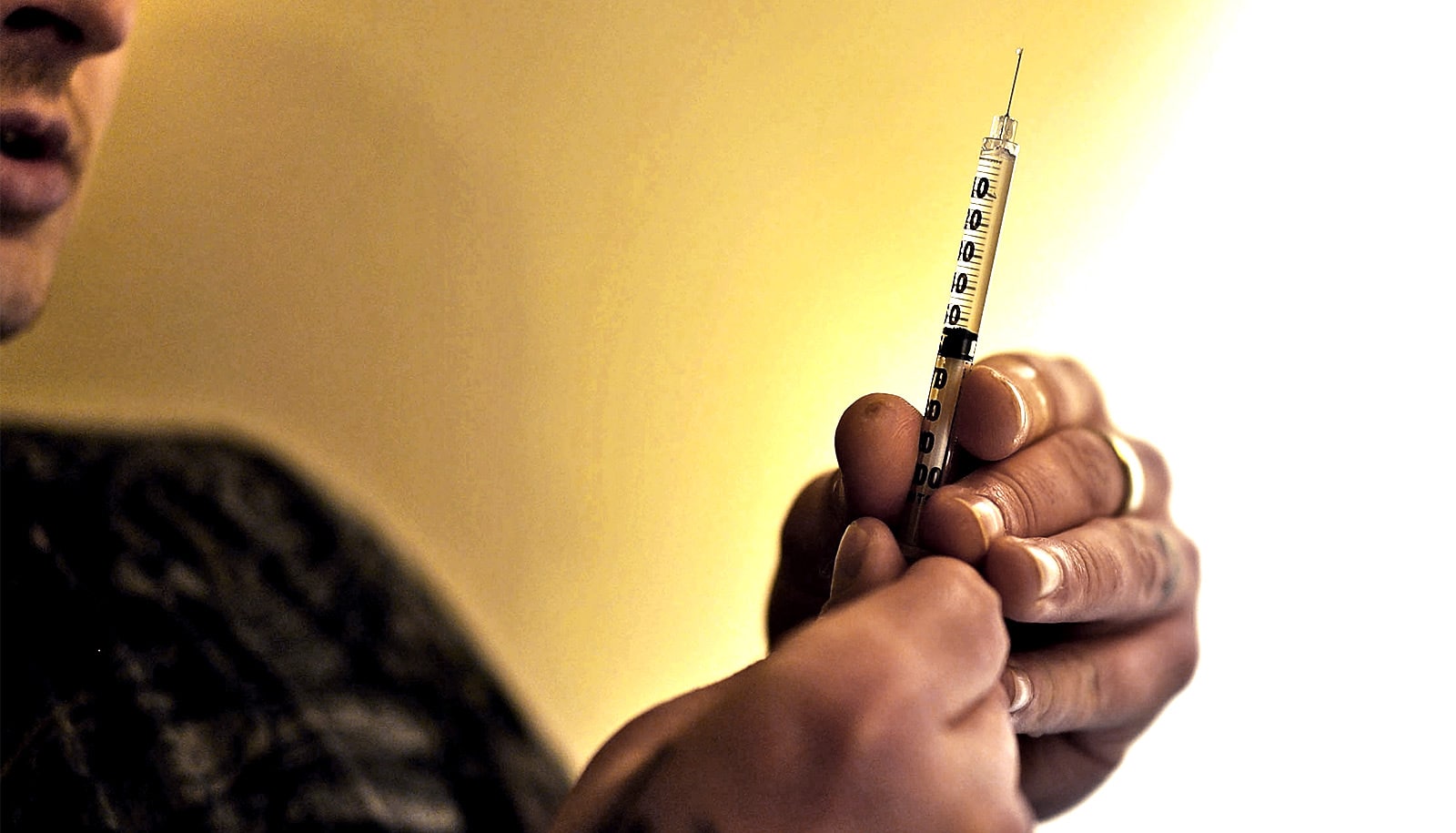
Overdose prevention centers, where individuals can consume illicit drugs under the observation of trained staff, are not associated with significant increases in crime, a new study finds.
When the researchers compared syringe service programs in New York City with two programs that were recently sanctioned by city officials to offer supervised drug consumption, they found no significant increases in crimes recorded by the police or calls for emergency service in the surrounding neighborhoods.
The findings, which are published in JAMA Network Open, come as plans to open overdose prevention centers proceed in Rhode Island, Massachusetts, and elsewhere, and not long after lawmakers in Philadelphia passed a preemptive measure to ban these types of centers, says coauthor Brandon del Pozo, an assistant professor (research) at Brown University’s Warren Alpert Medical School and School of Public Health.
“What this data shows is that if a neighborhood benefits from an established syringe service program, then adding the service of supervised drug consumption is not likely to increase reported crime, disorder complaints, or related calls to 311 and 911,” del Pozo says.
Even in New York, del Pozo adds, the federal prosecutor for Manhattan characterized the city’s OPCs as unlawful and threatened to close them. Yet, according to the study, concerns about OPC-caused crime and disorder are unfounded, del Pozo says.
“To those who worry that opening overdose prevention centers will increase crime in neighborhoods that need these types of programs, I would say that our analysis does not bear that out.”
In late November 2021, the first officially sanctioned US overdose prevention sites began operation in New York. The two sites are operated by OnPoint NYC, a harm reduction coalition, in the Manhattan communities of East Harlem and Washington Heights, at the locations of long-established syringe service programs that provide people with access to naloxone, harm reduction resources, and connections to treatment for substance use disorder and infectious diseases.
By February 2023, more than 2,300 clients had visited the overdose prevention centers approximately 55,000 times, requiring over 700 overdose interventions—with no fatalities.
To evaluate the effect of the two new overdose prevention centers on crime and disorderly behavior, the researchers analyzed five administrative datasets placed in the public domain by the city of New York. These included criminal complaints, arrest reports, criminal court summonses, and 911 and 311 call records—from January 2019 through December 2022.
They compared crime and disorder complaints in 17 neighborhoods that had brick-and-mortar syringe service programs with the two programs that had been converted to overdose prevention centers, from two years before the OPCs opened to one year after.
To augment their results, they also looked at other city locations with similar levels of felony crime reports and drug arrests during the two years before the overdose prevention centers began operating.
The researchers found no significant changes in violent crimes, property crimes recorded by police, 911 calls for crime, medical incidents, or 311 calls regarding drug use or “unsanitary” conditions observed in the vicinity of the OPCs, and observed significant reductions in calls for homeless-related conditions.
The researchers concluded that initial data from New York City do not support concerns about crime and disorder that threaten to hamper the expansion of overdose prevention centers in other US cities.
“According to these measures, reports of crime changed very little in the neighborhoods surrounding OPCs,” del Pozo says.
“Moving forward, we must continue to conduct research to see how law enforcement and public health practitioners, especially harm reduction groups, can continue to effectively collaborate law enforcement and public health practitioners, especially harm reduction groups, can effectively collaborate on solutions to the opioid crisis in America.”
Additional coauthors are from the University of Pennsylvania and the University of Connecticut School of Public Policy.
The National Institute on Drug Abuse, part of the National Institutes of Health, supported the work. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Source: Brown University