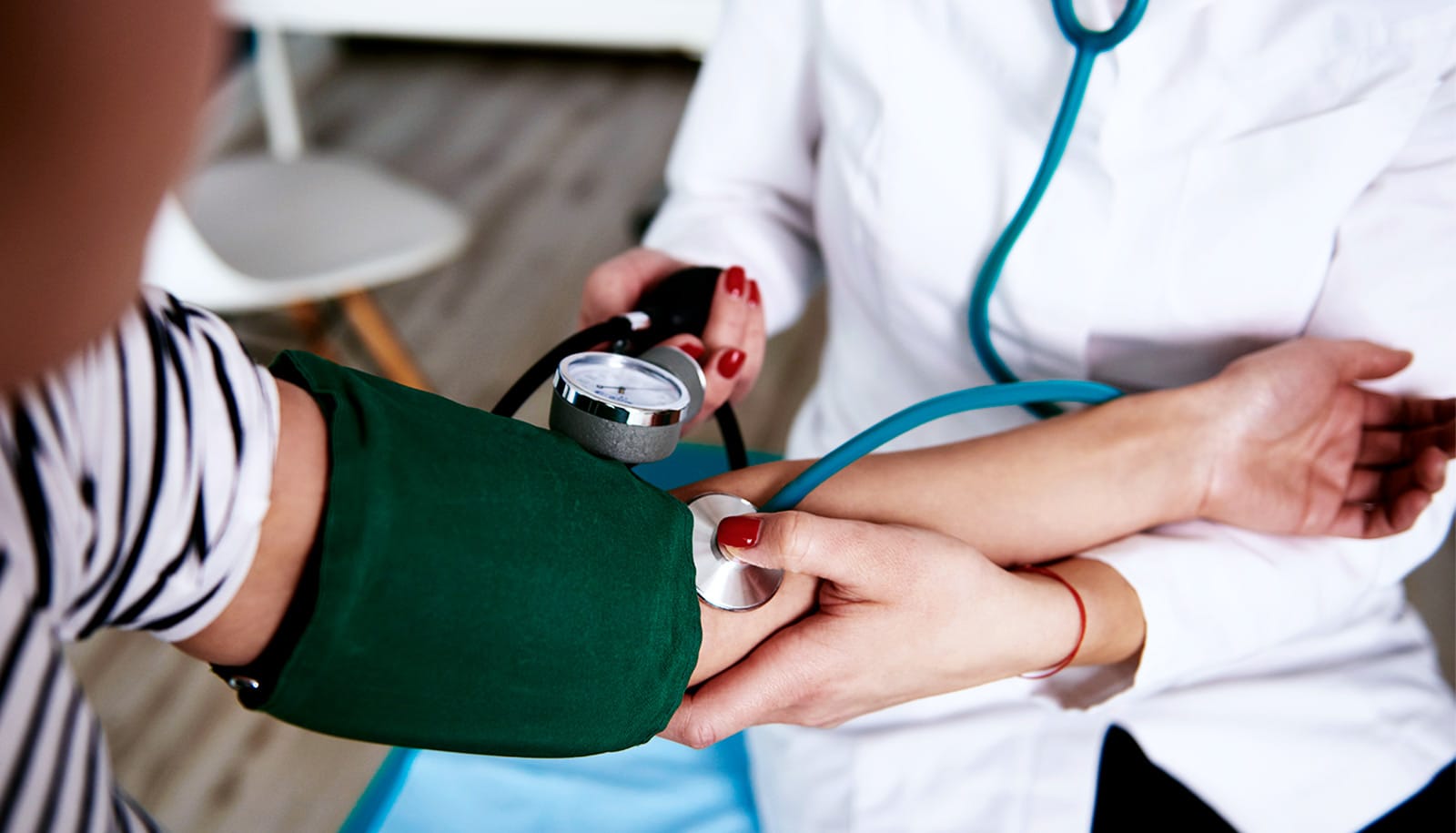
Complications from pregnancy and childbirth can have deadly implications as much as 50 years later.
Conditions like high blood pressure in pregnancy, gestational diabetes, and preterm delivery were all tied to a greater risk of death in the decades following delivery, according to the study in the journal Circulation, which used long-range, racially-inclusive data.
“We know that the context of childbirth has changed since the 1950s and ’60s, but these findings demonstrate how crucial it is to people’s long-term health that we invest in preventive care and screenings for people with complicated pregnancies and deliveries, both then and today,” says lead author Stefanie Hinkle, an assistant professor of epidemiology at Penn Medicine.
In the United States, more than 800 people die every year giving birth. The latest number shows that, out of every 100,000 births, more than 23 result in the death of the person delivering.
France’s maternal death rate is the next highest among peer countries, and the United States’ death rate is still three times as high. These figures account for deaths in childbirth and during the immediate postpartum period, but the long-term effects of complicated childbirths—which can lead to serious, lifelong health conditions such as heart disease, diabetes, and more—have often been overlooked.
Hinkle and her coauthors drew on data collected from more than 46,000 people who’d given birth at a dozen United States health centers between 1959 and 1966. The patients were tracked for deaths of any kind until 2016, at which time 39%, roughly 18,000, had died.
In their analysis, the researchers found that a pre-term childbirth (a delivery three weeks or more before the due date) due to spontaneous labor was tied to a 7% increase in risk of death compared to those who delivered a baby full-term.
The risk climbed to 23% for those whose water broke before term, 31% for preterm induced labor, and actually doubled—109%—for patients who had a pre-term caesarean delivery, all compared to those who hadn’t had these types of deliveries.
When it came to hypertensive disorders of pregnancy (high blood pressure conditions like preeclampsia, which can be life-threatening), the risk of death in subsequent years ranged from 9% for those with high blood pressure tied specifically to their pregnancy to 32% for those who already had high blood pressure before their pregnancy and then developed preeclampsia in their pregnancy.
Finally, gestational diabetes or high blood sugar levels in pregnancy increased the risk of death in the following decades by 14%.
As previous research has shown deaths in childbirth and the immediate postpartum period disproportionately affect Black people, Hinkle and her colleagues specifically attempted to focus on an area of the research that is largely missing: Differences in outcomes by race.
“The value of these data is that they provide more inclusive findings, extending what has been mostly limited to predominately white samples to Black pregnant people, as well,” Hinkle says. “It is essential for individuals to know that they are represented in data that leads to clinical recommendations.”
Overall, the death rate for Black patients was higher than white patients (41% of the Black patients in the sample compared to 37% of white patients). Pre-term delivery—and, thus, the risk of pregnancy complications—was much more common, comparatively, in Black patients than white patients (20 to 9).
Hinkle believes more research is needed to study whether these findings point to pregnancy complications being “causal” in mortality or “just predictive by revealing an underlying risk.”
“Future work should seek to understand whether intervening earlier in the postpartum period among high risk patients prevents future disease incidence,” Hinkle says. “Our group is also currently working to identify low-cost interventions to potentially prevent complicated pregnancies and deliveries.”
The Eunice Kennedy Shriver National Institute of Child Health and Human Development funded the work.
Source: Penn