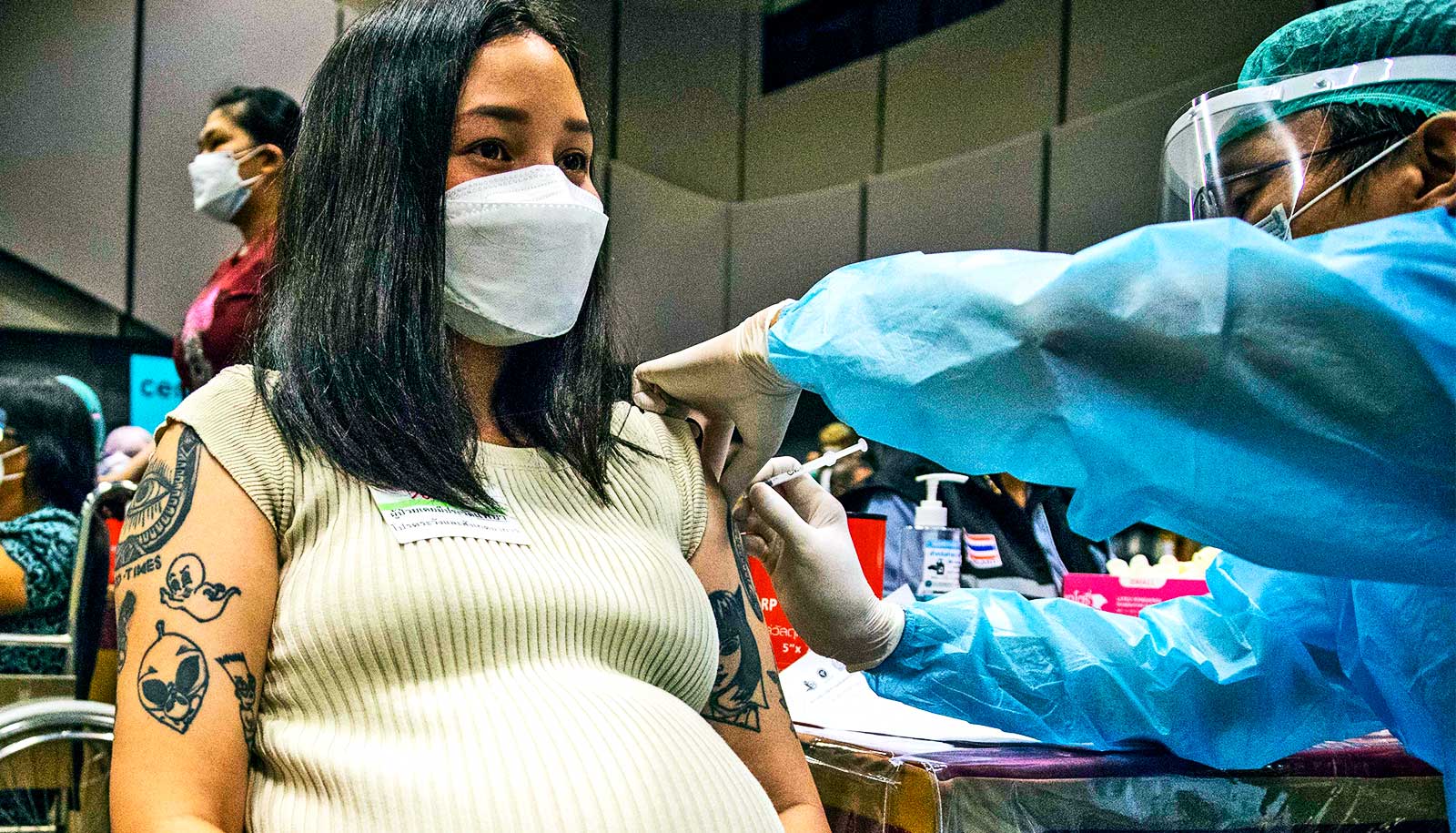
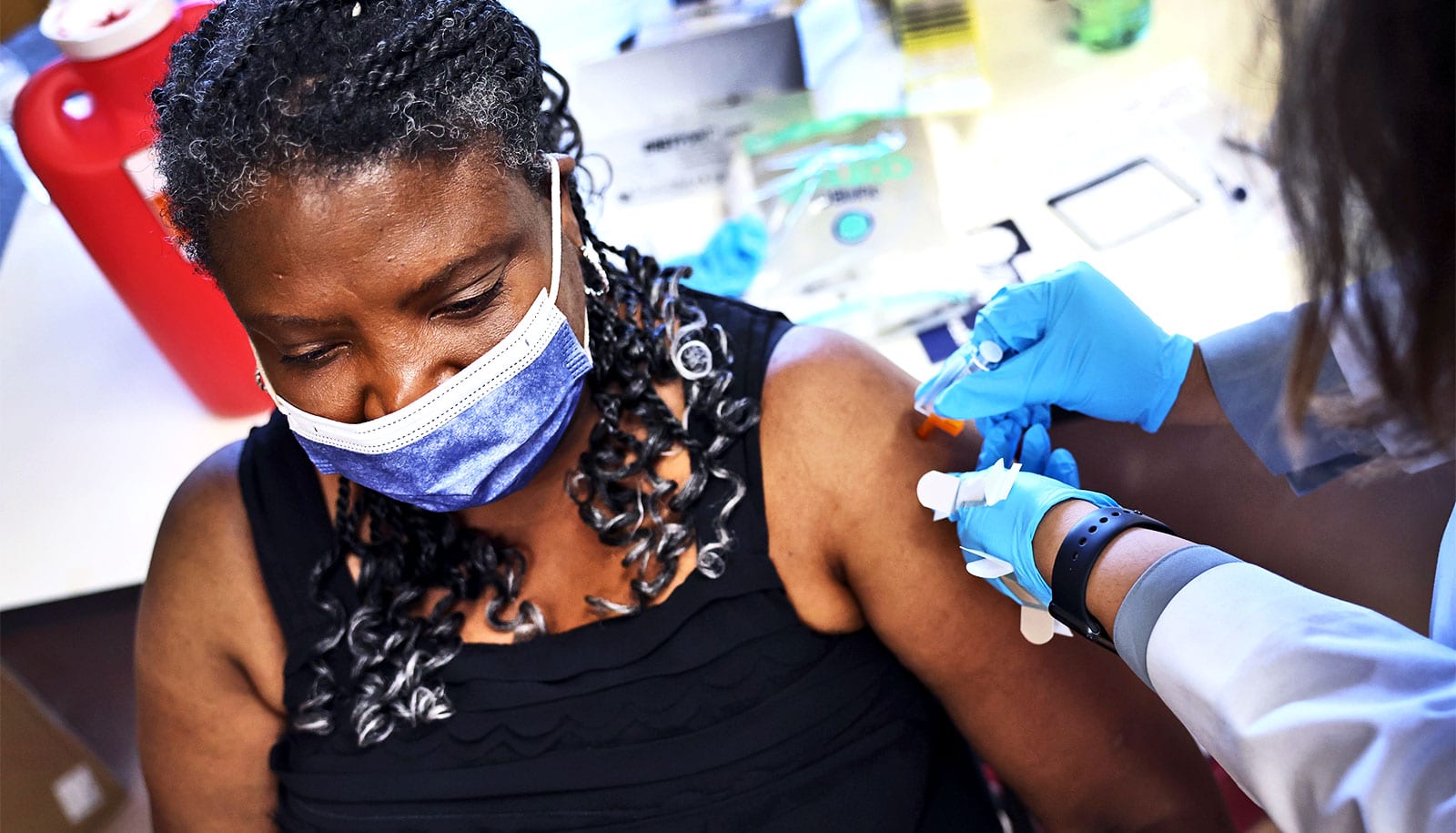
Even two years after infection with the virus, fallout from COVID-19 may persist, researchers report.
In the spring, the US government and the World Health Organization declared an end to the COVID-19 global health emergency. But for millions of people who have been infected with SARS-CoV-2, the pandemic’s legacy of pain, suffering, and daily disruption persists as a debilitating condition known as long COVID.
The new study found that people who had COVID—including those who were hospitalized within the first 30 days following infection and those who were not—were still, up to two years after infection, at an elevated risk for many long COVID-related conditions including diabetes, lung problems, fatigue, blood clots, and disorders affecting the gastrointestinal and musculoskeletal systems.
“For far too many people, the continuing and enduring risk of long COVID and its long-term, adverse effects on health are sober reminders that the pandemic is not in the rearview mirror,” says senior author Ziyad Al-Aly, a clinical epidemiologist at Washington University School of Medicine in St. Louis. “The continuous struggles of people with long COVID are vivid, daily reminders of the detrimental and long-lasting legacy of COVID-19.”
