The number of hours an obstetrician has been on the clock before an unscheduled delivery significantly influences risks to the mother and unborn baby, researchers report.
Previous studies have considered adverse outcomes in relation to the day of the week and the time of the day at which the delivery occurred, but this is the first study to examine where the delivery falls during a doctor’s shift and how that timing leads to increased risks.
James Scott, an associate professor of statistics at the McCombs School of Business at the University of Texas at Austin, says that he and his fellow researchers hypothesized that the total number of hours worked during a shift may be a more important predicator of adverse outcomes than whether the delivery occurred during the weekend or in the middle of the night.
The researchers looked at 24,506 unscheduled deliveries in the United Kingdom from January 2008 to October 2013. The obstetricians, all from the same labor and delivery ward, worked 12-hour shifts, and this scheduling pattern remained consistent throughout the study period.
The researchers found no significant differences in the rates of commonly occurring adverse outcomes between day versus night shifts, weekday versus weekend deliveries, vaginal or c-section deliveries, or whether a junior or more senior doctor oversaw the delivery.
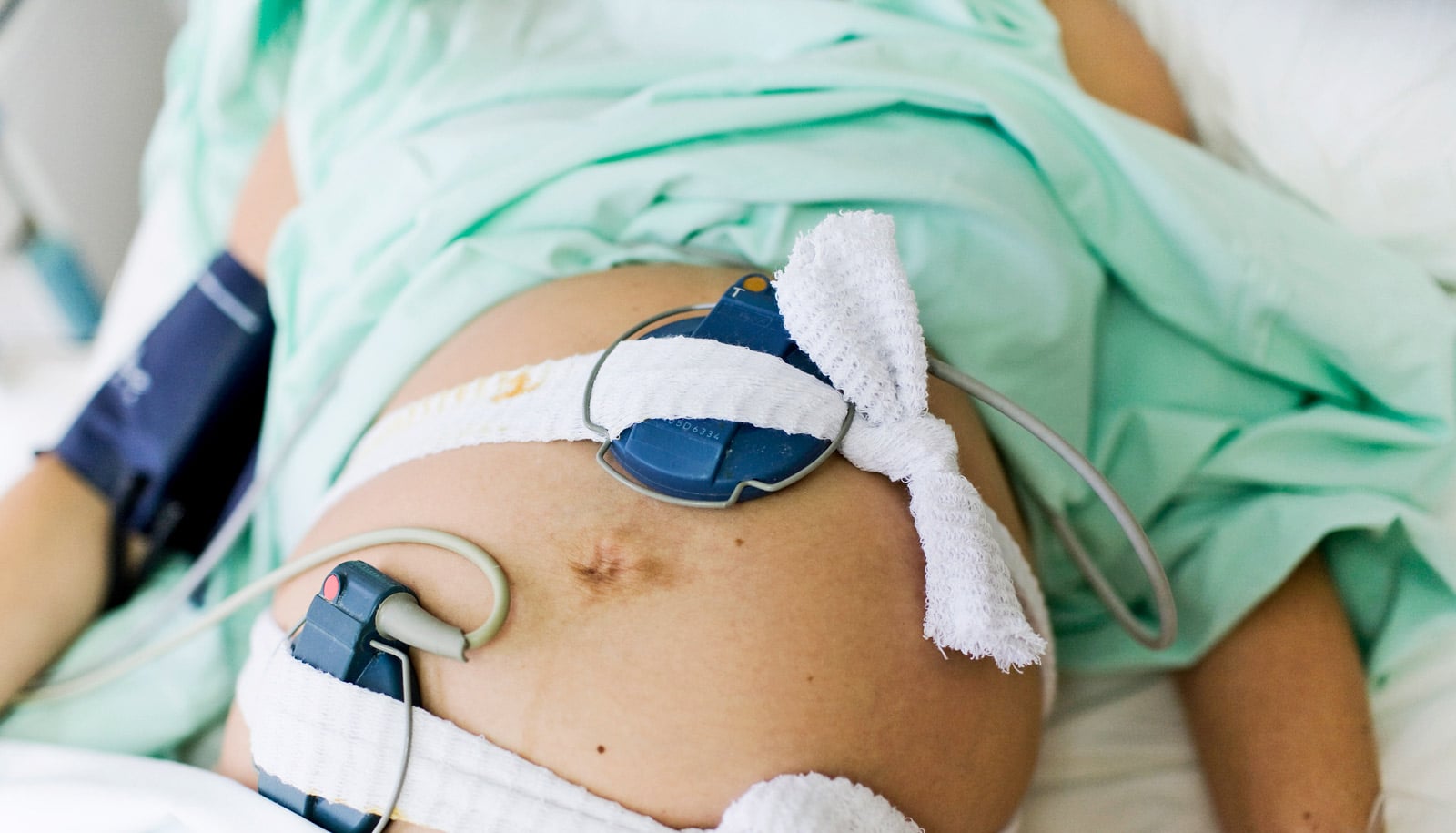
Instead, they found that two specific adverse outcomes—maternal blood loss and fetal acidosis, or low blood oxygen levels in an unborn baby—increased significantly when a physician entered the 9th hour of a 12-hour shift.
“There are all sorts of studies about the timing of deliveries, but what nobody had looked at before is whether there is there some kind of proxy for how fatigued the doctors are,” Scott says. “We find that there’s a peak eight to 10 hours after the beginning of a shift when, relative to baseline, the risk of maternal blood loss exceeding 1.5 liters increases by 30 percent, and arterial pH, a marker for infant distress, is at increased risk of falling below 7.1.”
Doctors without ‘me time’ are a lesson for us all
Normal arterial pH is between 7.3 and 7.4. The researchers hypothesize that fatigue led doctors to miss small fetal distress signals. Scott says ideally, those would have been caught if the doctors were just a little bit fresher and sharper.
The researchers also found that maternal blood loss and fetal acidosis risks actually dropped in the last two hours of doctors’ shifts, when they’d likely be the most fatigued. After consulting with study participants, the researchers surmised that the drop in risk level is likely due to doctors deferring more complicated and high-risk, but non-emergent, cases for the next shift.
Scott says the study shows that patient outcomes aren’t always clinical; they can also be operational, and staffing decisions are part of that.
The study appears the American Journal of Obstetrics and Gynecology.
Source: University of Texas at Austin