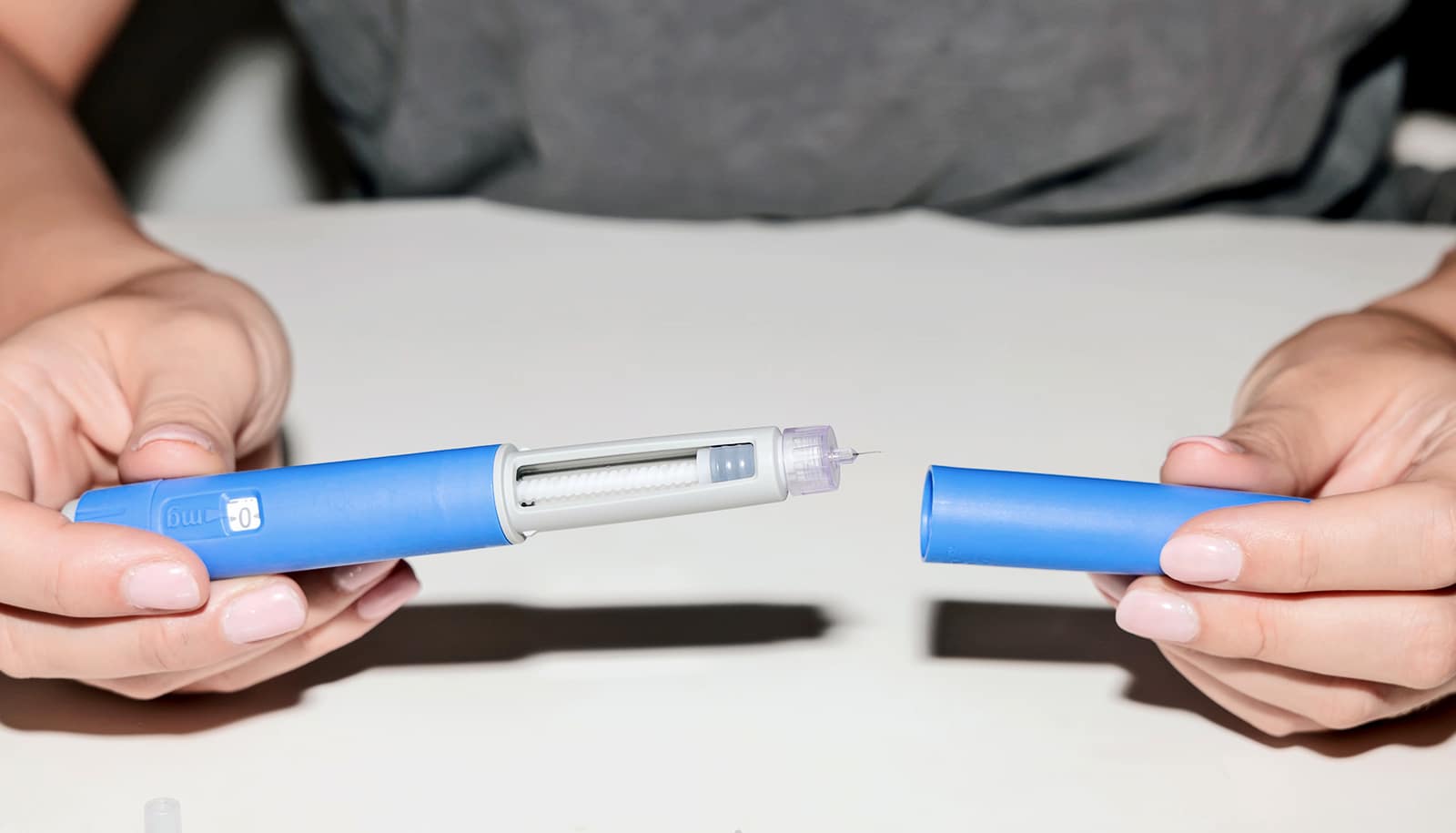
The implications of high prices for new diabetes and obesity therapies are alarming, according to researchers.
For years, Kasia Lipska, associate professor of medicine (endocrinology) at Yale School of Medicine (YSM), has been advocating for affordable pricing of insulin, an essential—and sometimes lifesaving—drug for many individuals with diabetes.
Now, she is turning her attention to a similar trend of soaring prices among new diabetes and obesity medications.
The implications of exorbitant prices for these therapies are alarming, according to Lipska, who first became aware of the drug pricing issue in 2016 when one of her patients couldn’t afford to increase the dose of insulin she was taking. In subsequent research, Lipska discovered that 1.1 million Americans, or 14% of those who filled insulin prescriptions, reached catastrophic spending, defined as spending more than 40% of post-subsistence income on insulin alone.
The same insulin and other medications for diabetes and obesity are frequently priced 10 times higher in the US than in peer countries, Lipska says.
In a new paper in Diabetes Care, Lipska, Reshma Ramachandran, assistant professor of medicine (general medicine) at YSM, and first author Kathryn Nagel, former YSM internal medicine department resident, used findings from previous research on insulin pricing to look at the issues underlying drug affordability.
“As with insulin, our patients are facing parallel challenges in accessing other new non-insulin diabetes and anti-obesity medications,” Ramachandran says.
In their research and analysis, Lipska, Ramachandran, and Nagel gathered evidence about the changes needed to achieve fair pricing of new diabetes and obesity drugs, creating a blueprint that policymakers can use for potential action.
“Writing the article helped us map out the different pieces that go into the drug pricing process in the US,” Lipska says. “We learned more about the complex chain of events that leads from drug development and patent law to how much patients pay when the medicine gets to them.”
“Our paper highlights where along the drug development and delivery value chain there is more work yet to be done by policymakers to enable more equitable and affordable access to these medications,” Ramachandran adds.
Ramachandran notes a key lesson learned from efforts to improve access to insulin is that there is no single silver bullet. “Our paper shows that a range of upstream and downstream policies are necessary,” she says.
But there are challenges to policy reform, the researchers observe.
“While the recent Inflation Reduction Act includes several policies to lower prescription drug prices, including for those used in diabetes treatment, the legislation also has serious limitations in providing relief for patients, particularly for novel, transformative treatments,” Ramachandran says.
Lipska points to the power of US corporations as another obstacle to drug affordability.
“Many patient advocacy groups, educational events, and even professional societies that clinicians are a part of are in some way influenced or supported by the pharmaceutical industry,” she says.
Still, the issue is gaining traction, Lipska says. She notes a growing awareness of the need to address the drug pricing crisis through state and federal intervention and of the role clinicians can play in advocating on behalf of their patients.
“There are a lot of policies targeting drug affordability that have recently been proposed or enacted into law,” she says. “Clinicians can give feedback about how certain solutions are playing out in practice and bring an important perspective to this conversation.”
Source: Serena Crawford for Yale University