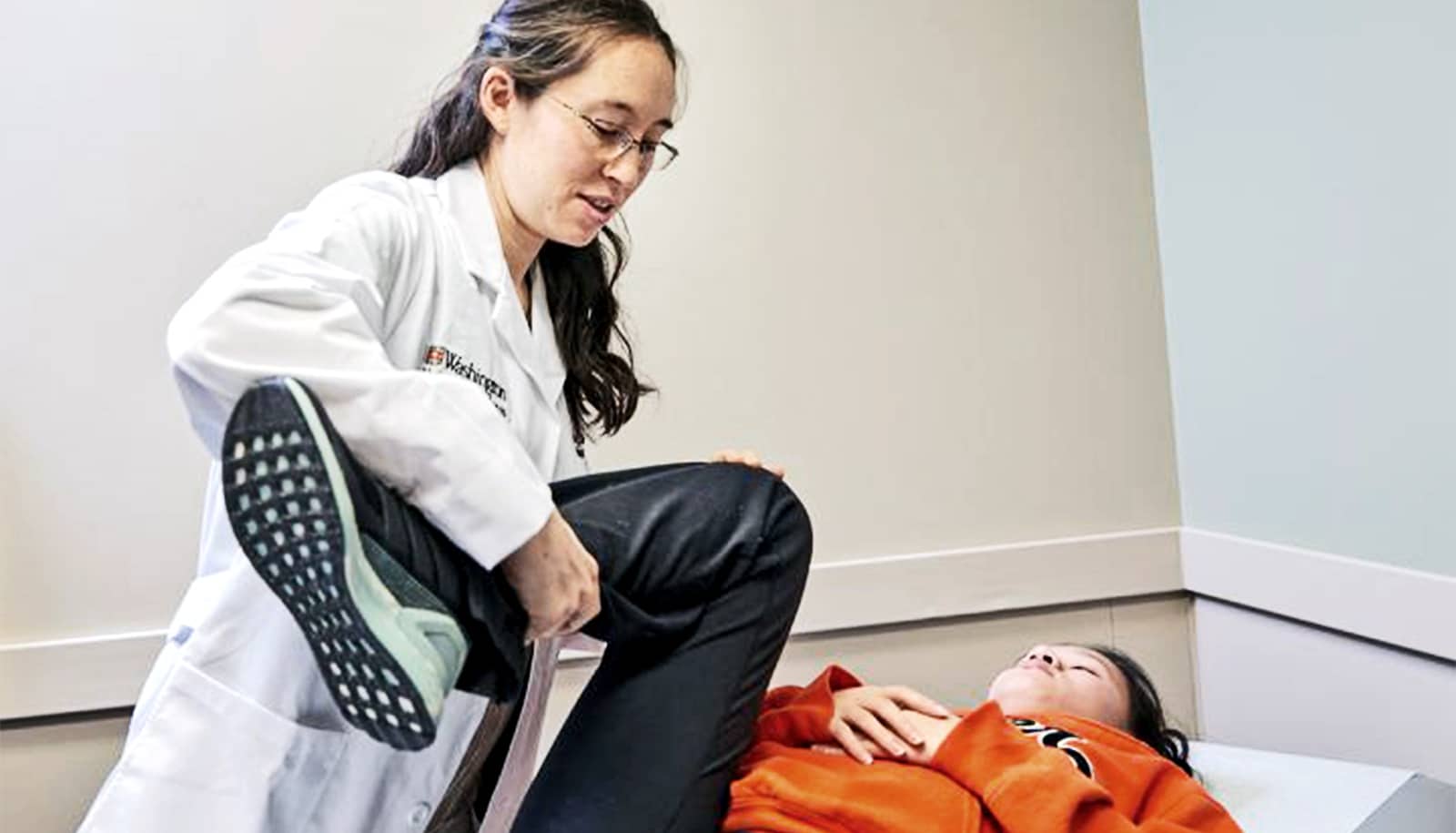
Clinical depression and anxiety can have a negative impact on outcomes following hip surgery, such as pain, slower recoveries, and inadequate return to activity, according to new research.
In one of the first large studies to focus on mental health effects associated with hip pain, the researchers analyzed data gathered in 12 smaller studies conducted since 2014.
The results suggest it may be advisable to start screening young patients with hip pain for depression and anxiety, especially before they undergo arthroscopic hip procedures.
Checking for depression and anxiety before surgery
“In a perfect world, we would screen patients for anxiety and depression before surgery and offer treatment, if needed,” says first author Abby L. Cheng, an assistant professor of orthopedic surgery at Washington University School of Medicine in St. Louis. “But that’s not usually what happens with these patients right now. Plus, many patients think that if their pain goes away, their anxiety or depression will go away, too. But that doesn’t seem to be the case.”
Cheng, a physiatrist trained in physical medicine and rehabilitation, works with patients who have hip pain, but she does not perform hip surgery herself. She analyzed data from more than 5,600 hip surgery patients, ages 29 to 41.
All of the studies in the analysis included evaluations of the effects of depression or anxiety on postsurgical clinical outcomes, such as use of pain-killing drugs after an operation, return to pre-surgery activities, and overall patient satisfaction following surgery. In every study, patients with anxiety and depression prior to surgery were statistically less likely to have good outcomes after their operations.
All of the patients had undergone arthroscopic surgery to correct hip problems, the most common of which was femoroacetabular impingement, a condition in which the hip socket is too deep, causing the thigh bone to rub against the socket. The condition can be painful and can significantly increase arthritis risk and the need for eventual hip-replacement surgery. Cheng says patients with these hip problems also often have unexpectedly high rates of depression and anxiety.
“There are people who may have anxiety or depression, who then develop a hip problem, and that can make things worse because rather than having the mindset that the hip problem is a small, fixable issue, their extra worry actually can increase the impact of the hip problem on their lives,” she says.
“Or sometimes people who have hip problems may then develop new depressive or anxious symptoms because their hip issues are preventing them from doing things they want and need to do. That combination of things can play a role in making each of the problems worse.”
Mind and body connection
In all of the studies reviewed, the patients were otherwise healthy and active before being limited by hip pain. The patients in the studies were young primarily because of the type of hip surgery studied. Older patients tend to be candidates for more extensive operations, such as hip-replacement surgery. But in younger patients, doctors often perform arthroscopic procedures to correct defects, attempting to delay or prevent the need for total joint-replacement operations that are so common in older adults
“These young people often were involved in sports activities such as soccer or dance, but their pain prevented them from participating in these things they had enjoyed,” Cheng says. “Often those activities are good outlets for stress, so the inability to participate affects quality of life.”
Doctors who treat young hip patients don’t routinely screen for depression or anxiety, much less refer their patients to behavioral health services as part of the treatment plan for hip pain. But Cheng now proposes research into accessible, affordable behavioral-health interventions for these patients, especially before considering hip surgery.
“We need to start screening for symptoms of psychological impairment, and we need to be able to offer our high-risk patients easier access to behavioral health professionals,” Cheng says.
“There’s an understanding, for example, that back pain is associated with stress, but we’re just now starting to examine the relationships between anxiety and hip pain, as well as shoulder pain or pain in other parts of the body. The more we look at it, the more it becomes clear that the mind and the body are connected, and we can’t separate them and treat one without treating the other.”
The findings appear in the American Journal of Sports Medicine.
Funding for the work came from the Washington University Department of Orthopaedic Surgery.