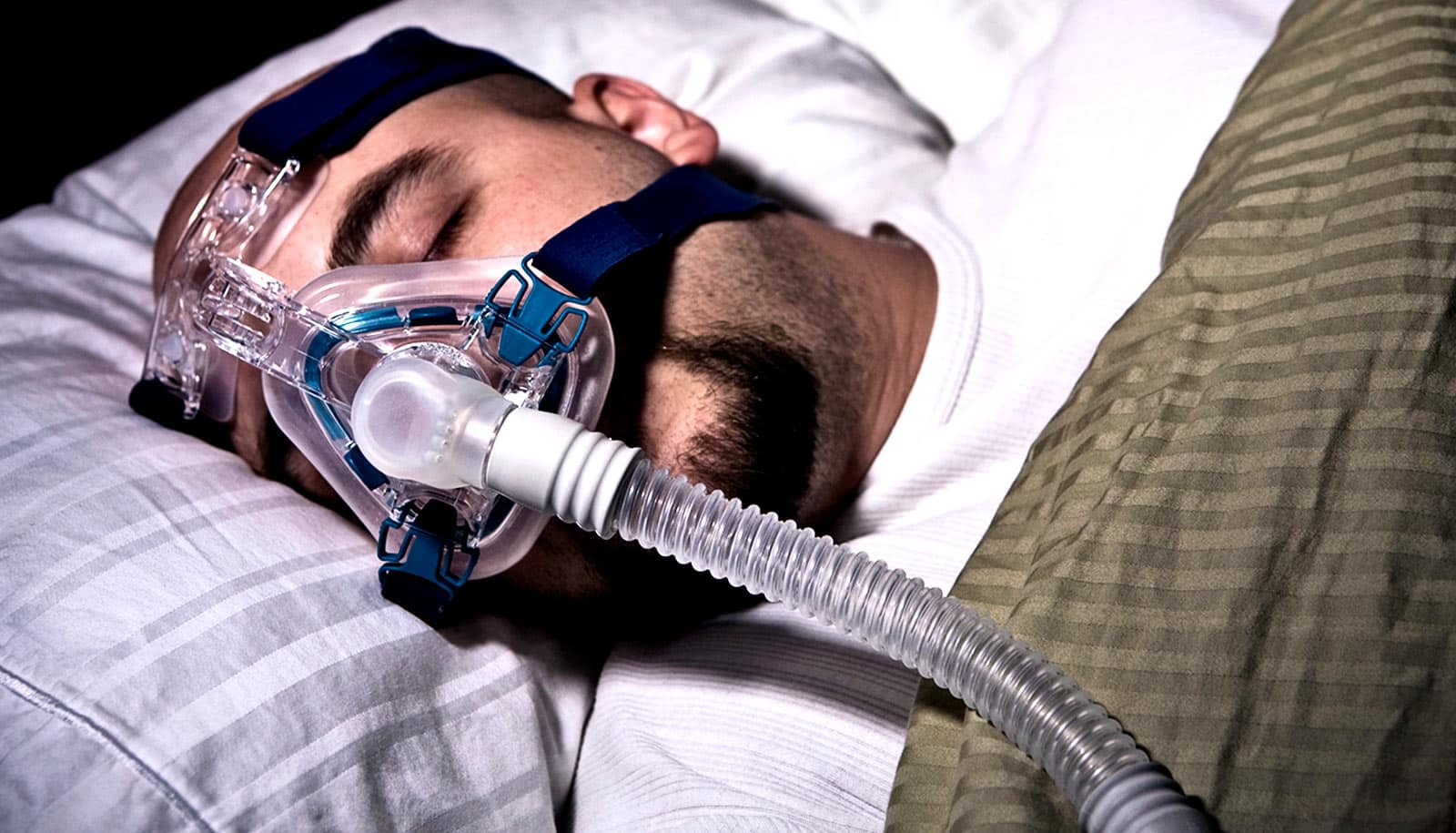
Improvements in sleep apnea symptoms due to weight loss appear to be linked to fat reduction in the tongue, researchers have discovered.
