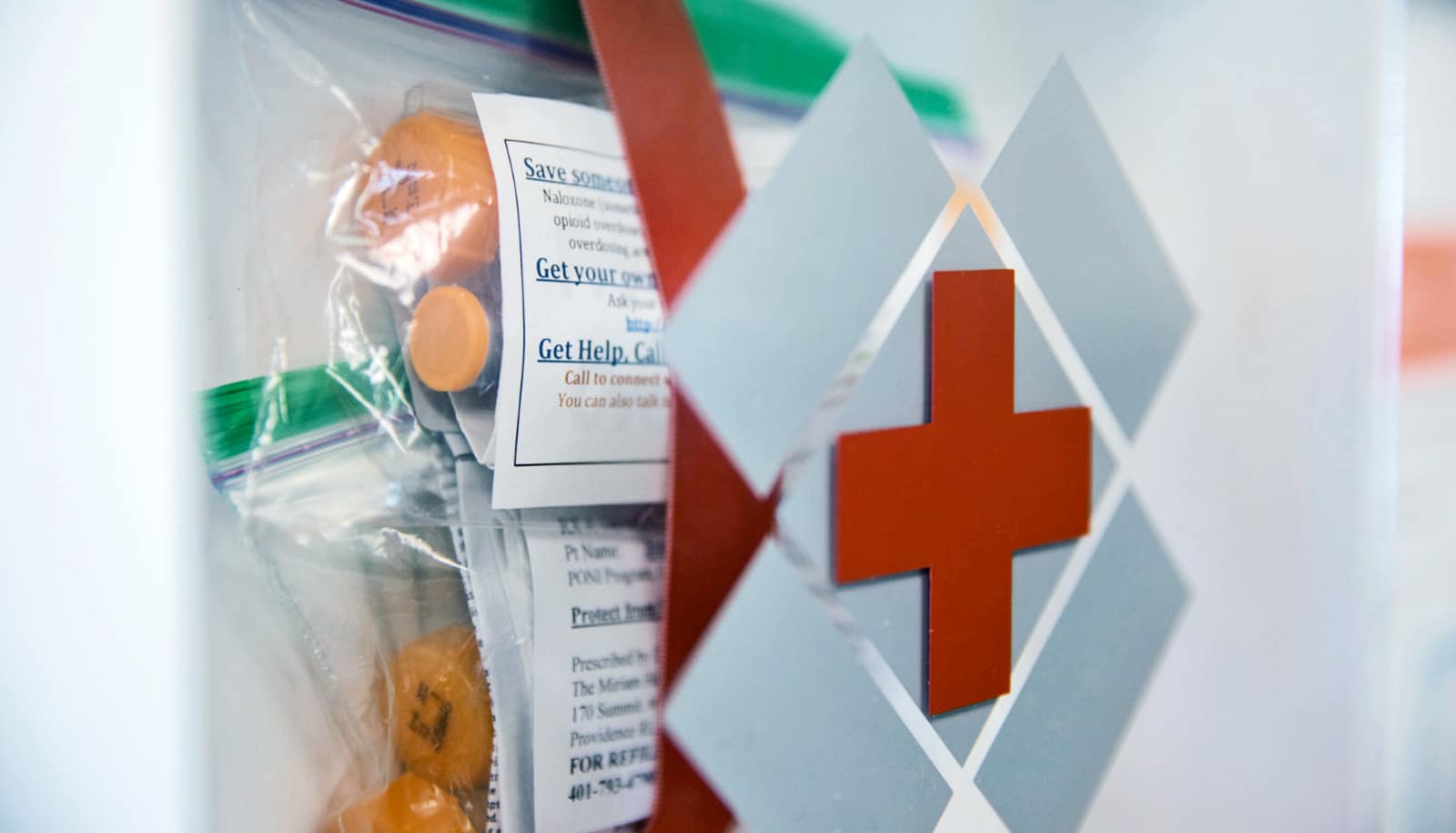
Placing a new kind of emergency medicine kit called a “NaloxBox” that contains anti-overdose medication in public places could allow bystanders to prevent drug overdoses, the creators say.
