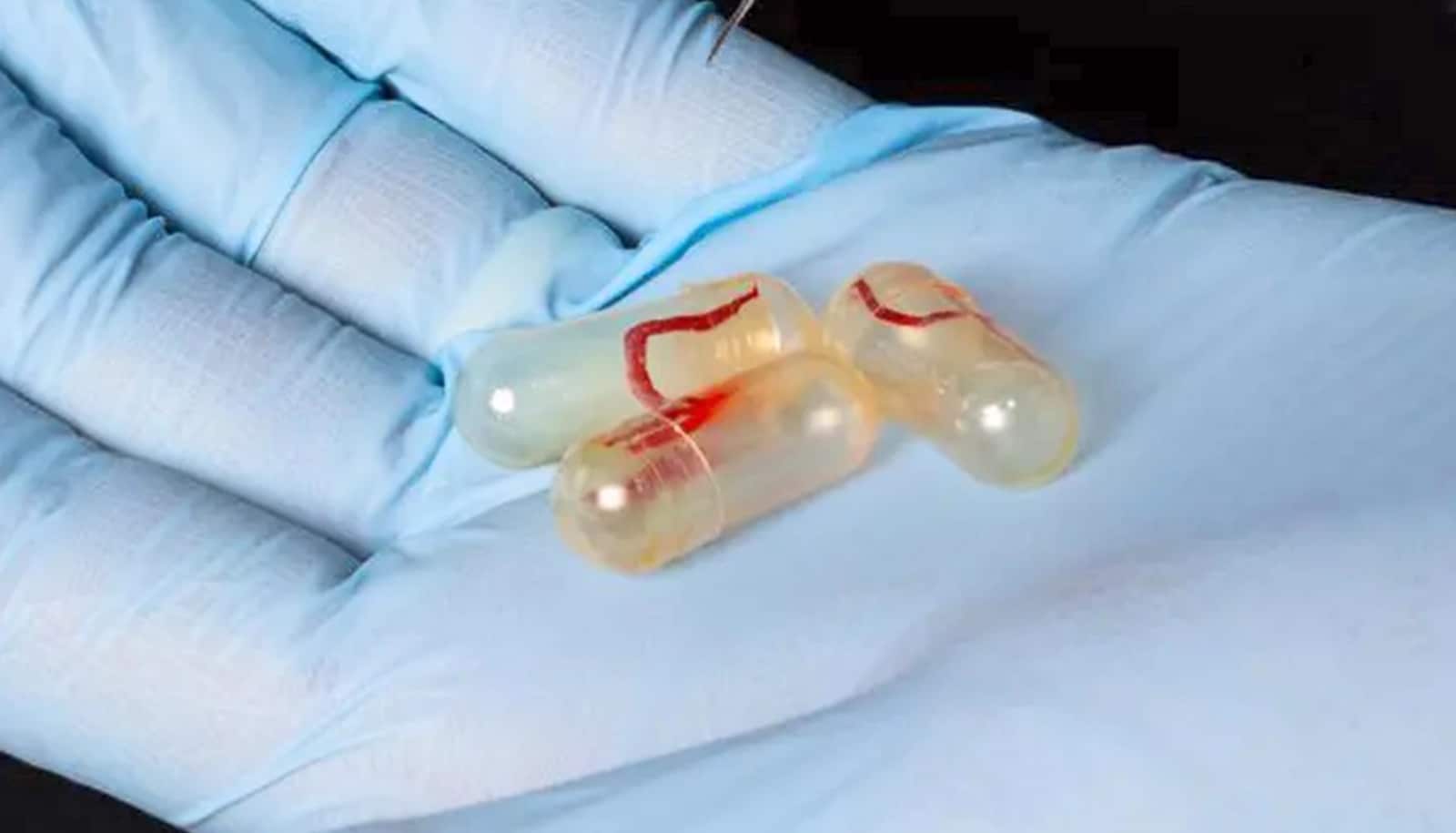
Biomedical engineers are using pulses of ultrasound to help deliver tiny amounts of a drug to small targets in the brain.
The method—recently tested in rats—involves “caging” a drug with tiny biodegradable nanoparticles. When the particles reach the right place in the brain, precisely targeted high-frequency sound break them up and release the drug.
“If further testing of our combination method works in humans, it will not only give us a way to direct medications to specific areas of the brain, but will also let us learn a lot more about the function of each brain area,” says Jordan Green, associate professor of biomedical engineering at Johns Hopkins University.
The method should minimize side effects, researchers say. Because a drug could be targeted to a small area, the total amount of drug used could be much lower, often below the level at which annoying or dangerous side effects occur.
Why these brain tumor drugs miss the mark
And because elements used in this technique are already proven safe in people, researchers believe the method could be in clinical use more quickly than usual. They hope to start regulatory approval within a year or two.
The brain is a delicate and challenging organ to treat, Green says. To protect itself from infections and from swelling caused by the immune system, the brain is surrounded by a molecular “fence” called the blood-brain barrier.
“In humans, ultrasound machines can target a volume as small as a few millimeters cubed, less than one ten-thousandth of the brain.”
It lines every blood vessel feeding the brain. Only very small drug molecules that dissolve in oil can get through the BBB. Most drugs developed for brain disorders fit those criteria, but, with current delivery methods, are released not only in target areas but also in areas throughout the brain and body where they are unneeded and unwanted.
This shotgun nature of current drug delivery methods limits doctors’ treatment options, says Raag Airan, a radiologist at Stanford University and coauthor of the paper.
“When working with a patient who has post-traumatic stress disorder, for example, it would be nice to quiet down the overactive part of the brain—for instance, the amygdala—during talk therapy sessions. Current technologies can at best quiet down half of the brain at a time, so they are too nonspecific to be useful.”
As reported in the journal Nano Letters, Green’s group designed nanoparticles with an outer expandable “cage” made of biodegradable plastic. The particles form an expandable sphere that can carry a drug, in this case propofol, an anesthetic used to treat seizures.
The center of the cage is filled with liquid perfluoropentane. When ultrasound waves—delivered noninvasively through a rat’s scalp and skull—strike the liquid, it turns to gas. That expands the surrounding cage and lets the propofol escape.
Before testing in animals, researchers fine-tuned the protocol in plastic tubes, seeking the right ultrasound power and frequency to release adequate amounts of drug without damaging the BBB.
Device delivers drug to brain by remote control
They then gave rats a drug that causes seizures, followed by the propofol-laden nanoparticles. Using MRI, they targeted ultrasound pulses to a precise area in the rat brain and released the drug from nanoparticles floating through blood vessels there. As soon as they applied the ultrasound, the rats’ seizures calmed down.
“These experiments show the effectiveness of this method to manipulate the function of brain cells through the precise delivery of drugs,” says Green. “In humans, ultrasound machines can target a volume as small as a few millimeters cubed, less than one ten-thousandth of the brain.”
Airan, who was at Johns Hopkins during the study, says another application could be the “brain mapping” required in many neurosurgeries. Before removing a tumor, for example, a surgeon needs to know where not to cut.
“That requires keeping the patient awake, while the surgeon exposes the brain and probes it with electrodes while assessing responses,” Airan says. “The ultrasound method would allow us to use a drug like propofol to briefly ‘turn off’ specific areas of the brain one at a time, prior to the surgery, with nothing more invasive than a needle stick.”
The National Institutes of Health, Philips Inc., the Foundation of the American Society for Neuroradiology, the National Science Foundation, Achievement Rewards for College Scientists, and the Walter and Mary Ciceric Foundation funded the work.
Source: Johns Hopkins University