Using magnetic resonance imaging (MRI) to measure the effect of weight loss on the upper airway in patients with obesity, researchers found that reducing tongue fat is a primary factor in lessening the severity of obstructive sleep apnea (OSA).
“Most clinicians, and even experts in the sleep apnea world, have not typically focused on fat in the tongue for treating sleep apnea,” says Richard Schwab, chief of sleep medicine in the Perelman School of Medicine at the University of Pennsylvania. “Now that we know tongue fat is a risk factor and that sleep apnea improves when tongue fat is reduced, we have established a unique therapeutic target that we’ve never had before.”
Sleep apnea and our tongues
Twenty-two million Americans suffer from sleep apnea, a serious health condition in which breathing repeatedly stops and starts, causing patients to wake up randomly throughout their sleep cycles. The condition, which is usually marked by loud snoring, can increase your risk for high blood pressure and stroke. While obesity is the primary risk factor for developing the condition, there are other causes, such as having large tonsils or a recessed jaw.
CPAP (continuous positive airway pressure) machines improves sleep apnea in about 75% of patients, studies suggest, but for the other 25%—those who may have trouble tolerating the machine—alternative treatment options, such as oral appliances or upper airway surgery, are more complicated.
A 2014 study led by Schwab compared patients with obesity with and without sleep apnea, and found that the participants with the condition had significantly larger tongues and a higher percentage of tongue fat when compared to those without the condition. The researchers’ next step was to determine if reducing tongue fat would improve symptoms and to further examine cause and effect.
The new study included 67 participants with mild to severe obstructive sleep apnea who were obese —those with a body mass index greater than 30.0. Through diet or weight loss surgery, the patients lost nearly 10% of their body weight, on average, over six months. Overall, the participants’ sleep apnea scores improved by 31% after the weight loss intervention, as measured by a sleep study.
Before and after the weight loss intervention, the study participants underwent MRI scans to both their pharynx as well as their abdomens. Then, using a statistical analysis, the research team quantified changes between overall weight loss and reductions to the volumes of the upper airway structures to determine which structures led to the improvement in sleep apnea. The team found that a reduction in tongue fat volume was the primary link between weight loss and sleep apnea improvement.
The study also found that weight loss resulted in reduced pterygoid (a jaw muscle that controls chewing) and pharyngeal lateral wall (muscles on the sides of the airway) volumes. Both these changes also improved sleep apnea, but not to the same extent as the reduction in tongue fat.
Getting better rest
The authors believe that tongue fat is a potential new therapeutic target for improving sleep apnea. They suggest that researchers could design future studies to explore whether certain low-fat diets are better than others in reducing tongue fat and whether cold therapies—like those used to reduce stomach fat—might apply to reducing tongue fat. However, Schwab notes, these types of interventions have not yet been tested.
Schwab’s team is also examining new interventions and other risk factors for sleep apnea, including whether some patients who don’t have obesity but who have “fatty” tongues could be predisposed to the condition, but are less likely to get a diagnosis.
In a recent related study, Schwab found that ethnicity may also play a role in sleep apnea severity. His research team compared the upper airway anatomy of Chinese and Icelandic patients with sleep apnea, and found that, compared to Icelandic patients of similar age, gender, and symptoms, Chinese patients had smaller airways and soft tissues, but bigger soft palate volume with more bone restrictions. This means that Asian patients may generally be more at risk for severe sleep apnea symptoms.
The bottom line, according to Schwab, is that all patients who suffer from snoring or sleepiness should have a sleep apnea screening, whether or not they appear to fall into the typical “high-risk” obesity categories.
“Primary care doctors, and perhaps even dentists, should be asking about snoring and sleepiness in all patients, even those who have a normal body mass index, as, based on our data, they may also be at risk for sleep apnea,” Schwab says.
The National Institutes of Health supported the work.
The research appears in the American Journal of Respiratory and Critical Care Medicine.
Source: Penn