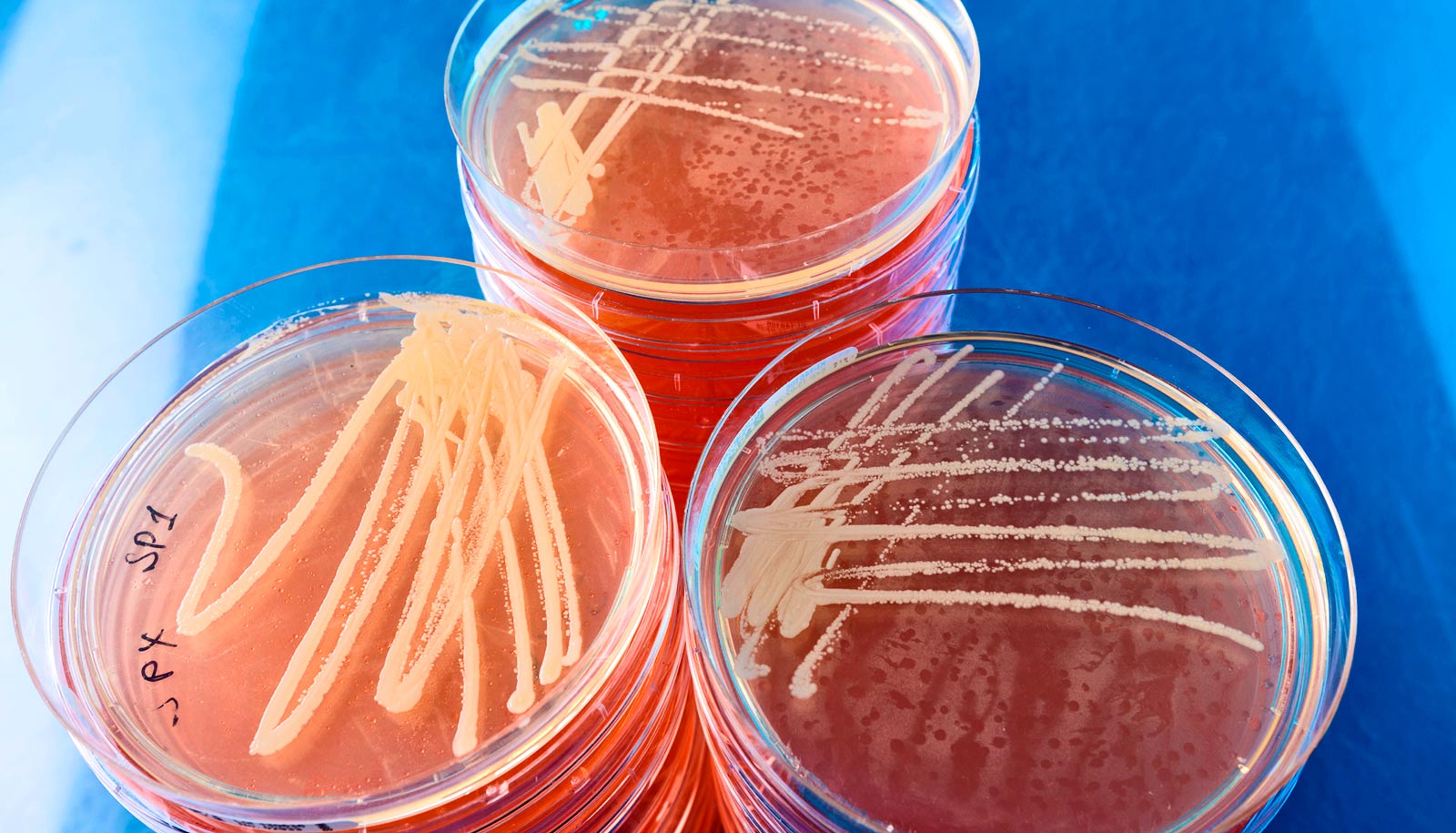
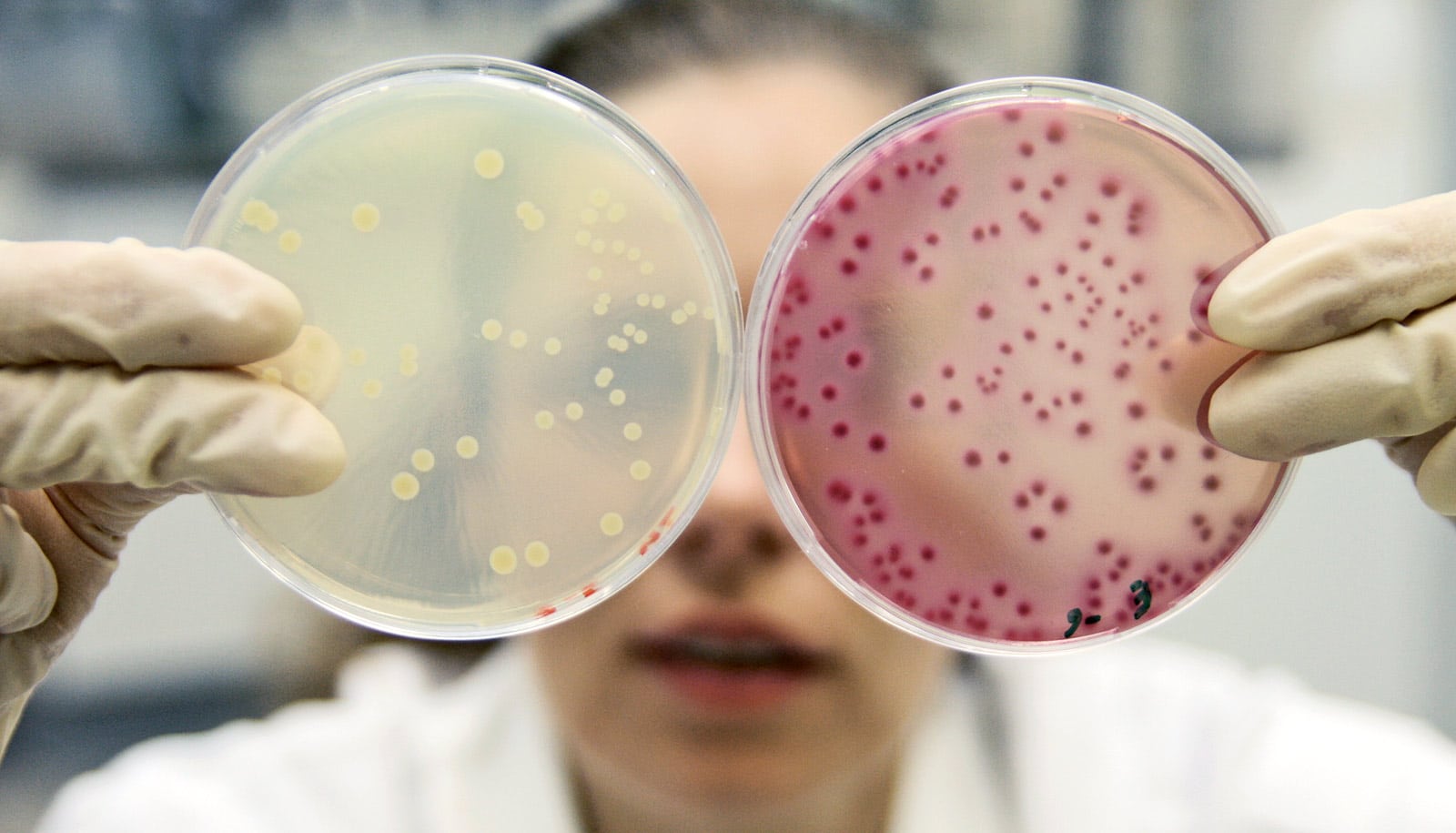
To combat the rise of drug-resistant bacteria, researchers are examining how one superbug adapts to fight an antibiotic of last resort.
Scientists say they tracked the biochemical changes that the superbug vancomycin-resistant Enterococci (VRE) undergo as they adapt to fight the antibiotic, daptomycin, hoping they’ll find clues that prolong the drug’s effectiveness.
“We need to get to a stage where we can anticipate how these pathogens will become resistant to antibiotics so we can stay one step ahead of them,” says Yousif Shamoo, a professor of biochemistry and cell biology in the biosciences department at Rice University and coauthor of a new paper in Antimicrobial Agents and Chemotherapy showing that VRE can develop resistance to daptomycin in more than one way.
The stakes are high, researchers say. In 2014, the World Health Organization reported that antibiotic-resistant infections were on pace to kill 10 million people per year worldwide by 2050.
VRE is one of the nation’s leading antibiotic resistance threats, according to the US Centers for Disease Control, which estimates it will infect some 20,000 people in the US this year and kill 1,300 of them.
Daptomycin first became available in 2003 and is one of the last drugs doctors can use to fight multidrug-resistant superbugs like VRE, methicillin-resistant Staphylococcus aureus (MRSA), and glycopeptide-resistant enterococci (GRE).
Unfortunately, health officials documented cases of daptomycin resistance as early as 2005, and the number of cases is on the rise worldwide.
One of the principle findings of the new study is that a specific strain of VRE, Enterococcus faecium, has an unusually diverse set of strategies for resisting antibiotics like daptomycin. That diversity can make treatment of infections even more difficult, researchers say.
“By understanding how these pathogens acquire resistance, we can develop new treatment strategies or new ‘co-drugs’ that target their ability to become resistant,” Shamoo says.
Researchers could administer these combination drugs that target the evolution of resistance with antibiotics like daptomycin to both help patients fight off infection and stem the spread of increasingly resistant strains of bacteria in hospitals, Shamoo says.
Lead author Amy Prater, who graduated from Rice in July, showed that the same strain of VRE could activate different biochemical pathways to activate up to three strategies, depending upon its environment.
The multipronged strategy will make it more difficult for health officials to fight growing daptomycin resistance in VRE, but the results help clear up previously confusing experimental findings about VRE resistance, which is a step in the right direction, Shamoo says.
“If we understand how a pathogen acquires resistance, we can anticipate its next move, and hopefully act beforehand to cut it off. Predictability is the key.”
Additional coauthors are from Rice and the University of Texas Health Science Center at Houston. The National Institutes of Health supported the work.
Source: Rice University