessels was significantly enlarged in people with preclinical Alzheimer’s disease,” Apte says.
The eye test researchers used in the study shines light into the eye, allowing a doctor to measure retinal thickness, as well as the thickness of fibers in the optic nerve. A form of that test often is available in ophthalmologist’s offices.
“The retina and central nervous system are so interconnected that changes in the brain could be reflected in cells in the retina,”
For the current study, however, researchers added a new component to the more common test: angiography, which allows doctors to distinguish red blood cells from other tissue in the retina.
“The angiography component allows us to look at blood-flow patterns,” says Gregory P. Van Stavern, professor of ophthalmology and visual sciences. “In the patients whose PET scans and cerebrospinal fluid showed preclinical Alzheimer’s, the area at the center of the retina without blood vessels was significantly larger, suggesting less blood flow.”
“The retina and central nervous system are so interconnected that changes in the brain could be reflected in cells in the retina,” Apte adds.
Of the patients studied, 17 had abnormal PET scans and/or lumbar punctures, and all of them also had retinal thinning and significant areas without blood vessels in the centers of their retinas. The retinas appeared normal in the patients whose PET scans and lumbar punctures were within the typical range.
More studies in patients are needed to replicate the findings, Van Stavern says, noting that if changes detected with this eye test can serve as markers for Alzheimer’s risk, it may be possible one day to screen people as young as their 40s or 50s to see whether they are at risk for the disease.
“We know the pathology of Alzheimer’s disease starts to develop years before symptoms appear, but if we could use this eye test to notice when the pathology is beginning, it may be possible one day to start treatments sooner to delay further damage.”
Research to Prevent Blindness and a grant from Optovue Inc. funded the work.