On the night of Saturday, June 3, just six days before Amos House installed six “NaloxBoxes”—wall-mounted kits with doses of the opioid overdose reversing medicine naloxone—a resident nearly died of an overdose.

In that case, the affected woman, who was found on the floor of a bathroom, survived because fellow residents happened to have their own naloxone and were ready to act, says Eileen Hayes, director of the homelessness and recovery services center on Pine Street in Providence, Rhode Island. But now there are NaloxBoxes arrayed strategically around the center’s main building and residences so that the medicine will always be within reach to residents and staff alike.
“It’s crucial that we educate people and make it available,” Hayes says. “We’re a recovery program, and we’re working with men and women who are really working hard to be in recovery, and yet that doesn’t mean that relapse doesn’t happen.”
Professors Geoff Capraro of the Warren Alpert Medical School of Brown University and Claudia Rébola of the Rhode Island School of Design created NaloxBoxes. Capraro, a Lifespan emergency medicine physician, had the idea that naloxone should be made readily available in public places where overdoses may occur. He brought the idea to RISD, where Rébola has ultimately led the boxes’ design.
“…we saw potential for putting this medicine in the hands of bystander good Samaritans…”
What they’ve developed is an emergency kit with the same goals as a fire extinguisher or an automated external defibrillator—to enable anyone in the wrong place at the right time to save lives.
Nationally, drug overdoses are rising sharply, mostly because of opioids like heroin or prescription painkillers. The epidemic is especially severe in Rhode Island, where 336 people died from overdoses in 2016 alone, prompting a series of programs and actions by the governor including an executive order signed just today.
“There’s no publicly available naloxone,” Capraro says. “It’s all by prescription or pharmacy dispensed. So we saw potential for putting this medicine in the hands of bystander good Samaritans so they could give it quickly. The time to deliver the medicine matters.”
With grant support from the Rhode Island Department of Health and the Preventing Overdose and Naloxone Intervention program at the Miriam Hospital, Capraro and Rébola produced 48 boxes this spring. They have begun to install them this summer, conducting trainings in opiate overdose recognition and rescue in conjunction with the installations, beginning at Amos House and continuing at least 12 other community facilities such as shelters within the Rhode Island Coalition for the Homeless.
Deadly overdoses can cluster in unexpected places
The boxes, not much bigger than a ream of office paper, contain four injectable doses of naloxone, printed instructions for how to administer it, and a mask for providing rescue breaths (in an overdose, people stop breathing).
The boxes are also being outfitted with cellular electronics that send a simple text message to their host when they are opened. That way, whoever is responsible for the box is alerted when someone has used it, so that the possible emergency is documented and any taken naloxone can be refilled.
The design is simple, but it carries many intentional choices aimed at making the drug available quickly and keeping it stocked reliably and efficiently. Last fall, Rébola inherited the project from colleague Soojung Ham and continued design brainstorming with their industrial design students.
Each box displays a red logo on a clear plastic door to make the box recognizable without obscuring the contents. The door opens with a Velcro latch for easy access—no mechanism to manipulate, no glass to break, no codes to enter. Merely opening the box triggers the text message with no other action by the user.
The naloxone is held within a vertical elastic strap that is centered for equal access by right- or left-handed users. The boxes are also designed to accommodate other forms of naloxone packaging, not just one kind of injectable. Some future sites may prefer to stock the intranasal formulation, for instance.
“This is really linking health and design together,” Rébola says. “We have learned a lot through the process.”
With feedback from hosts and users and further funding, the duo hopes to continually improve the NaloxBox design and to install them in many more community service facilities and public spaces.
Rescue kits reduce opioid overdose deaths
“It can happen to anybody in any walk of life,” Capraro says. “Our distribution should reflect that distribution of the epidemic.”
Source: Brown University