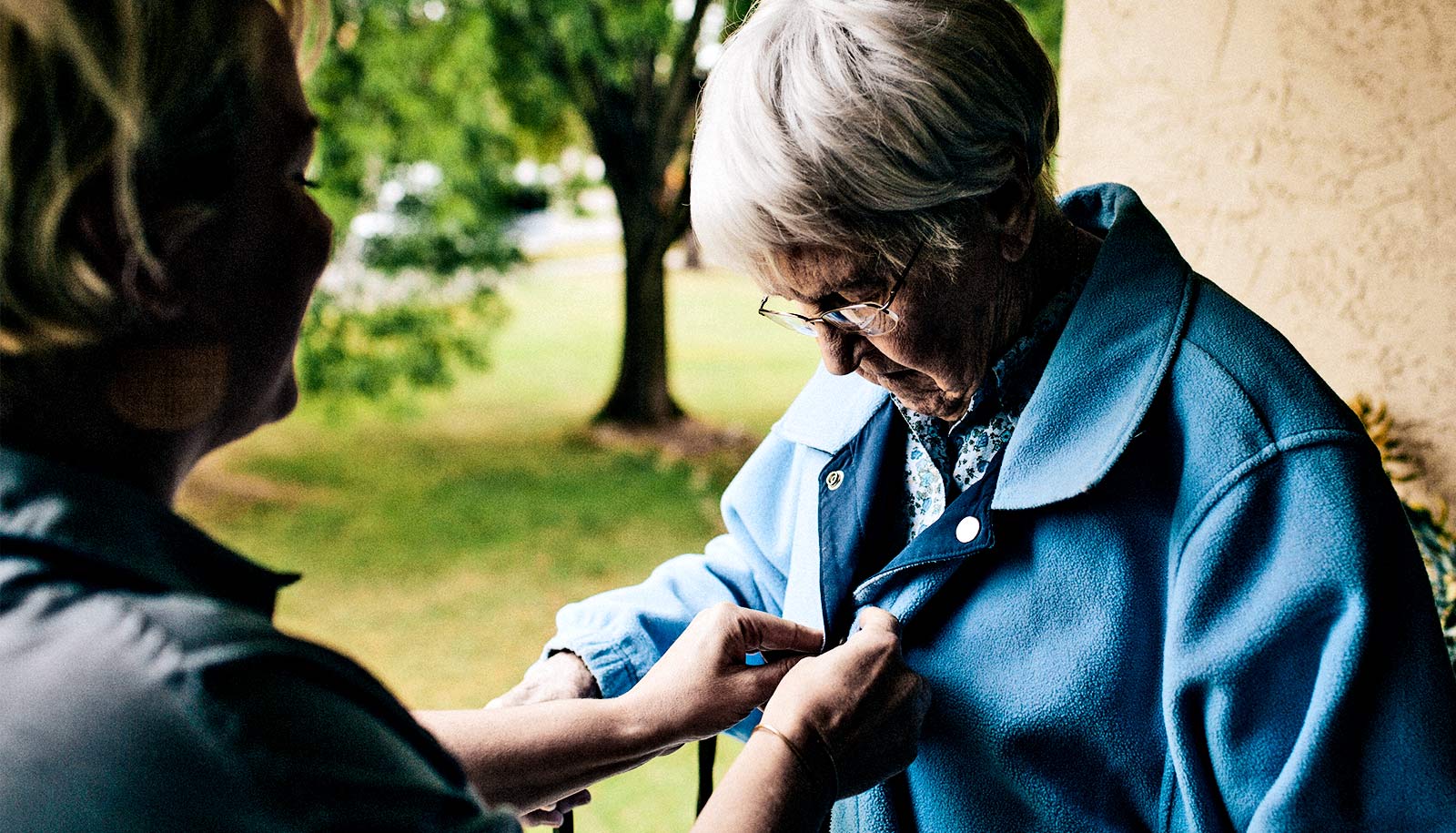
Family caregivers often struggle with medical and nursing tasks as well as navigating the complex health care system, according to a new study.
Resources like home health care nurses or aides can, however, serve as a central point-of-contact to improve coordinated care, the research suggests.
After Jo-Ana Chase, associate professor in the University of Missouri’s Sinclair School of Nursing, heard her mother had successful heart surgery, she was relieved when her mom finally returned home from the hospital in the care of her brother.
However, she quickly learned her brother felt lost on the best ways to care for their mom due to confusing discharge instructions from the hospital and logistical challenges related to home health care services like wound care and medication management.
Motivated by her own family’s struggles navigating the often complicated American health care system, Chase is working with clinicians and health care providers to better engage family caregivers in providing coordinated care after a loved one returns home from the hospital.
In the new study, she sought to better understand the resources family caregivers currently use to help health care providers identify gaps in coverage and recommend resources to assist overburdened caregivers and ultimately improve and better coordinate care.
“The American health care system has been very patient-focused; however, we also need to remember that patients often rely on family for help with their care,” Chase says.
“Now that we are starting to recognize how impactful the work is that family caregivers provide, my goal is to better engage these family caregivers and help them access the resources they need to better support the loved ones they care for.”
Chase interviewed family caregivers about the medical and nursing tasks they completed for a loved one after a hospital-to-home transition, such as treating wounds or giving medication, and found that many caregivers needed more support.
“After a patient is discharged from the hospital, a home health care nurse will often come to the patient’s home periodically to check in, make sure the medications are right, evaluate the home for safety, check the patient’s vital signs and assess wounds,” Chase says. “This is an excellent opportunity for the clinicians to work with caregivers to address any questions, challenges, or concerns family caregivers may be having.”
Further, while caregivers may receive discharge instructions for providing care after a patient leaves the hospital, the instructions may fail to consider caregivers’ preparedness and various environmental factors, such as what equipment is needed, or which room in a house is best for administering a specific task like changing a bandage.
In addition to home health care nurses, primary care providers, social workers, nearby community centers, and respite services can also help support and take the load off of overburdened caregivers.
“At some point in our lives, most of us will become a caregiver for someone, whether it is a child, spouse, parent, or relative,” Chase says. “So, encouraging the health care system to effectively engage caregivers benefits us all. I hope one day when I am sick and someone has to take care of me, my caregiver doesn’t experience the same challenges my brother did caring for my mom.”
The study appears in the Journal of Applied Gerontology. The Eugenie and Joseph Doyle Research Partnership Fund of the Visiting Nurse Service of New York funded the work. The content is solely the responsibility of the authors and does not necessarily represent the official views of the funding agency.
Source: University of Missouri