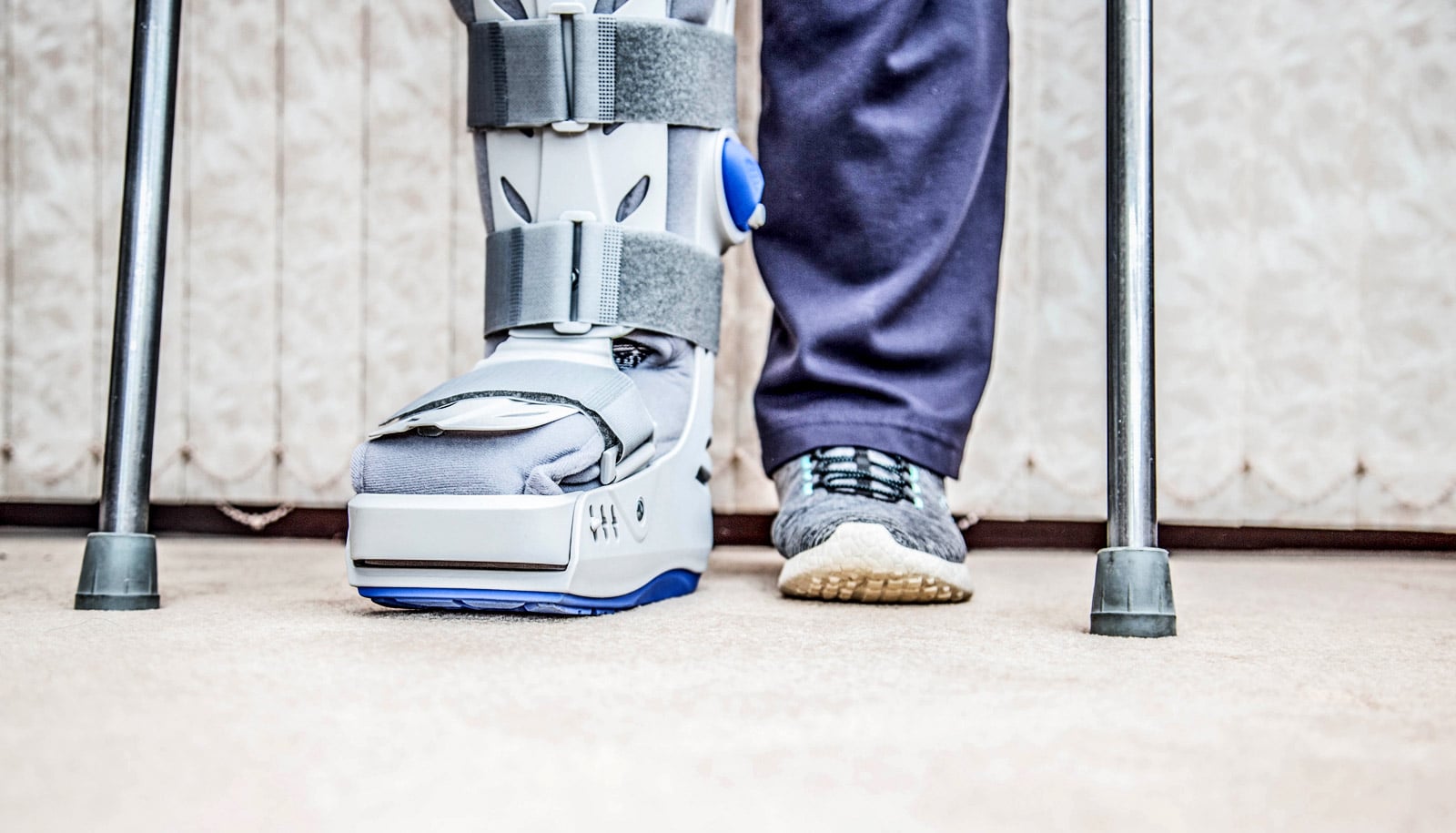
Most older people hospitalized for hip fracture surgery carried biomarkers of developing Alzheimer’s disease even though they had no clinical signs of dementia, according to a new study.