On an encouraging note, however, the researchers noted that during the two-year study period, some COVID-related health risks among the nonhospitalized—the majority of people infected with the virus—declined and became insignificant. Such risks included death, hospitalization, and disorders associated with the brain, heart, kidneys and mental health. For example, risks of death and hospitalization became insignificant at six and 19 months, respectively.
But those hospitalized within 30 days of being infected with the virus fared worse. Two years after infection, their risk of death and hospitalization remained elevated, and their risk of adverse health conditions remained significant across all organ systems.
The study appears in Nature Medicine.
“Our findings highlight the substantial cumulative burden of health loss due to long COVID and emphasize the ongoing need for health care for those faced with long COVID,” says Al-Aly, who treats patients within the VA St. Louis Health Care System.
“It appears that the effects of long COVID for many will not only impact such patients and their quality of life, but potentially will contribute to a decline in life expectancy and also may impact labor participation, economic productivity, and societal well-being.”
Past research by Al-Aly and scientists worldwide has detailed COVID-19’s assault on nearly every human organ, contributing to diseases and conditions affecting the lungs, heart, brain, and the body’s blood, musculoskeletal, and gastrointestinal systems. The new study focused on the risk of death, hospitalization, and 80 different adverse health conditions possible in people with COVID-19 during the two years post-infection.
“Most of what we know about long COVID is limited to research analyzing data of patients six months to a year after initial infection,” Al-Aly says. “Looking beyond the first year after infection and understanding of the longer term health trajectories of people who had COVID-19 is very important and may help inform care strategies for this population.”
The researchers analyzed about 6 million de-identified medical records in a database maintained by the US Department of Veterans Affairs, the nation’s largest integrated health care system. Patients represented multiple ages, races, and sexes.
The researchers created a controlled data set of more than 5.9 million people who did not test positive for COVID-19 infection from March 1, 2020, through December 31, 2020. Using the same time frame, the researchers also compiled a group of 138,818 people who had tested positive for COVID-19. Of the latter, 118,238 represented the nonhospitalized patients, and the hospitalized group numbered 20,580.
The researchers used statistical modeling to examine the health risks associated with the virus two years after infection. Within that time frame, they collected data from those who had COVID-19 and from the noninfected control group at five different periods to determine if and when the risks for 80 long COVID-related conditions had started to decline and equalize with the noninfected control group.
Compared with the control group, the postinfection risks of death and hospitalization among those not hospitalized diminished and became on par with the noninfected control group at six months and 19 months, respectively. Over the two-year span, the risks decreased and became insignificant for 55 (69%) of the 80 long COVID-related conditions studied by researchers.
Among those hospitalized for COVID-19, the risk of death and hospitalization remained elevated two years postinfection as did the risk for 52 (65%) of the 80 long COVID-related conditions.
“This suggests a difficult and protracted road to recovery among those whose disease was sufficiently severe enough to necessitate hospitalization while infected with the virus,” Al-Aly says.
Additionally, researchers measured and compared the number of healthy life-years lost due to COVID-19. They found that among those nonhospitalized, at two years after infection COVID-19 had contributed to 80 lost years of healthy life per 1,000 persons. About 25% of this loss occurred during the second year.
“This 25% is a substantial proportion of an exorbitantly high burden of disability and disease,” Al-Aly says. “This illustrates the long and arduous journey of dealing with the long-term health consequences of the virus. COVID-19 still generates substantial additional risks of health loss even in the second year after infection.”
The researchers found that the number of healthy-life years lost to COVID-19 was significantly higher than with other major diseases in the US. For example, over a lifetime, cancer and heart disease claimed, respectively, 50 and 52 healthy-life years lost per 1,000 people compared to COVID’s 80 in the first two years after infection.
“It is possible the burden of disability and disease due to long COVID may increase as we continue to study the virus’s long-term health effects,” Al-Aly says. “These figures at two years already show a staggeringly high burden. What’s more, unlike cancer and heart disease, there is no treatment yet for long COVID.”
Steps to decrease the risk of long COVID should be a major focus of public health policy, Al-Aly says. “Reducing the risk of infection and transmission with updated vaccines—including vaccines that block transmission—may be a critical strategy to reduce the risk of long-term health problems,” he says. “We also need an urgent, coordinated approach that matches the scale and gravity of long COVID to find treatments as soon as possible.”
Funding for this research came from the US Department of Veterans Affairs.