New research offers the first details of how enteroviruses—which cause millions of infections worldwide each year—enter the body through the intestine.
Enterovirus infections are associated with diseases that can range from mild flu-like symptoms to much more severe outcomes such as inflammation in the brain or heart, acute paralysis, and even death. Enterovirus infections acquired within neonatal intensive care units can be devastating as newborns are particularly susceptible to infection by these viruses.
They are the second most common human infectious agents and are primarily transmitted through close person-to-person contact, touching infected surfaces, or ingesting food or water containing the virus.
“Despite their major global impact, especially on the health of children, little is known about the route that these viruses take to cross the intestine, their primary point of entry. Our approach has for the first time shed some light on this process,” says senior author Carolyn Coyne, associate professor of microbiology and molecular genetics at the University of Pittsburgh School of Medicine.
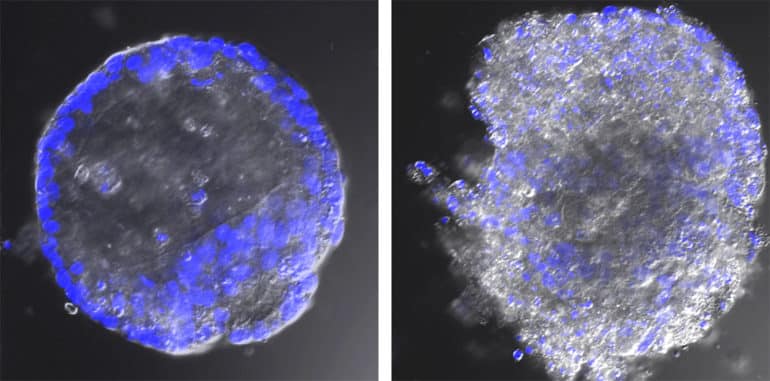
In the study, researchers isolated stem cells from premature human small intestines and grew them in the laboratory into enteroids, or so-called “mini-guts,” which contained the different cell types and tissue structures that are normally found in the human intestine.
New clues to why intestines of preemies stop working
Using the mini-gut model, they demonstrated that echovirus 11 (E11), the enterovirus most commonly associated with NICU infections, induced significant damage to the enteroids, which could facilitate passage of the virus into the bloodstream from the infected intestine.
The results also provided the first evidence that different types of enteroviruses could target distinct cells within the gastrointestinal tract and might vary in their effectiveness at infecting intestinal cells.
“This study not only provides important insights into enterovirus infections, but also provides an important model that could be used to test the efficacy of anti-enterovirus therapeutics in the premature intestine,” says Misty Good, assistant professor of pediatrics at the Washington University School of Medicine in St. Louis and co-senior author of the study.
The National Institutes of Health, the Burroughs Wellcome Fund, and Children’s Hospital of Pittsburgh of UPMC supported the work, which appears in the Proceedings of the National Academy of Sciences.
Source: University of Pittsburgh