The results add to evidence that brain alterations that lead to poor balance in older people may underpin both increased risk of hip-fracturing falls and Alzheimer’s, and that hip fracture itself may serve as a first sign of undiagnosed disease, researchers say.
“We studied a group of patients without a clinical diagnosis of dementia, meaning that many of our study participants were active and living independently without overt signs of Alzheimer’s disease,” says Esther Oh, associate professor of medicine at Johns Hopkins University and associate director of the university’s Memory and Alzheimer’s Treatment Center.
The study doesn’t suggest that every older person with a hip fracture has Alzheimer’s, Oh says. But it does suggest that people facing hip repair surgery after a fall be monitored closely for post-operative delirium or other mental or cognitive problems, because some may have underlying Alzheimer’s disease.
What else is going on?
More than 5.5 million people in the United States—most over 65—have Alzheimer’s disease, according to National Institute on Aging estimates.
Several previous studies have shown that up to a quarter of older adults hospitalized for hip fracture surgery are likely to die within a year, suggesting a serious medical condition may have been simmering undiagnosed prior to the falls that sent those patients to the hospital, Oh says.
The new study, which appears in PLOS ONE, was in part a response to results of Johns Hopkins research published last year which found that 34 percent of hip fracture patients develop delirium during their hospital stay. Delirium characteristics include restlessness, delusions, and incoherent thoughts and speech.
Because patients with Alzheimer’s disease are more likely to experience these symptoms, and because of the higher than normal mortality rate associated with hip fracture, Oh and colleagues designed a study to directly test hip fracture patients for Alzheimer’s disease biomarkers.
Over almost five years, they recruited 200 hip fracture patients admitted to Johns Hopkins Hospital and Johns Hopkins Bayview Medical Center.
Participants were an average of 82 years old, ranging from 65 to 102. The study included only hip fracture patients who received spinal (local) anesthesia before surgery, so that doctors could collect spinal fluid samples at the time of anesthetic injection.
Researchers tested spinal fluid samples for elevated levels of commonly accepted biomarkers of Alzheimer’s and other neurodegenerative diseases, including the proteins amyloid beta 42 (Aβ42), Aβ40, tau, and tau with a phosphate chemical group attached (p-tau).
The amyloid proteins and tau appear in tangled clumps in nerve cells and in plaques that form in the brains of people with advanced Alzheimer’s. High levels of p-tau indicate brain injury or other types of brain cell damage.
Clinical dementia
Before surgery, participants also completed standard tests of mental state, memory, and cognition. On the basis of those results, participants received Clinical Dementia Ratings. A score of 0 meant completely healthy (70 participants) and 0.5 indicated mild cognitive symptoms (81 participants). A score of greater than 1.0 indicated early dementia (13 participants) and a score of 2.0 meant moderate dementia (four participants).
When researchers looked at biomarker levels in the group with a rating of 0, they found 62 out of 70 patients, or 88.6 percent, had abnormal levels of at least one of the Alzheimer’s biomarkers. In the group with a score of 0.5, 80 of 81 participants had abnormal levels in one of the biomarkers.
The researchers ruled out older age as a factor skewing their results; normally 23 to 32 percent of people between 65 and 74 years old have abnormal Aβ levels. In the hip fracture patients, however, 68 percent of people in this same age range with a Clinical Dementia Rating of 0 had abnormal levels of Aβ.
Oh’s group plans to monitor study participants for a year after surgery to document progression and clinical dementia ratings.
Additional researchers are from Johns Hopkins and Harvard Medical School. The Johns Hopkins Institute for Clinical and Translational Research, funded in part by the National Center for Advancing Translational Sciences, the National Institute on Aging, the Rosalinde and Arthur Gilbert Foundation, the Roberts Gift Fund, the Swedish and European Research Councils, the UK Dementia Research Institute, and Swedish State Support for Clinical Research, funded the work.
Source: Johns Hopkins University